南方医科大学学报 ›› 2026, Vol. 46 ›› Issue (4): 848-860.doi: 10.12122/j.issn.1673-4254.2026.04.13
• • 上一篇
杨平娟1( ), 姬安琪2, 廖淑馨1, 姚浩楠2, 高震东1, 陈攀1, 程浩艳2(
), 姬安琪2, 廖淑馨1, 姚浩楠2, 高震东1, 陈攀1, 程浩艳2( ), 高社干1,3(
), 高社干1,3( ), 石林林1(
), 石林林1( )
)
收稿日期:2025-11-19
出版日期:2026-04-20
发布日期:2026-04-24
通讯作者:
程浩艳,高社干,石林林
E-mail:pingjuan246@163.com;chenghaoyan@haust.edu.cn;gsg112258@163.com;celine_shih@haust.edu.cn
作者简介:杨平娟,在读硕士研究生,E-mail: pingjuan246@163.com
基金资助:
Pingjuan YANG1( ), Anqi JI2, Shuxin LIAO1, Haonan YAO2, Zhendong GAO1, Pan CHEN1, Haoyan CHENG2(
), Anqi JI2, Shuxin LIAO1, Haonan YAO2, Zhendong GAO1, Pan CHEN1, Haoyan CHENG2( ), Shegan GAO1,3(
), Shegan GAO1,3( ), Linlin SHI1(
), Linlin SHI1( )
)
Received:2025-11-19
Online:2026-04-20
Published:2026-04-24
Contact:
Haoyan CHENG, Shegan GAO, Linlin SHI
E-mail:pingjuan246@163.com;chenghaoyan@haust.edu.cn;gsg112258@163.com;celine_shih@haust.edu.cn
Supported by:摘要:
目的 制备负载光敏剂IR780的中空Cu9S8复合纳米载药系统,探讨其对食管癌光热-光动力(PTT-PDT)的联合治疗效果及潜在作用机制。 方法 采用牺牲模板法制备具有中空结构的Cu9S8纳米颗粒,并利用相变材料月桂酸将光敏剂IR780进行包覆,构建复合纳米颗粒IR780@Cu9S8。通过透射电镜(TEM)、X射线衍射(XRD)、紫外-可见光谱(UV-Vis)等对其形貌与结构进行系统表征。通过CCK-8、细胞活死染色、ROS及线粒体膜电位检测、细胞划痕、Transwell等方法评估其在近红外(808 nm,1.5 W/cm²,5 min)激光照射下对食管癌细胞的增殖、侵袭、迁移等恶性行为的影响。通过构建小鼠食管癌同种移植模型,进一步评估IR780@Cu9S8复合纳米颗粒在体内PTT-PDT联合抗肿瘤疗效及生物安全性。 结果 本研究制备的IR780@Cu9S8复合纳米颗粒呈均一空心类球形结构,光热转换效率约为44.0%。在近红外照射下,IR780@Cu9S8可实现显著的PTT-PDT协同抗肿瘤疗效,KYSE150细胞活力下降(P<0.001),增殖、迁移和侵袭能力也得到抑制(P<0.001)。体内实验同样表明其可在808 nm激光照射后,具有PTT与PDT协同增效,可抑制荷瘤小鼠肿瘤体积的生长(P<0.001),同时具有良好的生物相容性。 结论 IR780@Cu9S8复合纳米颗粒通过整合PTT与PDT的优势,实现光动力与光热效应的协同抗肿瘤作用,为食管癌的联合治疗及靶向药物递送研究提供了新策略。
杨平娟, 姬安琪, 廖淑馨, 姚浩楠, 高震东, 陈攀, 程浩艳, 高社干, 石林林. 多功能中空硫化铜复合纳米颗粒联合光热光动力治疗抑制食管癌的恶性进展[J]. 南方医科大学学报, 2026, 46(4): 848-860.
Pingjuan YANG, Anqi JI, Shuxin LIAO, Haonan YAO, Zhendong GAO, Pan CHEN, Haoyan CHENG, Shegan GAO, Linlin SHI. Hollow copper sulfide nanocomposites combined with photothermal and photodynamic therapy inhibits malignant behaviors of esophageal cancer cells[J]. Journal of Southern Medical University, 2026, 46(4): 848-860.
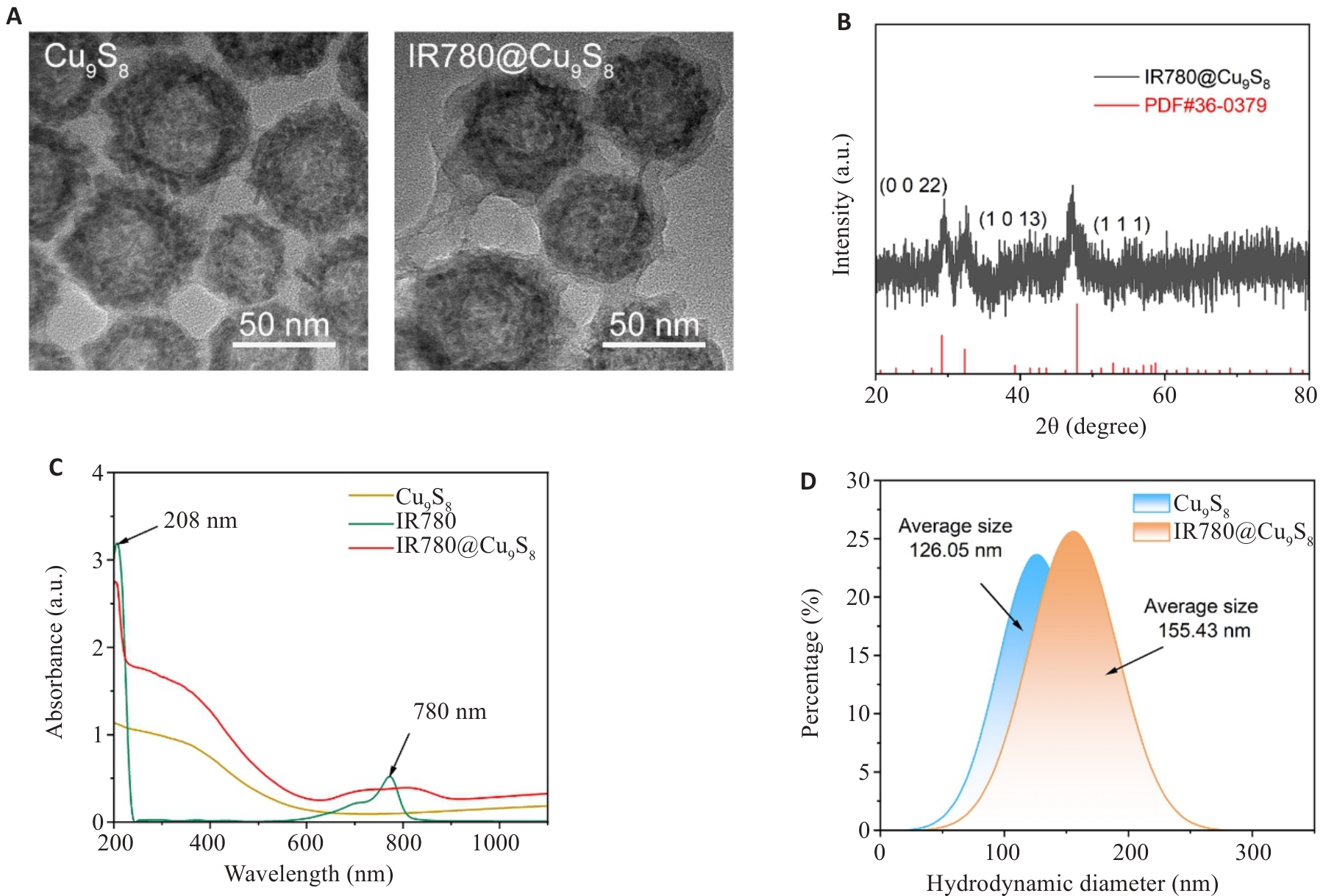
图1 IR780@Cu9S8的合成及表征
Fig.1 Synthesis and characterization of IR780@Cu9S8 nanoparticles. A: TEM images of Cu9S8 and IR780@Cu9S8 nanoparticles. B: XRD spectra of IR780@Cu9S8. C: UV-Vis spectra of Cu9S8, IR780 and IR780@Cu9S8 nanoparticles. D: Hydrodynamic diameter of Cu9S8 and IR780@Cu9S8 nanoparticles.
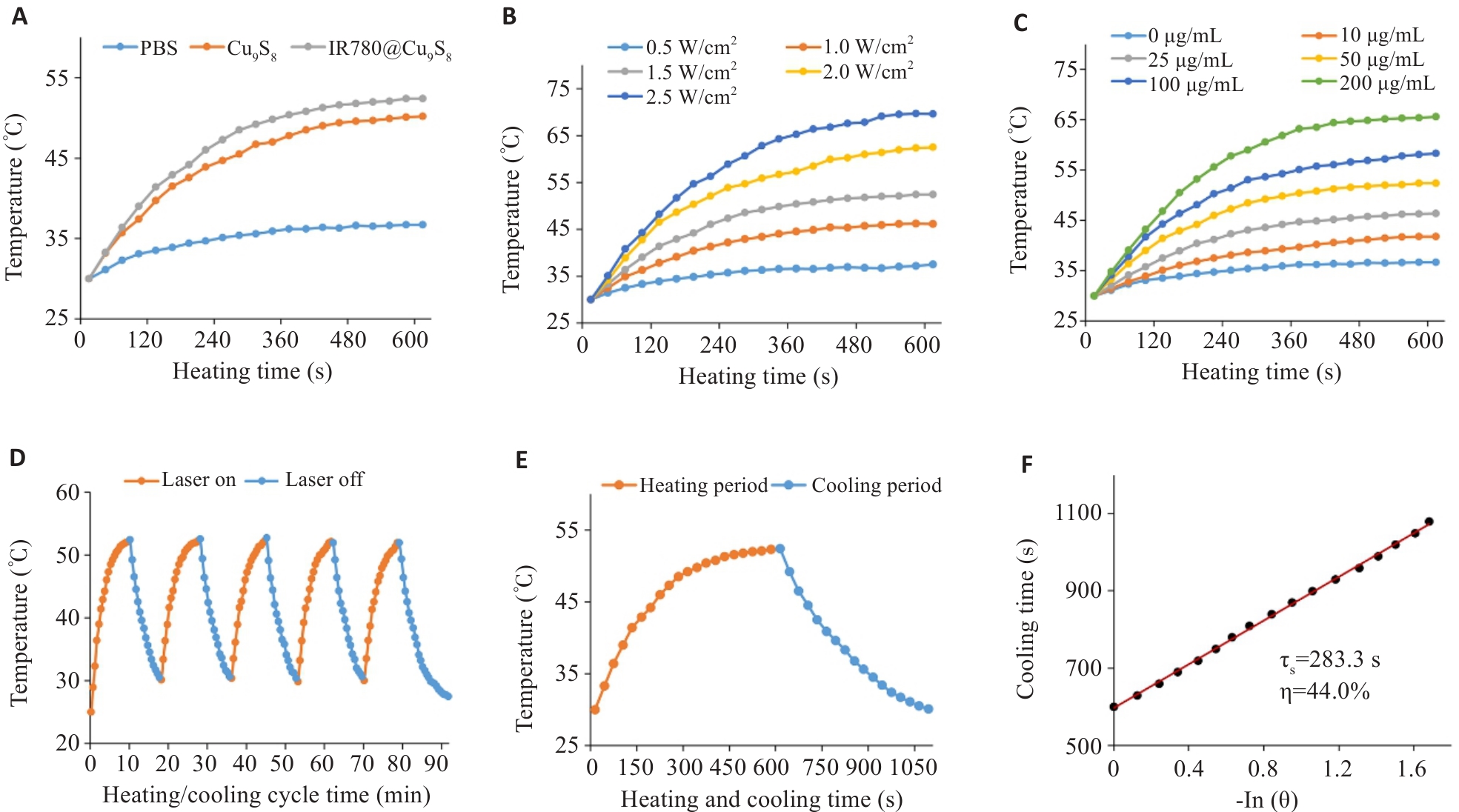
图2 IR780@Cu9S8的光热性能评估
Fig.2 Evaluation of the photothermal performance of IR780@Cu9S8. A: Photothermal curves of PBS, Cu9S8, and IR780@Cu9S8 (50 μg/mL) under 808 nm irradiation. B: Heating curves of IR780@Cu9S8 (50 μg/mL) aqueous solution under various laser powers (0.5, 1.0, 1.5, 2.0, 2.5 W/cm²). C: Photothermal curves of IR780@Cu9S8 aqueous suspensions at different concentrations under 808 nm light irradiation (1.5 W/cm²). D: Photothermal stability curve of IR780@Cu9S8 aqueous suspension (50 µg/mL). E, F: Temperature elevation and photothermal conversion efficiency of IR780@Cu9S8 under 808 nm irradiation.
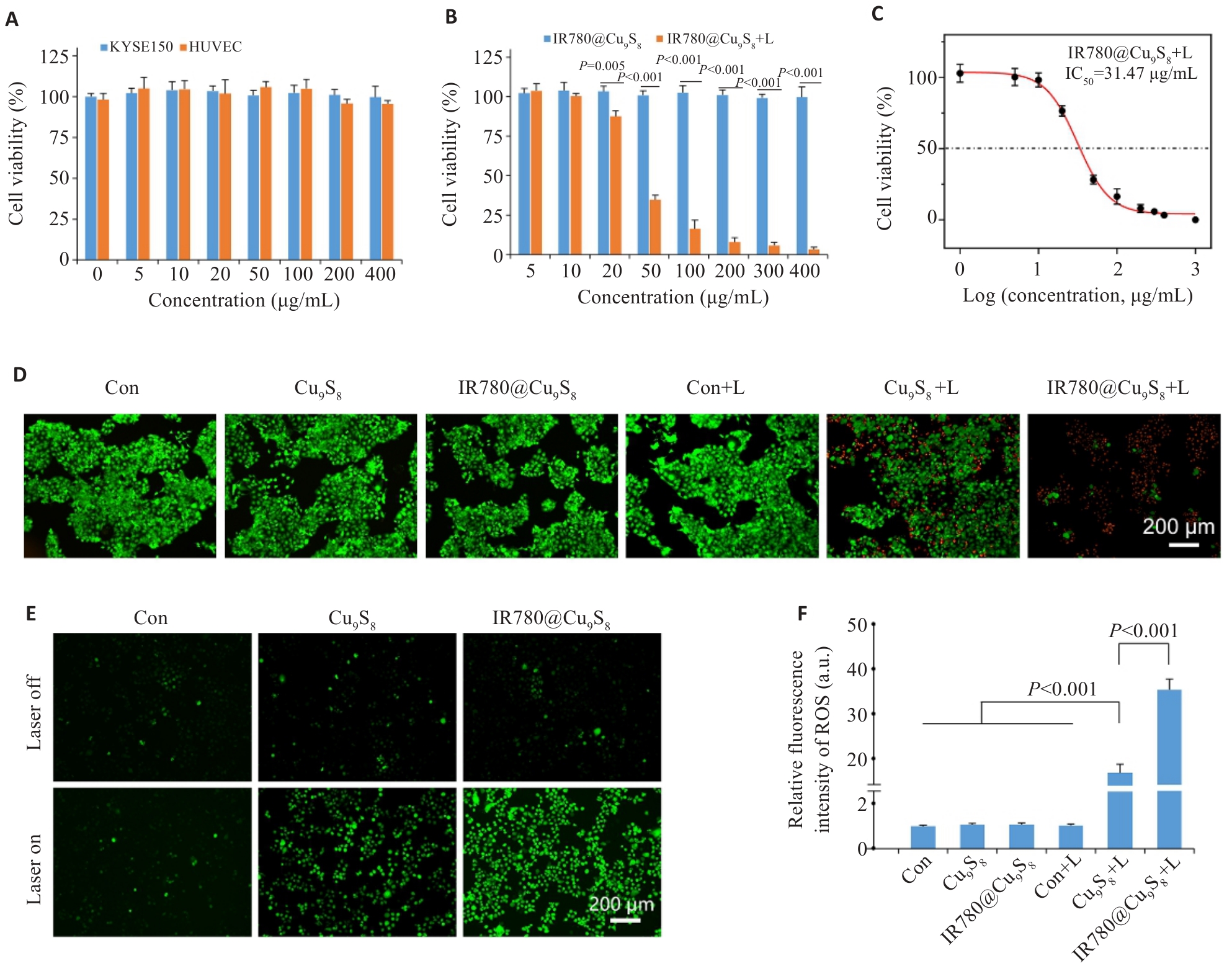
图3 IR780@Cu9S8的体外细胞毒性评估
Fig.3 In vitro cytotoxicity of IR780@Cu9S8 upon 808 nm irradiation. A: Viability of KYSE150 and HUVEC cells after 24 h co-incubation with IR780@Cu9S8. B: Viability of KYSE150 cells with different treatments. C: Viability of KYSE150 cells after 6 h incubation with IR780@Cu9S8 followed by 808 nm irradiation, fitted with a nonlinear dose-response curve (logistic model). D: Fluorescence images of calcein-AM/PI-stained KYSE150 cells after different treatments. E: Representative confocal images of ROS in KYSE150 cells after different treatments. F: Mean fluorescence intensity of ROS in KYSE150 cells. Data are presented as Mean±SD (n=3).
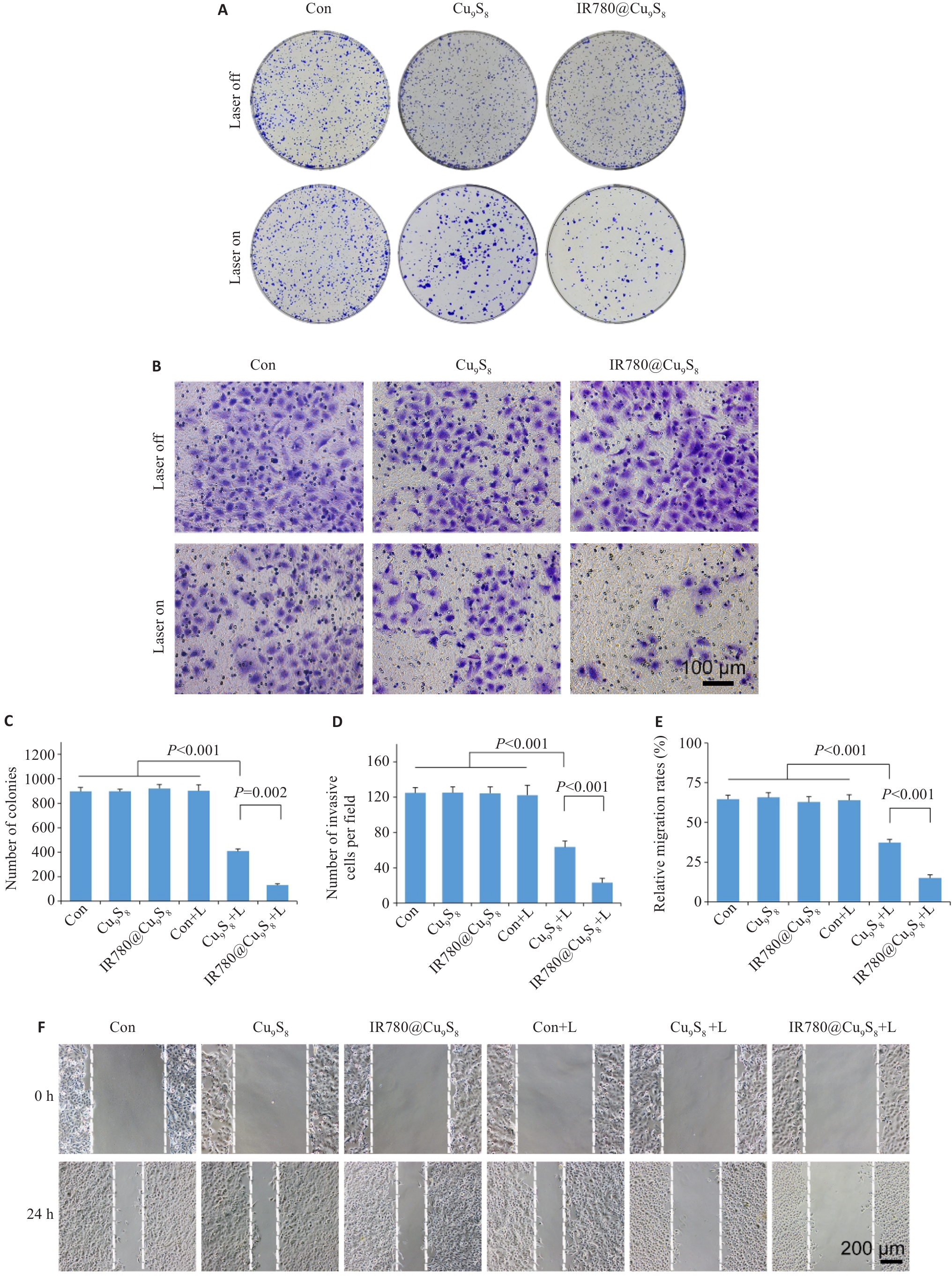
图5 IR780@Cu9S8对体外肿瘤细胞功能的抑制作用评估
Fig.5 Evaluation of the inhibitory effect of IR780@Cu9S8 on malignant behaviors of tumor cells in vitro. A, C: Colony-forming assay of the cells after different treatments. B, D: Changes in cell invasion capacity after the treatments. E, F: Relative migration rate of the cells at 24 h after different treatments in wound-healing assay and representative images of the cells at 0 h and 24 h. Data are presented as Mean±SD (n=3).
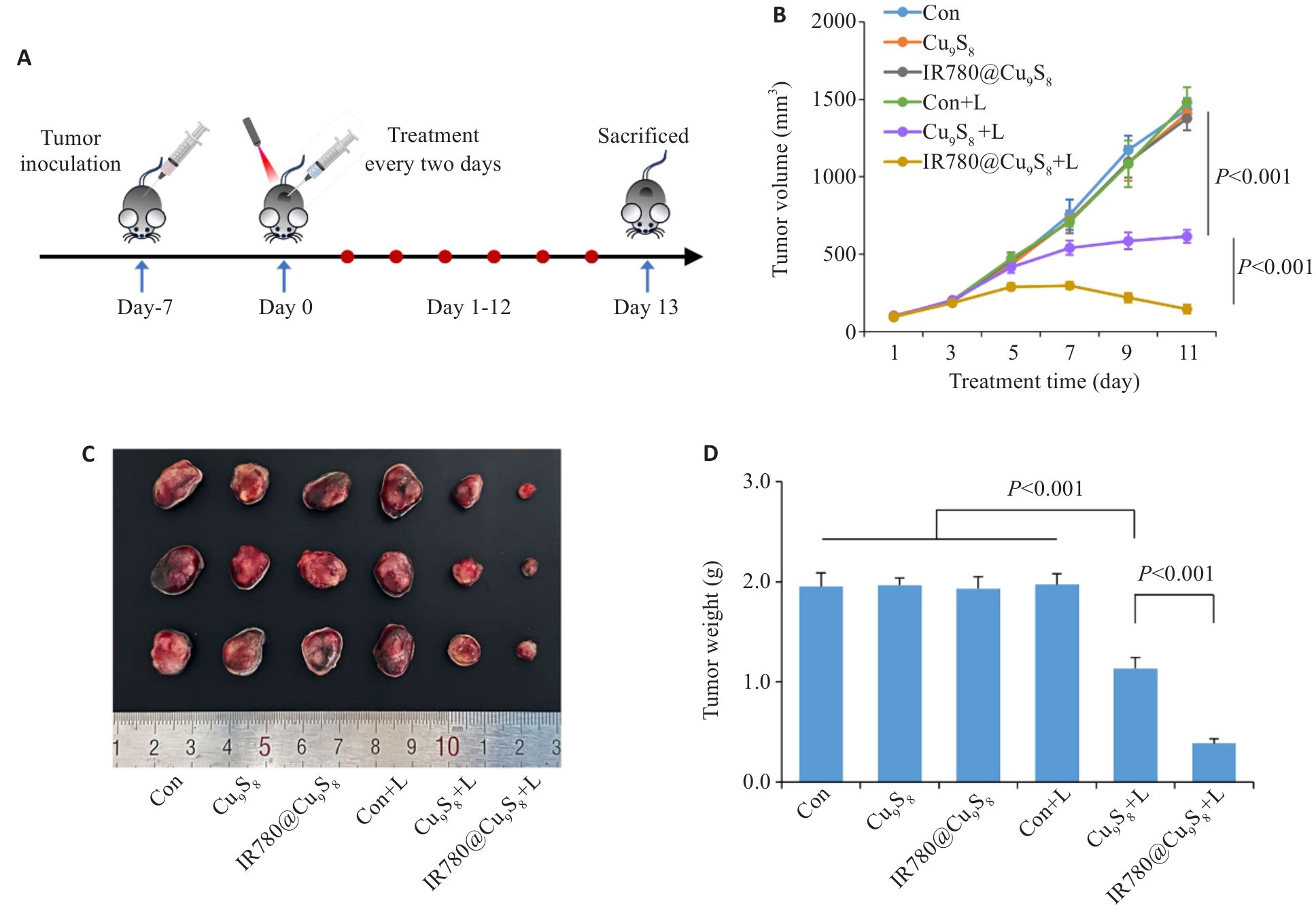
图6 IR780@Cu9S8的体内抗瘤疗效评估
Fig.6 Evaluation of the in vivo antitumor efficacy of IR780@Cu9S8. A:Schematic illustration of the strategy for treatment. B:Changes in tumor volume over time in the tumor-bearing mice. C:Photographs of excised tumors. D:Comparison of tumor weights at the end of the treatment among the groups. Data are presented as Mean±SD (n=3).
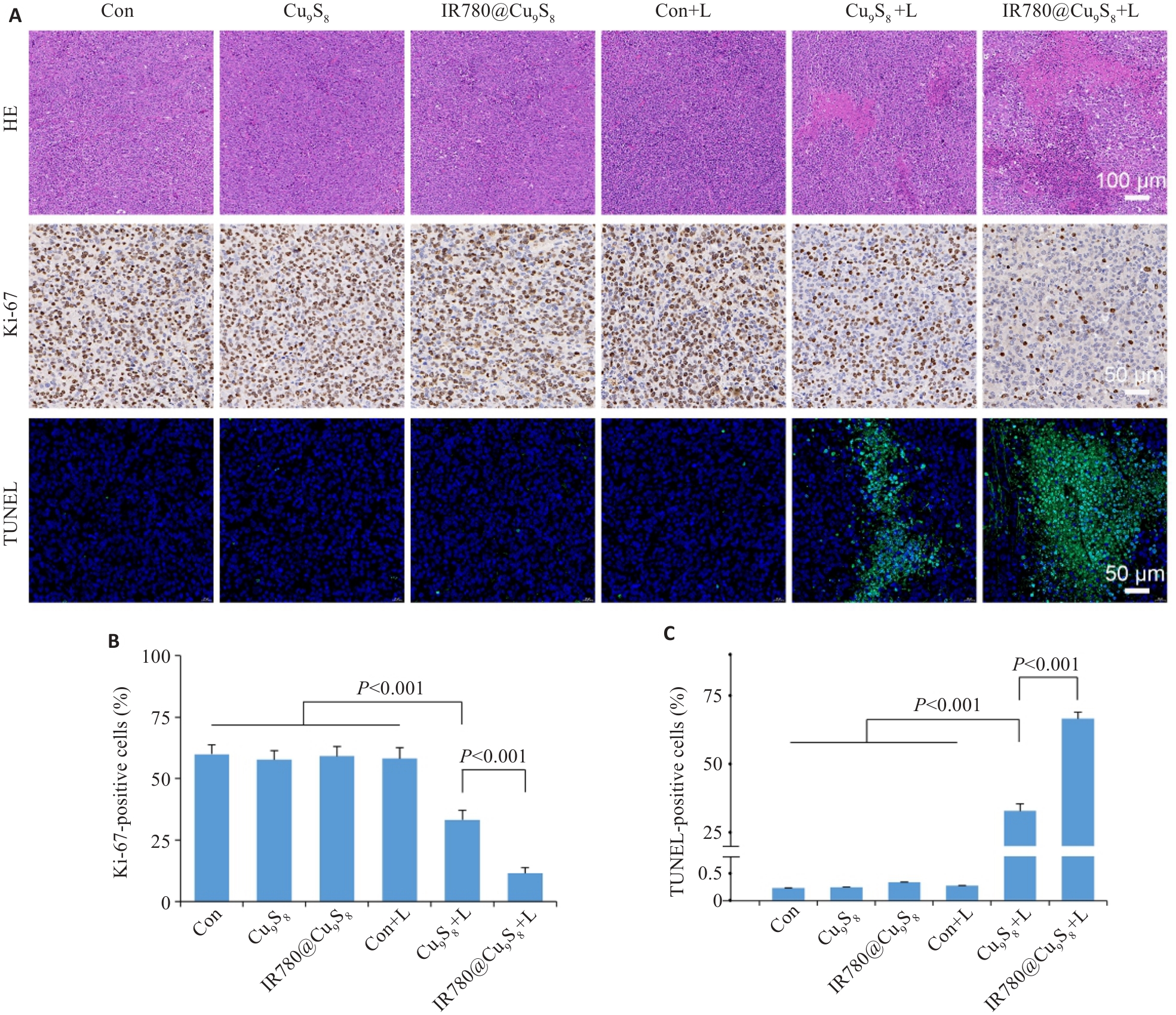
图7 IR780@Cu9S8的体内抗瘤疗效评估(HE染色、免疫荧光染色)
Fig.7 Evaluation of the in vivo antitumor efficacy of IR780@Cu9S8. A: HE staining, Ki-67 immunohistochemistry and TUNEL fluorescence staining of tumor sections. B: Percentage of Ki-67 positive cells among all cells. C: Percentage of TUNEL positive cells among all cells. Data are presented as Mean±SD (n=3).
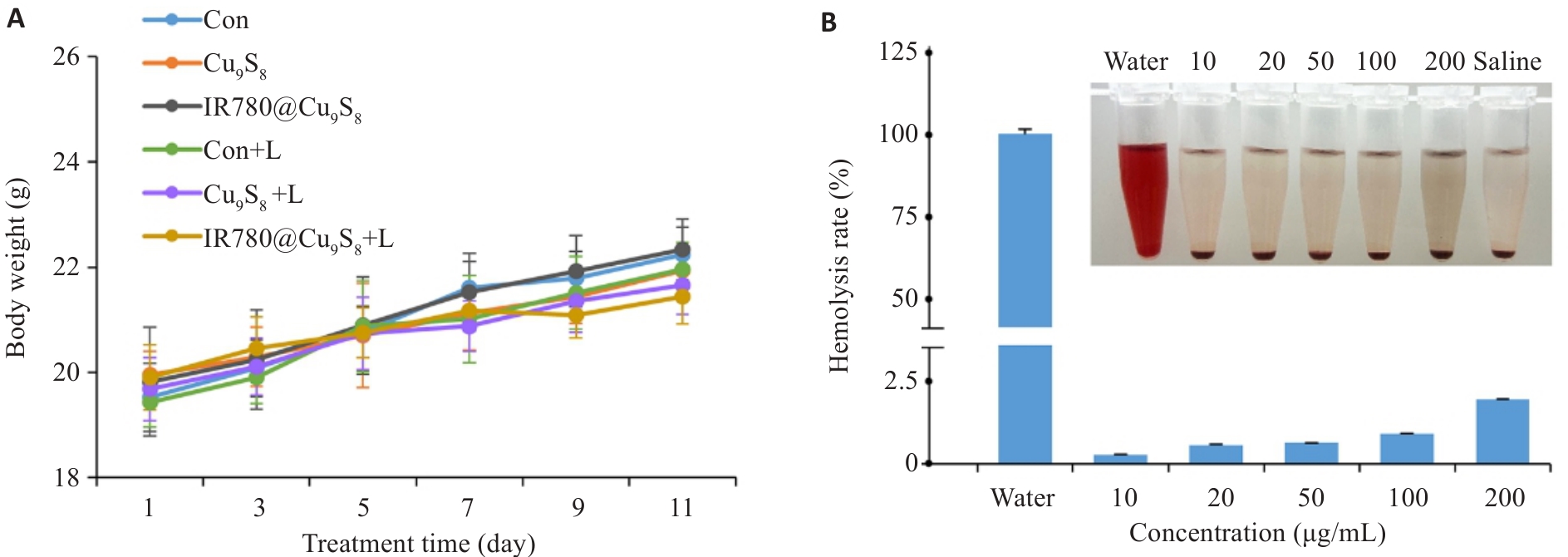
图8 IR780@Cu9S8的体内生物安全性检测
Fig.8 Evaluation of in vivo biocompatibility of IR780@Cu9S8. A: Body weights of male C57BL/6 tumor-bearing mice after different treatments. B: Hemolysis of male C57BL/6 mouse blood after treatment with different concentrations of IR780@Cu9S8. Data are presented as Mean±SD (n=3).
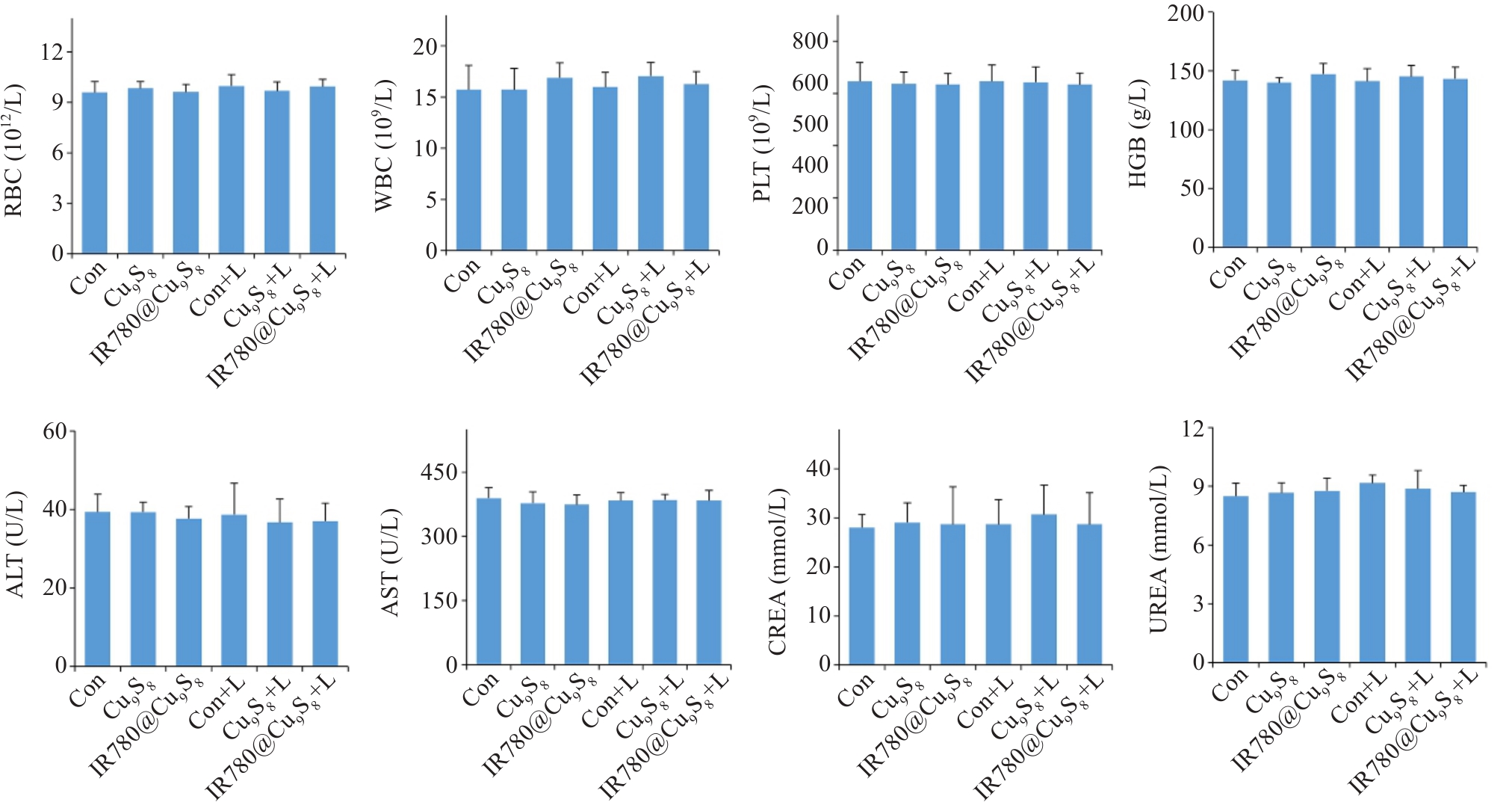
图9 小鼠血常规及血生化主要指标
Fig.9 Hematological and biochemical parameters analysis results of tumor-bearing male C57BL/6 mice after different treatments. Data are presented as Mean±SD (n=3).
| [1] | Bray F, Laversanne M, Sung H, et al. Global cancer statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries[J]. CA Cancer J Clin, 2024, 74(3): 229-63. doi:10.3322/caac.21834 |
| [2] | Inoue T, Ishihara R. Photodynamic therapy for esophageal cancer[J]. Clin Endosc, 2021, 54(4): 494-8. doi:10.5946/ce.2020.073 |
| [3] | Yi XL, Duan QY, Wu FG. Low-temperature photothermal therapy: strategies and applications[J]. Research, 2021, 2021: 2021/9816594. doi:10.34133/2021/9816594 |
| [4] | Cai YY, Chai T, Nguyen W, et al. Phototherapy in cancer treatment: strategies and challenges[J]. Sig Transduct Target Ther, 2025, 10: 115. doi:10.1038/s41392-025-02140-y |
| [5] | Yang YQ, Jiang SH, Stanciu SG, et al. Photodynamic therapy with NIR-II probes: review on state-of-the-art tools and strategies[J]. Mater Horiz, 2024, 11(23): 5815-42. doi:10.1039/d4mh00819g |
| [6] | Cuadrado CF, Lagos KJ, Stringasci MD, et al. Clinical and pre-clinical advances in the PDT/PTT strategy for diagnosis and treatment of cancer[J]. Photodiagn Photodyn Ther, 2024, 50: 104387. doi:10.1016/j.pdpdt.2024.104387 |
| [7] | Chitgupi U, Qin YR, Lovell JF. Targeted nanomaterials for phototherapy[J]. Nanotheranostics, 2017, 1(1): 38-58. doi:10.7150/ntno.17694 |
| [8] | Yano T, Minamide T, Takashima K, et al. Clinical practice of photodynamic therapy using talaporfin sodium for esophageal cancer[J]. J Clin Med, 2021, 10(13): 2785. doi:10.3390/jcm10132785 |
| [9] | Yano T, Kasai H, Horimatsu T, et al. A multicenter phase II study of salvage photodynamic therapy using talaporfin sodium (ME2906) and a diode laser (PNL6405EPG) for local failure after chemoradiotherapy or radiotherapy for esophageal cancer[J]. Oncotarget, 2017, 8(13): 22135-44. doi:10.18632/oncotarget.14029 |
| [10] | Horimatsu T, Yano T, Yamamoto Y, et al. Long-term outcome of PDT for local failure after CRT or RT for oesophageal cancer[J]. J Gastroenterol, 2026, 61(2): 131-8. doi:10.1007/s00535-025-02316-x |
| [11] | Tanaka M, Sasaki M, Nishie H, et al. Efficacy and safety of talaporfin sodium photodynamic therapy as a salvage treatment for locally recurrent esophageal squamous cell carcinoma[J]. Int J Clin Oncol, 2025, 30(11): 2307-15. doi:10.1007/s10147-025-02864-5 |
| [12] | Stapleton S, Dunne M, Milosevic M, et al. Radiation and heat improve the delivery and efficacy of nanotherapeutics by modulating intratumoral fluid dynamics[J]. ACS Nano, 2018, 12(8): 7583-600. doi:10.1021/acsnano.7b06301 |
| [13] | Meng ZQ, Chao Y, Zhou XF, et al. Near-infrared-triggered in situ gelation system for repeatedly enhanced photothermal brachytherapy with a single dose[J]. ACS Nano, 2018, 12(9): 9412-22. doi:10.1021/acsnano.8b04544 |
| [14] | Lei G, Zhuang L, Gan BY. Targeting ferroptosis as a vulnerability in cancer[J]. Nat Rev Cancer, 2022, 22(7): 381-96. doi:10.1038/s41568-022-00459-0 |
| [15] | Ivanchenko M, Evangelista AJ, Jing H. Palladium-rich plasmonic nanorattles with enhanced LSPRs via successive galvanic replacement mediated by co-reduction[J]. RSC Adv, 2021, 11(63): 40112-9. doi:10.1039/d1ra06109g |
| [16] | Yin WD, Li JQ, Ma YC, et al. Precise molecular engineering for the preparation of pyridinium photosensitizers with efficient ROS generation and photothermal conversion[J]. Phys Chem Chem Phys, 2024, 26(13): 10156-67. doi:10.1039/D3CP05718F |
| [17] | Shi Y, van der Meel R, Chen XY, et al. The EPR effect and beyond: Strategies to improve tumor targeting and cancer nanomedicine treatment efficacy[J]. Theranostics, 2020, 10(17): 7921-4. doi:10.7150/thno.49577 |
| [18] | Zhang ZH, Xue H, Xiong Y, et al. Copper incorporated biomaterial-based technologies for multifunctional wound repair[J]. Theranostics, 2024, 14(2): 547-70. doi:10.7150/thno.87193 |
| [19] | Gallo J, Villasante A. Recent advances in biomimetic nanocarrier-based photothermal therapy for cancer treatment[J]. Int J Mol Sci, 2023, 24(20): 15484. doi:10.3390/ijms242015484 |
| [20] | Shoaib A, Javed S, Tabish M, et al. Applications of nanomedicine-integrated phototherapeutic agents in cancer theranostics: a comprehensive review of the current state of research[J]. Nanotechnol Rev, 2024, 13: 20240023. doi:10.1515/ntrev-2024-0023 |
| [21] | Cui X, Lu GH, Fang F, et al. Iron self-boosting polymer nanoenzyme for low-temperature photothermal-enhanced ferrotherapy[J]. ACS Appl Mater Interfaces, 2021, 13(26): 30274-83. doi:10.1021/acsami.1c01658 |
| [22] | Lu DD, Chen MS, Yu LL, et al. Smart-polypeptide-coated mesoporous Fe3O4 nanoparticles: non-interventional target-embolization/thermal ablation and multimodal imaging combination theranostics for solid tumors[J]. Nano Lett, 2021, 21(24): 10267-78. doi:10.1021/acs.nanolett.1c03340 |
| [23] | Nguyen VN, Zhao Z, Tang BZ, et al. Organic photosensitizers for antimicrobial phototherapy[J]. Chem Soc Rev, 2022, 51(9): 3324-40. doi:10.1039/D1CS00647A |
| [24] | Ji AQ, Yang PJ, Ma B, et al. Photothermal-responsive curcumin-loaded copper-based nanocomposites for targeted drug release and combined immunotherapy[J]. J Colloid Interface Sci, 2025, 698: 138042. doi:10.1016/j.jcis.2025.138042 |
| [25] | Li M, Wang Y, Lin HM, et al. Hollow CuS nanocube as nanocarrier for synergetic chemo/photothermal/photodynamic therapy[J]. Mater Sci Eng C, 2019, 96: 591-8. doi:10.1016/j.msec.2018.11.020 |
| [26] | Wang L, Niu CC. IR780-based nanomaterials for cancer imaging and therapy[J]. J Mater Chem B, 2021, 9(20): 4079-97. doi:10.1039/d1tb00407g |
| [27] | Alves CG, Lima-Sousa R, de Melo-Diogo D, et al. IR780 based nanomaterials for cancer imaging and photothermal, photodynamic and combinatorial therapies[J]. Int J Pharm, 2018, 542(1/2): 164-75. doi:10.1016/j.ijpharm.2018.03.020 |
| [28] | Xue YF, Chen KJ, Chen Y, et al. Engineering diselenide-IR780 homodimeric nanoassemblies with enhanced photodynamic and immunotherapeutic effects for triple-negative breast cancer treatment[J]. ACS Nano, 2023, 17(22): 22553-70. doi:10.1021/acsnano.3c06290 |
| [29] | Sun LM, Liu HM, Ye YQ, et al. Smart nanoparticles for cancer therapy[J]. Sig Transduct Target Ther, 2023, 8: 418. doi:10.1038/s41392-023-01642-x |
| [30] | Sultana N, Pathak R, Samanta S, et al. A comprehensive analysis of photothermal therapy (PTT) and photodynamic therapy (PDT) for the treatment of cancer[J]. Process Biochem, 2025, 148: 17-31. doi:10.1016/j.procbio.2024.11.015 |
| [31] | Wang X, Peng JL, Meng C, et al. Recent advances for enhanced photodynamic therapy: from new mechanisms to innovative strategies[J]. Chem Sci, 2024, 15(31): 12234-57. doi:10.1039/d3sc07006a |
| [32] | Yanagita T, Hikichi T, Nakamura J, et al. Novel photodynamic therapy for esophageal squamous cell carcinoma following radiotherapy[J]. Life, 2023, 13(6): 1276. doi:10.3390/life13061276 |
| [33] | Overchuk M, Weersink RA, Wilson BC, et al. Photodynamic and photothermal therapies: synergy opportunities for nanomedicine[J]. ACS Nano, 2023, 17(9): 7979-8003. doi:10.1021/acsnano.3c00891 |
| [34] | Bartusik-Aebisher D, Osuchowski M, Adamczyk M, et al. Advancements in photodynamic therapy of esophageal cancer[J]. Front Oncol, 2022, 12: 1024576. doi:10.3389/fonc.2022.1024576 |
| [35] | Chen YX, Guo F, Rao HH, et al. Photodynamic therapy in esophageal cancer: trends, innovations, and future directions from a global perspective (1985-2024)[J]. Discov Oncol, 2025, 16(1): 765. doi:10.1007/s12672-025-02643-8 |
| [36] | Xu HY, Zhang YR, Guo S, et al. Macrophage reprogramming combined with enhanced photodynamic therapy increases the patency of malignant esophageal obstruction after stenting[J]. Nanoscale, 2024, 16(34): 16035-47. doi:10.1039/D4NR01140F |
| [37] | Jiang N, Jiang M, Chen J, et al. Living hybrid material based on probiotic with photothermal properties inhibits PD-L1 expression after tumouricidal photothermal therapy[J]. Biomater Transl, 2025, 6(1):73-84. doi:10.12336/biomatertransl.2025.01.006 |
| [38] | Fialho MCP, de Oliveira MA, Machado MGC, et al. IR780-based nanotheranostics and in vivo effects: a review[J]. J Nano-theranostics, 2025, 6(1): 8. doi:10.3390/jnt6010008 |
| [39] | Karthikeyan L, Sobhana S, Yasothamani V, et al. Multifunctional theranostic nanomedicines for cancer treatment: Recent progress and challenges[J]. Biomed Eng Adv, 2023, 5: 100082. doi:10.1016/j.bea.2023.100082 |
| [40] | Gawne PJ, Ferreira M, Papaluca M, et al. New opportunities and old challenges in the clinical translation of nanotheranostics[J]. Nat Rev Mater, 2023, 8(12): 783-98. doi:10.1038/s41578-023-00581-x |
| [41] | Liu XH, Geng P, Yu N, et al. Multifunctional Doxorubicin@Hollow-Cu9S8 nanoplatforms for photothermally-augmented chemo-dynamic-chemo therapy[J]. J Colloid Interface Sci, 2022, 615: 38-49. doi:10.1016/j.jcis.2022.01.156 |
| [42] | Yang SB, Diao YZ, Hang LF, et al. BSA@IR780-loaded mesoporous polydopamine nanoparticles with enhanced photostability for multimodal imaging and photothermal therapy of tumors[J]. Nanoscale Adv, 2025, 7(8): 2182-94. doi:10.1039/d5na00008d |
| [43] | Zou Q, Pan HY, Zhang XN, et al. Flower-like Cu9S8 nanocatalysts with highly active sites for synergistic NIR-II photothermal therapy and chemodynamic therapy[J]. J Mater Chem B, 2023, 11(21): 4740-51. doi:10.1039/d3tb00488k |
| [44] | Ren Q, Zhang XJ, Sheng YY, et al. Phytic acid-Cu2+ framework/Cu2- x S nanocomposites with heat-shock protein down-modulation ability for enhanced multimodal combination therapy[J]. J Colloid Interface Sci, 2023, 652: 2116-26. doi:10.1016/j.jcis.2023.09.024 |
| [45] | Song YB, Tan KB, Zhou SF, et al. Biocompatible copper-based nanocomposites for combined cancer therapy[J]. ACS Biomater Sci Eng, 2024, 10(6): 3673-92. doi:10.1021/acsbiomaterials.4c00586 |
| [46] | Wang R, Huang ZW, Xiao YX, et al. Photothermal therapy of copper incorporated nanomaterials for biomedicine[J]. Biomater Res, 2023, 27(1): 121. doi:10.1186/s40824-023-00461-z |
| [1] | 张晨, 许智, 李想, 何彭翼翔, 曲凯林, 宁奇, 金奕玏, 杨宿睿, 吴旭. 具有光热抗菌活性的聚多巴胺修饰藻蓝蛋白纳米颗粒促进小鼠伤口皮肤愈合[J]. 南方医科大学学报, 2025, 45(9): 1959-1966. |
| [2] | 赵亚莉, 李佳怡, 谷变利, 陈攀, 张理, 张小漫, 杨平娟, 石林林, 高社干. Ag₂Se纳米颗粒通过清除牙龈卟啉单胞菌抑制食管癌恶性进展[J]. 南方医科大学学报, 2025, 45(2): 245-253. |
| [3] | 刘 溪, 胡 欢, 房 静, 黄 璐, 程向阳. 红景天注射液降低食管癌根治术患者单肺通气期间肺内分流及血清炎症介质:46例随机对照试验[J]. 南方医科大学学报, 2024, 44(4): 706-711. |
| [4] | 罗 钞, 王高明, 胡力文, 强 勇, 郑 超, 申 翼. 食管癌患者术后预测模型的构建和验证:基于SEER数据库[J]. 南方医科大学学报, 2022, 42(6): 794-804. |
| [5] | 林 萱, 毛 铎, 白瑞霞. 三种商品化光敏剂诱导小鼠免疫原性细胞死亡的效果比较[J]. 南方医科大学学报, 2022, 42(12): 1791-1798. |
| [6] | 孙巧玉, 刘 佳, 樊筱玓, 周咏春, 王效静, 崔 珍. 血浆SEPTIN9甲基化水平检测有助于食管癌诊断和放疗敏感性预测[J]. 南方医科大学学报, 2021, 41(8): 1214-1219. |
| [7] | 何庚翰, 陶 泉, 刘 闯, 张 迪, 周宇平, 刘瑞源. Mn2+掺杂普鲁士蓝纳米颗粒T1-T2双模磁共振成像和光热治疗的体外研究[J]. 南方医科大学学报, 2021, 41(6): 909-915. |
| [8] | 王永霞, 文楚然, 叶建森, 黄河清, 张玉娟, 袁惠玲, 姚广裕, 于 梦. 光动力脂质体凝胶协同曲妥珠单抗体外杀伤耐药性乳腺癌细胞的效果[J]. 南方医科大学学报, 2021, 41(2): 164-172. |
| [9] | 陈 栋, 陈之锋, 王 邹, 杨雅洁, 蒋艳萍, 胡 琛. 纳米硫化铜复合物光热治疗对舌鳞状细胞癌的体内外抑制作用[J]. 南方医科大学学报, 2021, 41(12): 1843-1849. |
| [10] | 黄 强, 卢 笛, 韩继钧, 于洪峰, 董 文, 蔡开灿, 余学飞. 基于开端同轴探头技术的人体正常食管和食管癌介电特性比较[J]. 南方医科大学学报, 2021, 41(11): 1741-1746. |
| [11] | 杏福宝, 张 雷, 唐 震, 李小军, 贡会源, 王 彪, 胡雁南. 胸腹腔镜食管癌根治术对患者术后免疫功能的影响[J]. 南方医科大学学报, 2021, 41(1): 146-150. |
| [12] | 龚 拯, 龙小毛, 韦慧君, 唐 莹, 栗 俊, 马 利, 余 军. 右美托咪定联合肺保护性通气策略可减轻单肺通气食管癌根治术患者的肺损伤[J]. 南方医科大学学报, 2020, 40(07): 1013-1017. |
| [13] | 姚文柱,路 宁,崔曼莉,王 佳,杜召召,张明鑫. 阳性淋巴结比率≥0.16是影响食管癌患者预后的独立危险因素[J]. 南方医科大学学报, 2020, 40(06): 837-842. |
| [14] | 吴宇翔,辛道,刘灿,王峰. SIRT1通过调控Snail表达参与食管癌EC-9706和Eca-109细胞的上皮间质转化[J]. 南方医科大学学报, 2018, 38(11): 1325-. |
| [15] | 曹赛,程梅容,刘素娥,段晓乐,李梅. 食管癌组织中TAK1 和TAB1 的表达及与临床预后的相关性[J]. 南方医科大学学报, 2018, 38(07): 895-. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||