Journal of Southern Medical University ›› 2026, Vol. 46 ›› Issue (3): 592-603.doi: 10.12122/j.issn.1673-4254.2026.03.13
Previous Articles Next Articles
Xuejun CHEN1( ), Yuan JING2, Huiyu LIANG1, Jingying ZHONG1, Zedong CHEN1, Yuzhi PENG1, Jiaojiao DAI2(
), Yuan JING2, Huiyu LIANG1, Jingying ZHONG1, Zedong CHEN1, Yuzhi PENG1, Jiaojiao DAI2( ), Ya XIAO1(
), Ya XIAO1( )
)
Received:2025-09-17
Online:2026-03-20
Published:2026-03-26
Contact:
Jiaojiao DAI, Ya XIAO
E-mail:1962889575@qq.com;djj52092@smu.edu.cn;xiaoya0527@126.com
Supported by:Xuejun CHEN, Yuan JING, Huiyu LIANG, Jingying ZHONG, Zedong CHEN, Yuzhi PENG, Jiaojiao DAI, Ya XIAO. Different Astragalus medicinal pairs improve diabetic nephropathy in mice by regulating lipid peroxidation through PTGS2[J]. Journal of Southern Medical University, 2026, 46(3): 592-603.
Add to citation manager EndNote|Ris|BibTeX
URL: https://www.j-smu.com/EN/10.12122/j.issn.1673-4254.2026.03.13
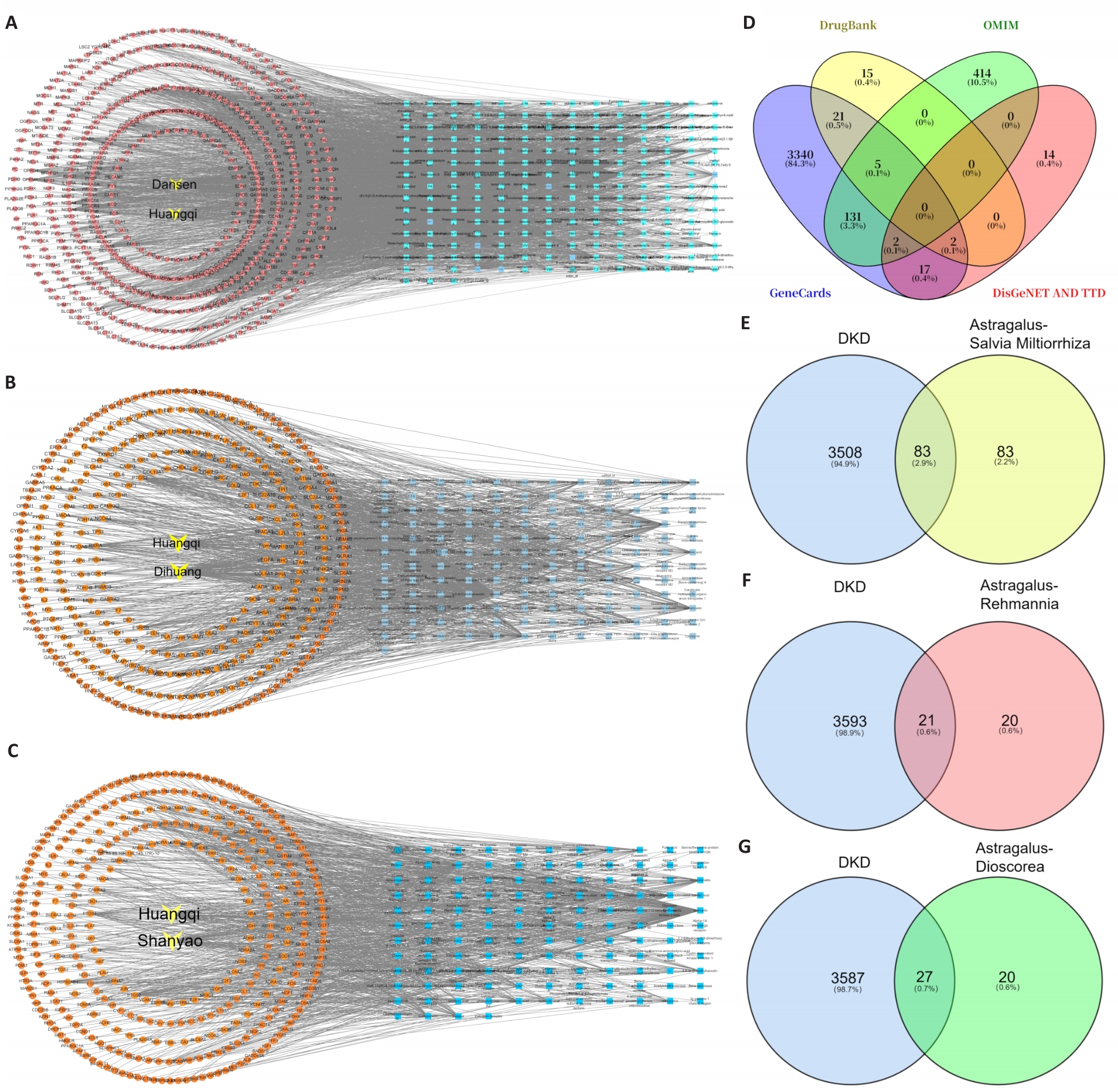
Fig.1 Identification of the effective components and targets of each Astragalus prescription for treatment of diabetic kidney disease (DKD). A-C: Bioactive components of each Astragalus herb pair and their targets. D: Disease-related targets of DKD screened from multiple databases. E-G: Intersection gene targets between each Astragalus herb pair and DKD.
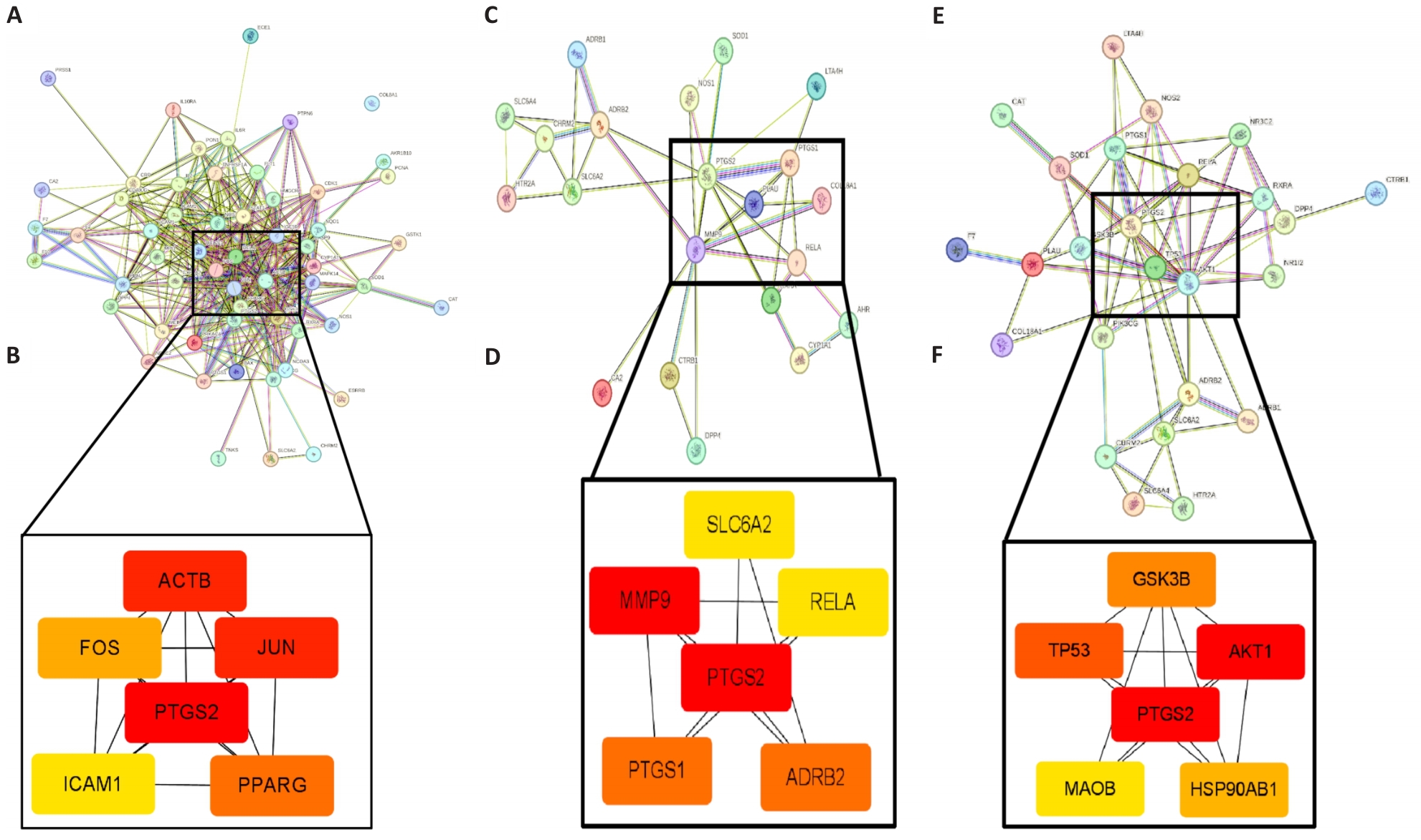
Fig.2 Identification of the core targets of different Astragalus prescriptions for treatment of DKD. A, C, E: Protein-protein interaction (PPI) networks of shared genes between DKD and the herb pairs Astragalus-Salvia miltiorrhiza, Astragalus-Rehmannia, and Astragalus-Dioscorea, respectively. B, D, F: Core therapeutic targets of each herb pair against DKD.
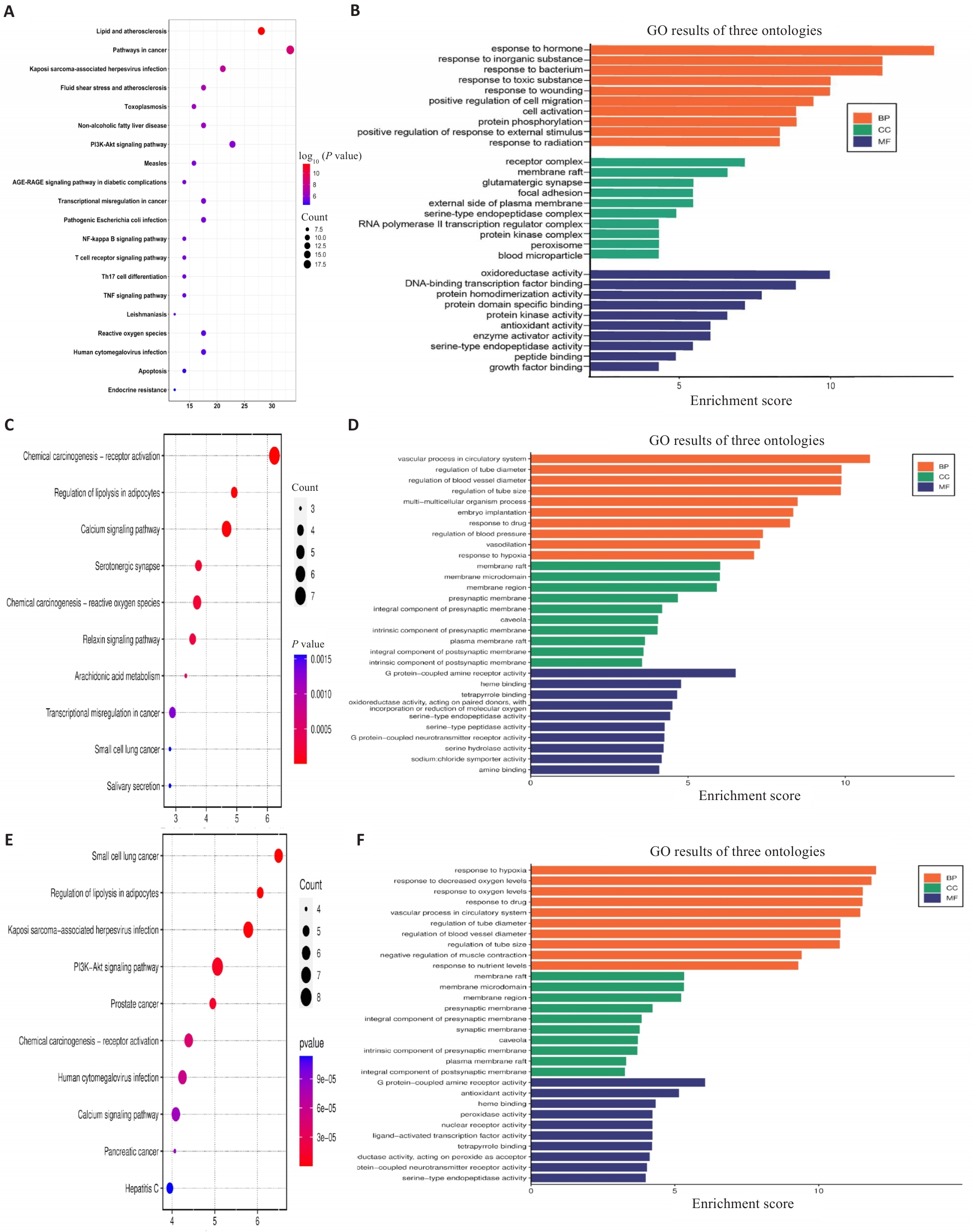
Fig.3 Analysis of potential signaling pathways for treatment of DKD. A, C, E: Bubble plots of KEGG pathway enrichment analysis for shared genes between DKD and the herb pairs Astragalus-Salvia miltiorrhiza, Astragalus-Rehmannia, and Astragalus-Dioscorea, respectively. B, D, F: Gene Ontology (GO) analysis of shared genes between each herb pair and DKD, categorized into biological process (BP), molecular function (MF), and cellular component (CC).
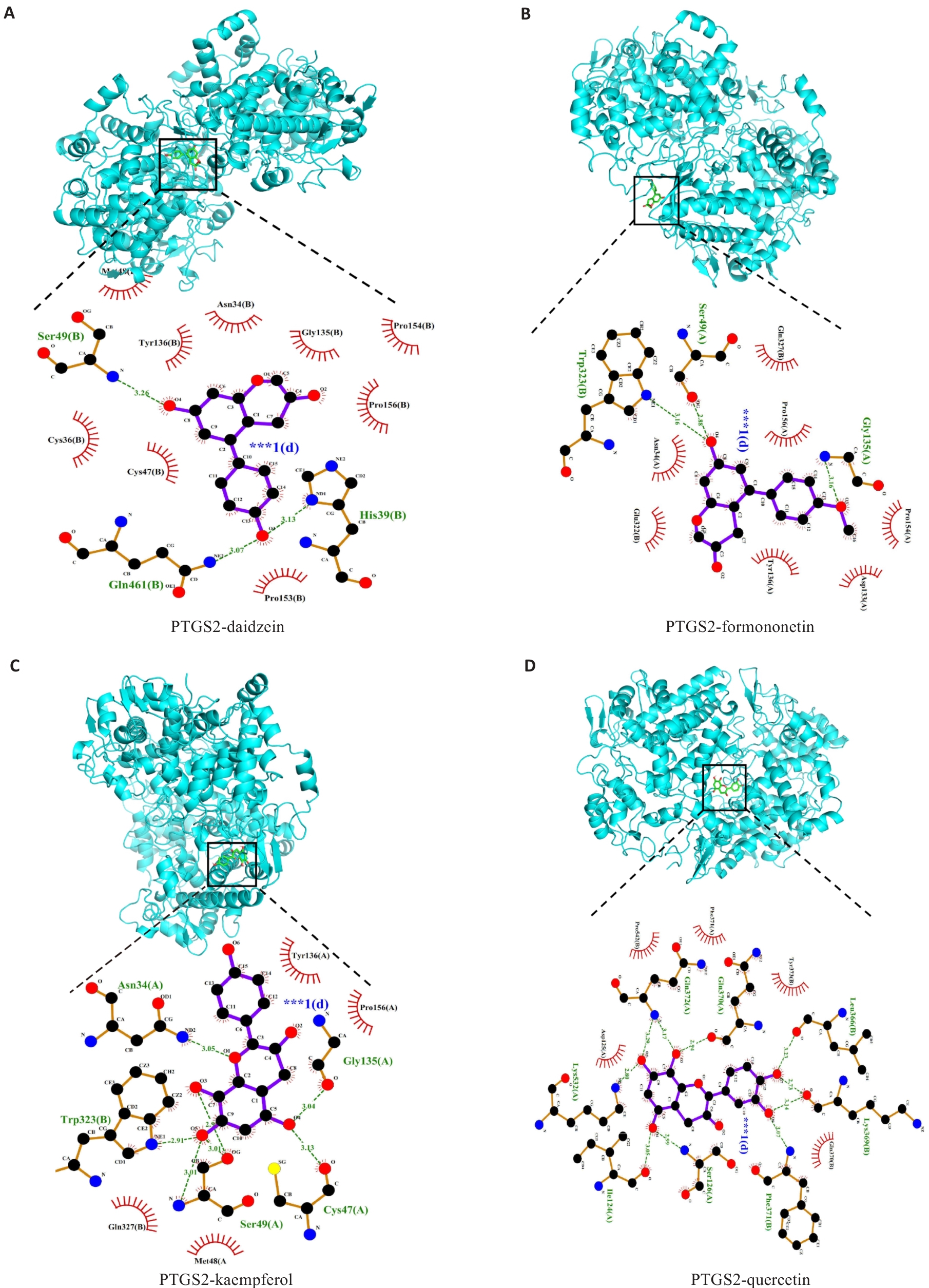
Fig.4 Molecular docking analysis of bioactive compounds with the key core target PTGS2. A: PTGS2 and Daidzein. B: PTGS2 and formononetin. C: PTGS2 and kaempferol. D: PTGS2 and quercetin.
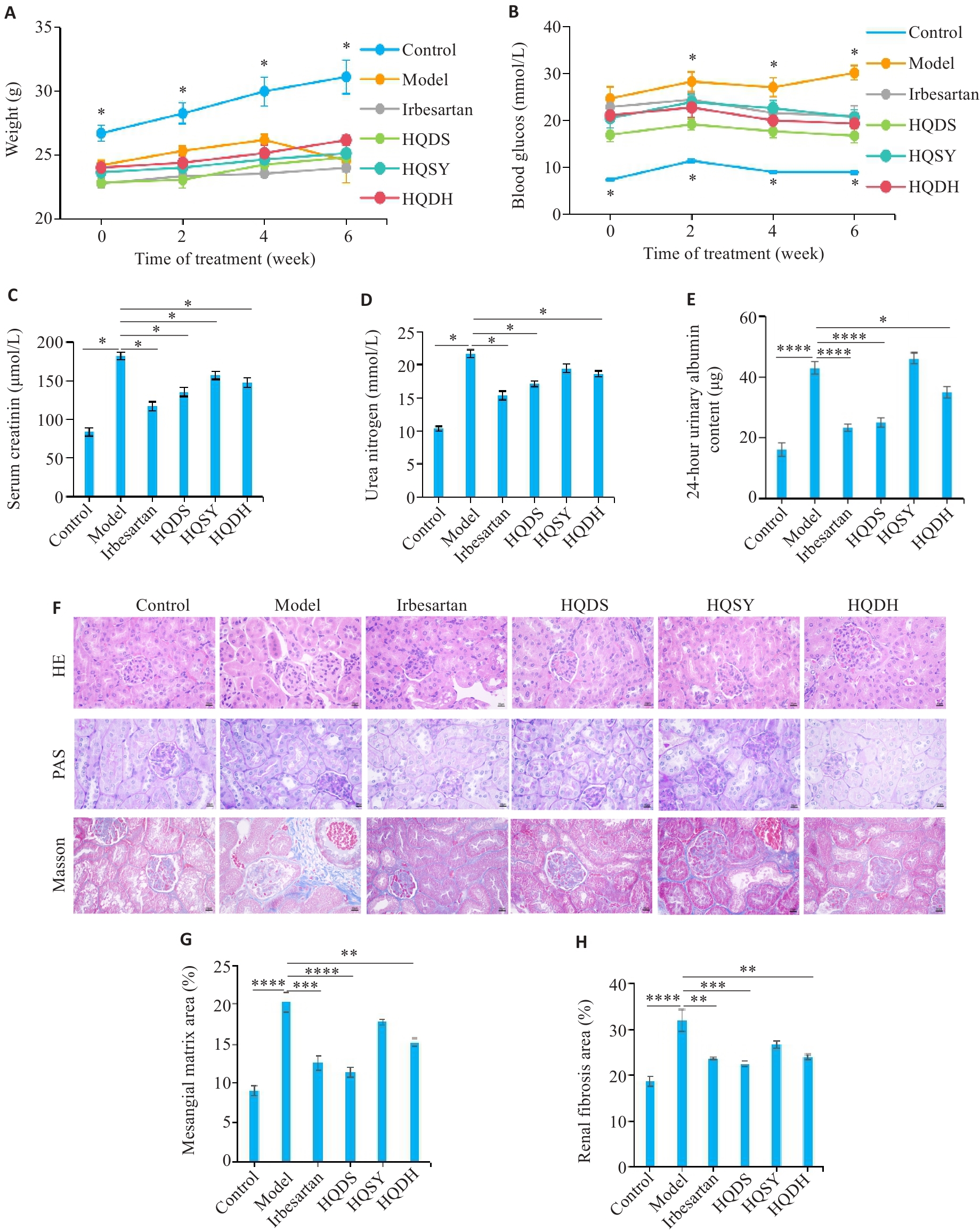
Fig.5 Therapeutic effects of the Astragalus combinations on kidney damage in DKD mice.A: Body weight in Control group, Model group, Irbesartan group, Astragalus and Danshen group (HQDS), Astragalus and Dioscorea opposita group (HQSY), and Astragalus and Rehmannia glutinosa group (HQDH) (n=5). B: Fasting blood glucose levels in each group (n=5). C: Serum creatinine levels in each group (n=5). D: Urea nitrogen levels in each group (n=5). E: 24-hour urinary albumin content in each group (n=5). F: Results of HE, periodic acid-Schiff (PAS), and Masson staining of mouse kidney tissue (Original magnification: ×400). G: Quantifications of PAS trichrome staining (n=3). H: Quantitative analysis of Masson staining results (n=3). Data are presented as Mean±SE. *P<0.05, **P<0.01, ***P<0.001, ****P<0.0001.
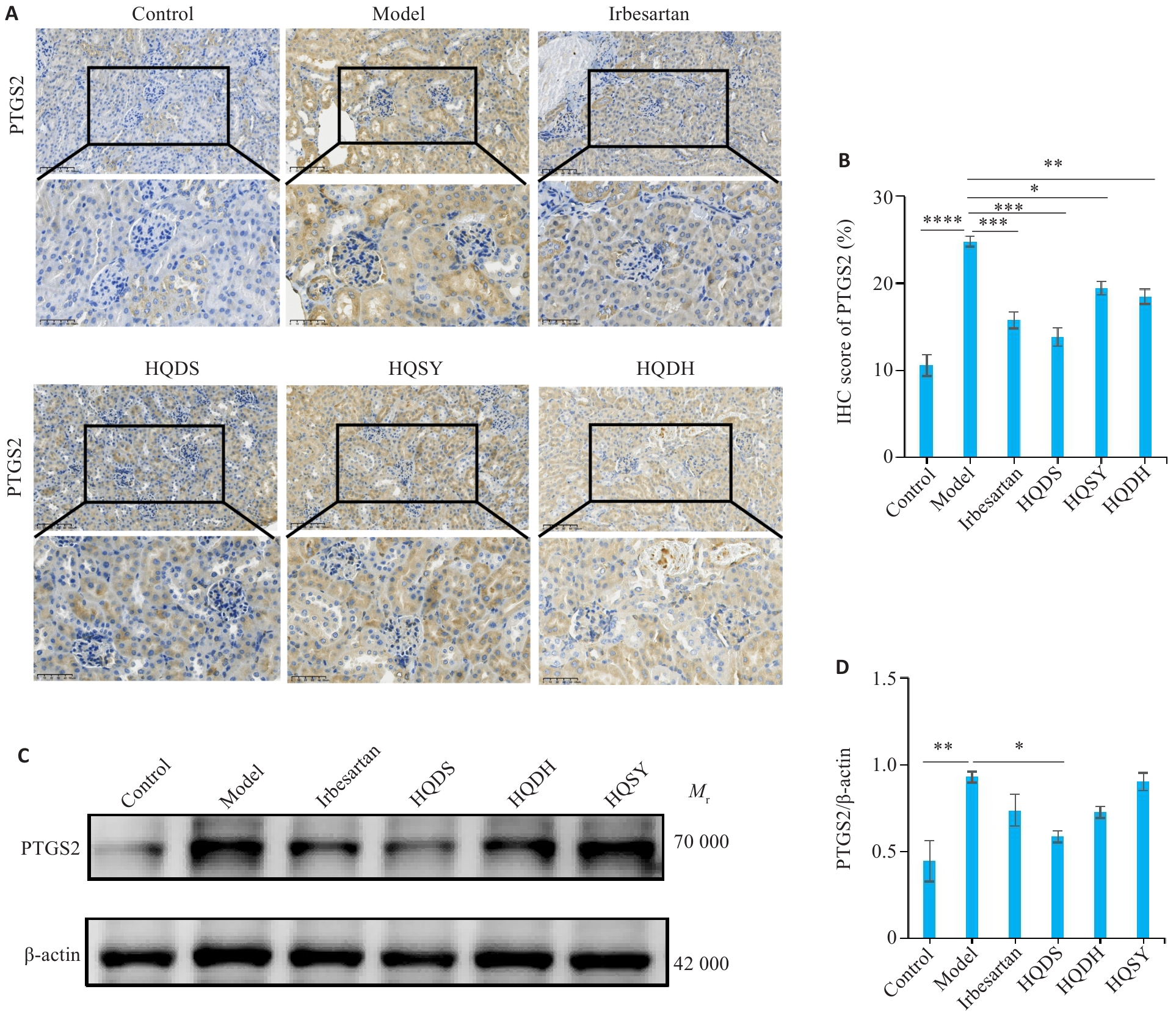
Fig.6 Expression and localization of PTGS2 in renal tissues of DKD mice. A: Immunohistochemical staining showing localization and expression level of PTGS2 protein in the renal tissues of each group (×400). B: Quantitative analysis of PTGS2 immunohistochemical staining intensity. C: Western blotting of PTGS2. D: Quantitative analysis of PTGS2 protein expression levels. Data are presented as Mean±SE. *P<0.05, **P<0.01, ***P<0.001, ****P<0.0001.
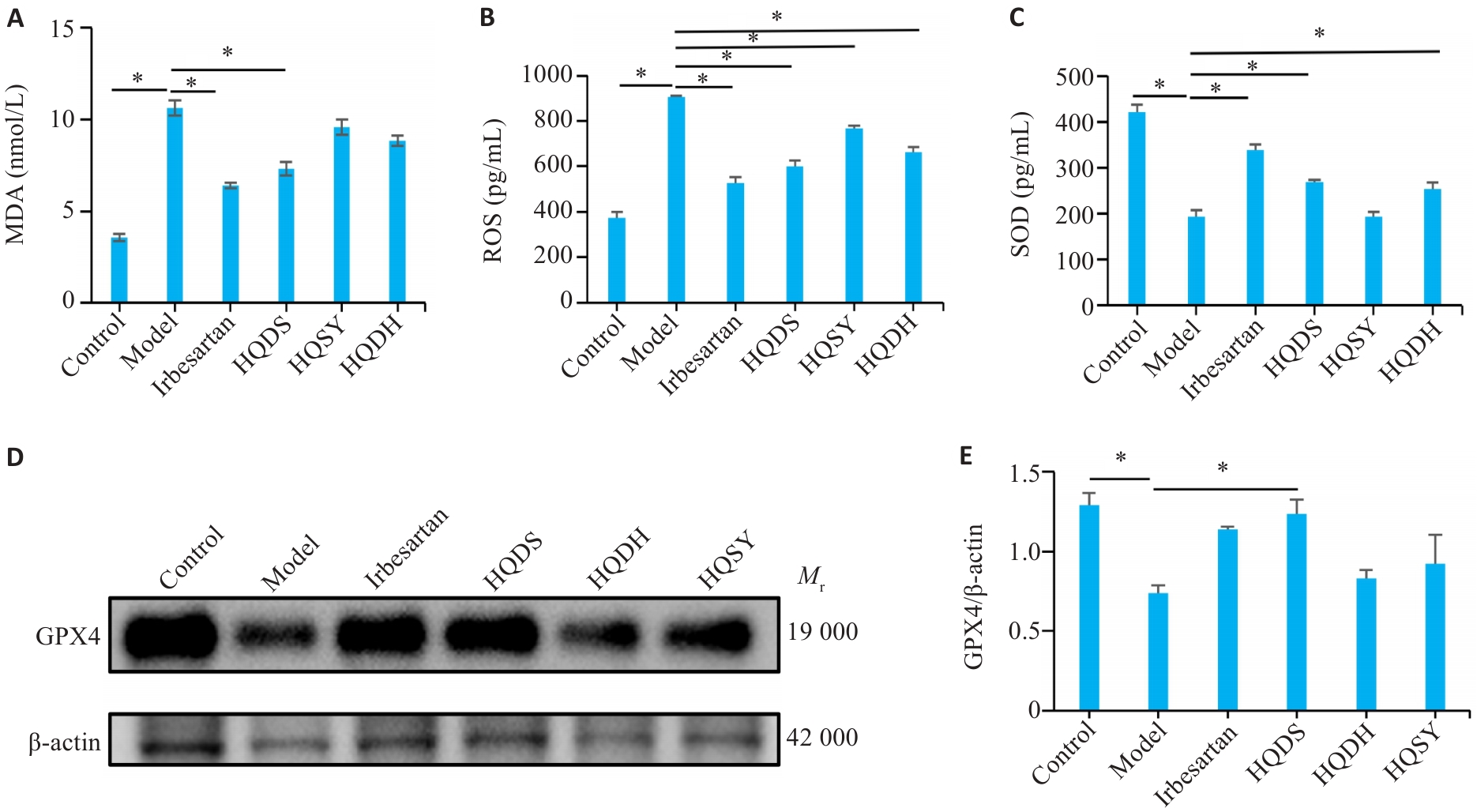
Fig.7 Differential regulatory effects of the 3 Astragali herb pairs on lipid peroxidation in DKD mice. A: Malondialdehyde (MDA) levels in each group. B: Reactive oxygen species (ROS) levels in each group. C: Superoxide dismutase (SOD) levels in each group. D: Western blotting results of GPX4. E: Quantitative analysis of GPX4 protein expression levels. Data are presented as Mean±SE. *P<0.05.
| [1] | Harreiter J, Roden M. Diabetes mellitus: definition, classification, diagnosis, screening and prevention (Update 2023)[J]. Wien Klin Wochenschr, 2023, 135(): 7-17. doi:10.1007/s00508-022-02122-y |
| [2] | 黄为钧, 赵进喜. 基于“新三消论”辨证论治糖尿病及其微血管并发症[J]. 中国中医基础医志, 2025, 31(2): 326-8. |
| [3] | Chaudhuri A, Ghanim H, Arora P. Improving the residual risk of renal and cardiovascular outcomes in diabetic kidney disease: a review of pathophysiology, mechanisms, and evidence from recent trials[J]. Diabetes Obes Metab, 2022, 24(3): 365-76. doi:10.1111/dom.14601 |
| [4] | Shafi T, Sozio SM, Plantinga LC, et al. Serum fructosamine and glycated albumin and risk of mortality and clinical outcomes in hemodialysis patients[J]. Diabetes Care, 2013, 36(6): 1522-33. doi:10.2337/dc12-1896 |
| [5] | Wang Y, He WC. Improving the dysregulation of FoxO1 activity is a potential therapy for alleviating diabetic kidney disease[J]. Front Pharmacol, 2021, 12: 630617. doi:10.3389/fphar.2021.630617 |
| [6] | 中华医学会肾脏病学分会专家组, 陈江华, 孙 林, 等. 糖尿病肾脏疾病临床诊疗中国指南[J]. 中华肾脏病杂志, 2021, 37(3): 255-304. doi:10.3760/cma.j.cn441217-20201125-00041 |
| [7] | Tamborlane WV, Laffel LM, Shehadeh N, et al. Efficacy and safety of dapagliflozin in children and young adults with type 2 diabetes: a prospective, multicentre, randomised, parallel group, phase 3 study[J]. Lancet Diabetes Endocrinol, 2022, 10(5): 341-50. doi:10.1016/s2213-8587(22)00052-3 |
| [8] | Fu ZM, Su XJ, Zhou Q, et al. Protective effects and possible mechanisms of catalpol against diabetic nephropathy in animal models: a systematic review and meta-analysis[J]. Front Pharmacol, 2023, 14: 1192694. doi:10.3389/fphar.2023.1192694 |
| [9] | Gupta S, Dominguez M, Golestaneh L. Diabetic kidney disease: an update[J]. Med Clin North Am, 2023, 107(4): 689-705. doi:10.1016/j.mcna.2023.03.004 |
| [10] | A/L B Vasanth Rao VR, Tan SH, Candasamy M, et al. Diabetic nephropathy: an update on pathogenesis and drug development[J]. Diabetes Metab Syndr, 2019, 13(1): 754-62. doi:10.1016/j.dsx.2018.11.054 |
| [11] | Shi CR, Kwong DL, Li X, et al. MAEL augments cancer stemness properties and resistance to sorafenib in hepatocellular carcinoma through the PTGS2/AKT/STAT3 axis[J]. Cancers (Basel), 2022, 14(12): 2880. doi:10.3390/cancers14122880 |
| [12] | Wang S, Qin S, Cai B, et al. Promising therapeutic mechanism for Chinese herbal medicine in ameliorating renal fibrosis in diabetic nephropathy[J]. Front Endocrinol (Lausanne), 2023, 14:932649. doi:10.3389/fendo.2023.932649 |
| [13] | 李雨婷. 糖尿病肾病的中医治疗[J]. 2025(2): 77-8. |
| [14] | 胡筱娟, 秦 艳, 刘恬园. 基于肾络瘀阻病机与糖尿病肾病相关性临床研究[J]. 陕西中医, 2015, 36(12): 1614-6. doi:10.3969/j.issn.1000-7369.2015.12.022 |
| [15] | 蔡 寸, 马红岩. 杨霓芝教授运用益气活血法治疗糖尿病肾病经验[J]. 河北中医, 2018, 40(6): 805-8. doi:10.3969/j.issn.1002-2619.2018.06.001 |
| [16] | 陈洪宇. 王永钧教授诊治2型糖尿病肾损害的临证经验[J]. 中国中西医结合肾病杂志, 2008, 9(9): 756-9. doi:10.3969/j.issn.1009-587X.2008.09.002 |
| [17] | 魏 敏, 赵晓山, 戴红芳, 等. 罗仁教授治疗糖尿病肾病的经验[C]//中华中医药学会第二十一届全国中医肾病学术会议论文汇编(上). 北京, 2008: 69-71. doi:ConferenceArticle/5aa07878c095d72220743076 |
| [18] | Liang QE, Bai ZY, Xie T, et al. Deciphering the pharmacological mechanisms of qidan Dihuang decoction in ameliorating renal fibrosis in diabetic nephropathy through experimental validation in vitro and in vivo[J]. Evid Based Complement Alternat Med, 2022, 2022: 4137578. doi:10.1155/2022/4137578 |
| [19] | 谢 伟, 沈小勇, 王 硕, 等. 知识史视野下黄芪性-效-用-忌的古今源流考证[J]. 中成药, 2024, 46(7): 2470-4. doi:10.3969/j.issn.1001-1528.2024.07.057 |
| [20] | 王小平, 王振国. 基于本草考证的丹参功效研究[J]. 中医药信息, 2023, 40(7): 58-61. doi:10.19656/j.cnki.1002-2406.20230709 |
| [21] | Xiang L, Jiang PP, Zhou L, et al. Additive effect of qidan Dihuang grain, a traditional Chinese medicine, and angiotensin receptor blockers on albuminuria levels in patients with diabetic nephropathy: a randomized, parallel-controlled trial[J]. Evid Based Complement Alternat Med, 2016, 2016: 1064924. doi:10.1155/2016/1064924 |
| [22] | Xiang L, Cai XS, Zhao XS, et al. Uncovering the mechanism of Qidan Dihuang Granule in the treatment of diabetic kidney disease combined network pharmacology, UHPLC-MS/MS with experimental validation[J]. Heliyon, 2023, 9(11): e21714. doi:10.1016/j.heliyon.2023.e21714 |
| [23] | 韩 明珠, 李晓华. 中医药治疗早期糖尿病肾病的研究进展[J].中国医药导报, 2018, 15(29): 42-5. |
| [24] | 吴 颖, 苗春平, 金海杰, 等. 张银霞运用中药治疗糖尿病经验探讨分析[J]. 中国保健营养, 2019, 29(29): 3-4. |
| [25] | Tian Y, Zhou CX, Yan Q, et al. Dapagliflozin improves diabetic kidney disease by inhibiting ferroptosis through β-hydroxybutyrate production[J]. Ren Fail, 2025, 47(1): 2438857. doi:10.1080/0886022x.2024.2438857 |
| [26] | Lin ZW, Xu YF, Guan LL, et al. Seven ferroptosis-specific expressed genes are considered as potential biomarkers for the diagnosis and treatment of cigarette smoke-induced chronic obstructive pulmonary disease[J]. Ann Transl Med, 2022, 10(6): 331. doi:10.21037/atm-22-1009 |
| [27] | Machado-Junior PAB, Lass A, de Bortolo J, et al. Sodium-glucose cotransporter-2 inhibitor improves renal injury by regulating the redox profile, inflammatory parameters, and pyroptosis in an experimental model of diabetic kidney disease[J]. ACS Pharmacol Transl Sci, 2025, 8(5): 1270-81. doi:10.1021/acsptsci.4c00552 |
| [28] | Kajal A, Singh R. Coriandrum sativum seeds extract mitigate progression of diabetic nephropathy in experimental rats via AGEs inhibition[J]. PLoS One, 2019, 14(3): e0213147. doi:10.1371/journal.pone.0213147 |
| [29] | Zou PJ, He QM, Xia HM, et al. Ferroptosis and its impact on common diseases[J]. PeerJ, 2024, 12: e18708. doi:10.7717/peerj.18708 |
| [30] | Geng JN, Yu XY, Liu CY, et al. Herba artemisiae capillaris extract prevents the development of streptozotocin-induced diabetic nephropathy of rat[J]. Evid Based Complement Alternat Med, 2018: 5180165. doi:10.1155/2018/5180165 |
| [31] | Hartal-Benishay LH, Tal S, Elkader AA, et al. Activity-dependent COX-2 proteolysis modulates aerobic respiration and proliferation in a prostaglandin-independent manner[J]. iScience, 2024, 27(12): 111403. doi:10.1016/j.isci.2024.111403 |
| [32] | Zou C, Xu FF, Shen JC, et al. Identification of a ferroptosis-related prognostic gene PTGS2 based on risk modeling and immune microenvironment of early-stage cervical cancer[J]. J Oncol, 2022: 3997562. doi:10.1155/2022/3997562 |
| [33] | Gao Q, Gao S, Li HY, et al. Multi-omics exploration of the role of PTGS2 as a hub gene in ferroptosis within the artery of takayasu arteritis[J]. J Inflamm Res, 2024, 17: 9135-46. doi:10.2147/jir.s478413 |
| [34] | Yang WS, SriRamaratnam R, Welsch ME, et al. Regulation of ferroptotic cancer cell death by GPX4[J]. Cell, 2014, 156(1/2): 317-31. doi:10.1016/j.cell.2013.12.010 |
| [35] | Xu JL, Weng CY, Zhang YQ, et al. GPX4 knockdown suppresses M2 macrophage polarization in gastric cancer by modulating kynurenine metabolism[J]. Theranostics, 2025, 15(12): 5826-45. doi:10.7150/thno.108817 |
| [36] | Sacco A, Battaglia AM, Botta C, et al. Iron metabolism in the tumor microenvironment-implications for anti-cancer immune response[J]. Cells, 2021, 10(2): 303. doi:10.3390/cells10020303 |
| [37] | Forcina GC, Dixon SJ. GPX4 at the crossroads of lipid homeostasis and ferroptosis[J]. Proteomics, 2019, 19(18): e1800311. doi:10.1002/pmic.201800311 |
| [38] | Xu JY, Pi JK, Zhang YJ, et al. Effects of ferroptosis on cardiovascular diseases[J]. Mediators Inflamm, 2023: 6653202. doi:10.1155/2023/6653202 |
| [1] | Qianqian MA, Yuqi NIU, Mingyu ZUO, Xin LI, Junke FU, Jinjin WANG. Guijianyu alleviates advanced glycation endproducts-induced mouse renal podocyte injury by inhibiting the AGEs-RAGE signaling pathway [J]. Journal of Southern Medical University, 2025, 45(9): 1938-1945. |
| [2] | Jinjin WANG, Wenfei CUI, Xuewei DOU, Binglei YIN, Yuqi NIU, Ling NIU, Guoli YAN. Euonymus alatus delays progression of diabetic kidney disease in mice by regulating EGFR tyrosine kinase inhibitor resistance signaling pathway [J]. Journal of Southern Medical University, 2024, 44(7): 1243-1255. |
| [3] | Benju LIU, Yelei WANG, Haiwen REN, Liwen OU, Xuan DENG, Mengxin HUANG, Xin WU, Quan GONG. 3-Methyladenine alleviates early renal injury in diabetic mice by inhibiting AKT signaling [J]. Journal of Southern Medical University, 2024, 44(7): 1236-1242. |
| [4] | WAN Lu, QIAN Yuchi, NI Wenjing, LU Yuxin, LI Wei, PAN Yan, CHEN Weidong. Linagliptin improves diabetic kidney disease in rats by promoting mitochondrial biogenesis through the AMPK/PGC-1α/TFAM pathway [J]. Journal of Southern Medical University, 2023, 43(12): 2053-2060. |
| [5] | REN Yi, LU Jinying, YU Lu, LI Zongzhe, WANG Gao, YANG Jing. Carnosine protects against diabetic nephropathy in rats by activating the AKT/mTOR pathway and restoring autophagy in the renal tissue [J]. Journal of Southern Medical University, 2023, 43(11): 1965-1970. |
| [6] | XING Lei, XING wenwen, GUO Hongmin. Exploring the therapeutic mechanism of Longqi Fang for diabetic kidney disease based on network pharmacology and verification in rats [J]. Journal of Southern Medical University, 2022, 42(2): 171-180. |
| [7] | LI Zhiyang, LIANG Dan, XIAO Yawen, DAI Yunli, AI Fujun, DING Jing, SHI Mingjun, XIAO Ying, GUO Bing. Oxymatrine improves renal fibrosis and inflammation in diabetic rats by modulating CHK1/2 phosphorylation [J]. Journal of Southern Medical University, 2021, 41(10): 1519-1526. |
| [8] | . Icariin alleviates lipid peroxidation after spinal cord injury in rats [J]. Journal of Southern Medical University, 2018, 38(06): 711-. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||