Journal of Southern Medical University ›› 2025, Vol. 45 ›› Issue (7): 1490-1497.doi: 10.12122/j.issn.1673-4254.2025.07.15
Previous Articles Next Articles
Ruimin HAN1( ), Manke ZHAO2, Junfang YUAN3, Zhenhong SHI3, Zhen WANG2(
), Manke ZHAO2, Junfang YUAN3, Zhenhong SHI3, Zhen WANG2( ), Defeng WANG3(
), Defeng WANG3( )
)
Received:2025-03-07
Online:2025-07-20
Published:2025-07-17
Contact:
Zhen WANG, Defeng WANG
E-mail:hrm0201@163.com;wangzhen@hebeu.edu.cn;wdf991217@126.com
Ruimin HAN, Manke ZHAO, Junfang YUAN, Zhenhong SHI, Zhen WANG, Defeng WANG. Live combined Bacillus subtilis and Enterococcus faecium improves glucose and lipid metabolism in type 2 diabetic mice with circadian rhythm disruption via the SCFAs/GPR43/GLP-1 pathway[J]. Journal of Southern Medical University, 2025, 45(7): 1490-1497.
Add to citation manager EndNote|Ris|BibTeX
URL: https://www.j-smu.com/EN/10.12122/j.issn.1673-4254.2025.07.15
| Primer name | Primer sequence (5' to3') | |
|---|---|---|
| Forward primer | Reverse primer | |
| GPR43 | CTTCTTTCTTGGCAATTACTGGC | CCGAAATGGTCAGGTTTAGCAA |
| GCG | AAGAGGAACCGGAACAACATTG | GCCCTCCAAGTAAGAACTCACA |
| GAPDH | AGGTCGGTGTGAACGGATTTG | TGTAGACCATGTAGTTGAGGTCA |
Tab. 1 Primer sequences for genes in the GPR43/GLP-1 pathway
| Primer name | Primer sequence (5' to3') | |
|---|---|---|
| Forward primer | Reverse primer | |
| GPR43 | CTTCTTTCTTGGCAATTACTGGC | CCGAAATGGTCAGGTTTAGCAA |
| GCG | AAGAGGAACCGGAACAACATTG | GCCCTCCAAGTAAGAACTCACA |
| GAPDH | AGGTCGGTGTGAACGGATTTG | TGTAGACCATGTAGTTGAGGTCA |
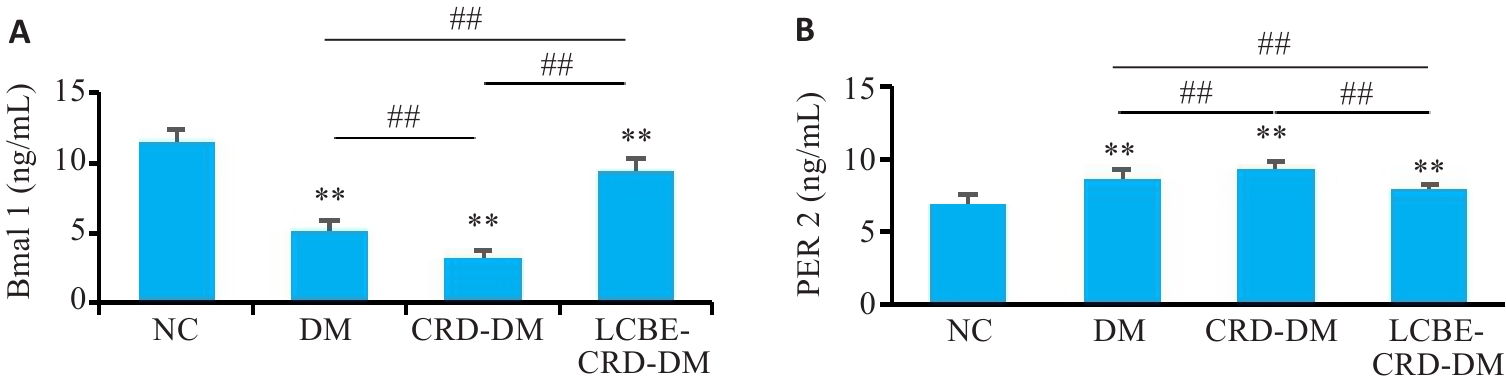
Fig. 4 Levels of rhythmic factors in the mice in each group. A: Level of Bmal 1 in the mice. B: Level of Per 2 in the mice. **P<0.001 vs NC group; ##P<0.001.
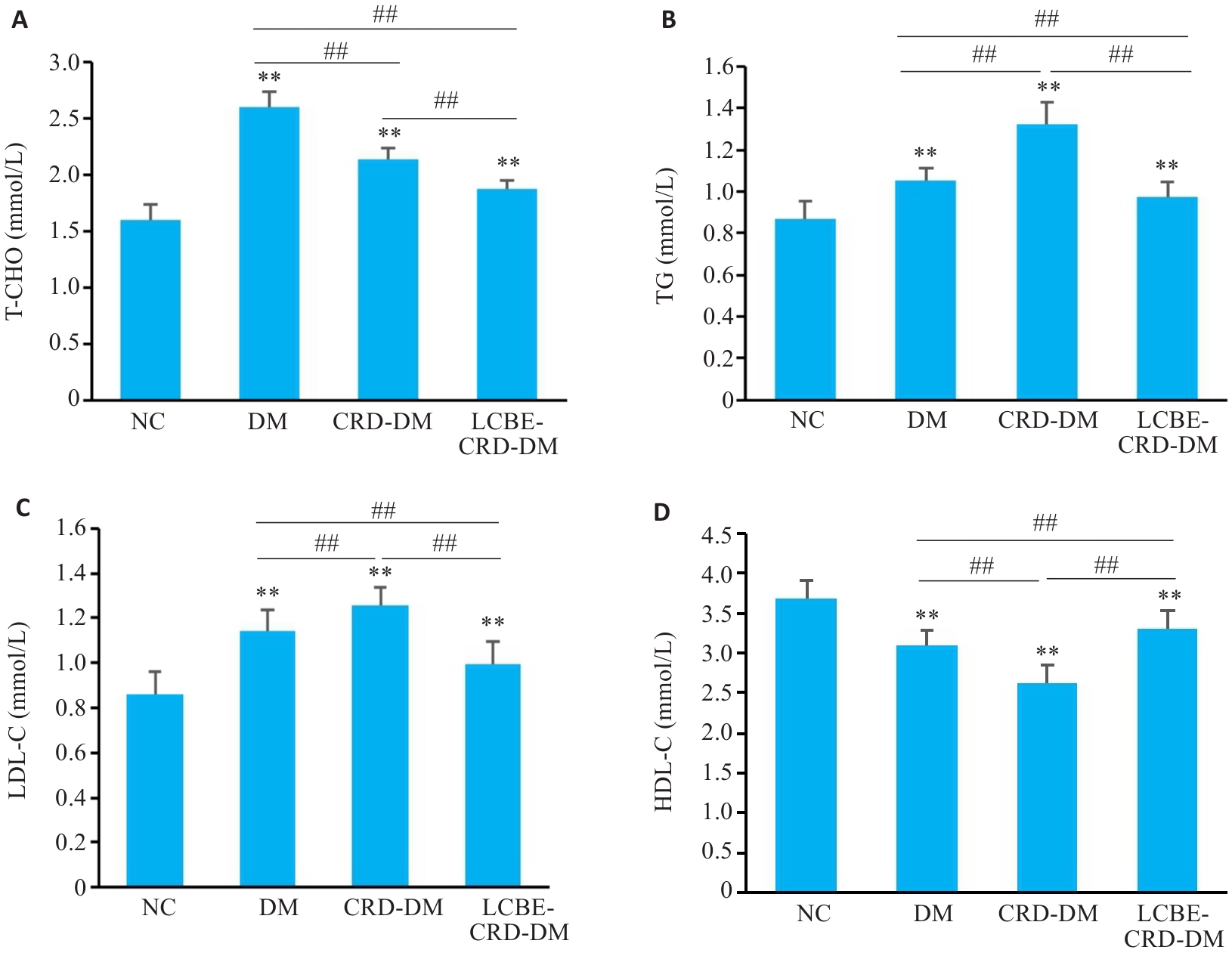
Fig.6 Comparison of lipid levels among the groups. A: Total cholesterol levels of the mice in each group. B: Triglyceride levels of the mice in each group. C: Low-density lipoprotein cholesterol levels of the mice in each group. D: High-density lipoprotein cholesterol levels of the mice in each group. **P<0.001 vs NC group; ##P<0.001.
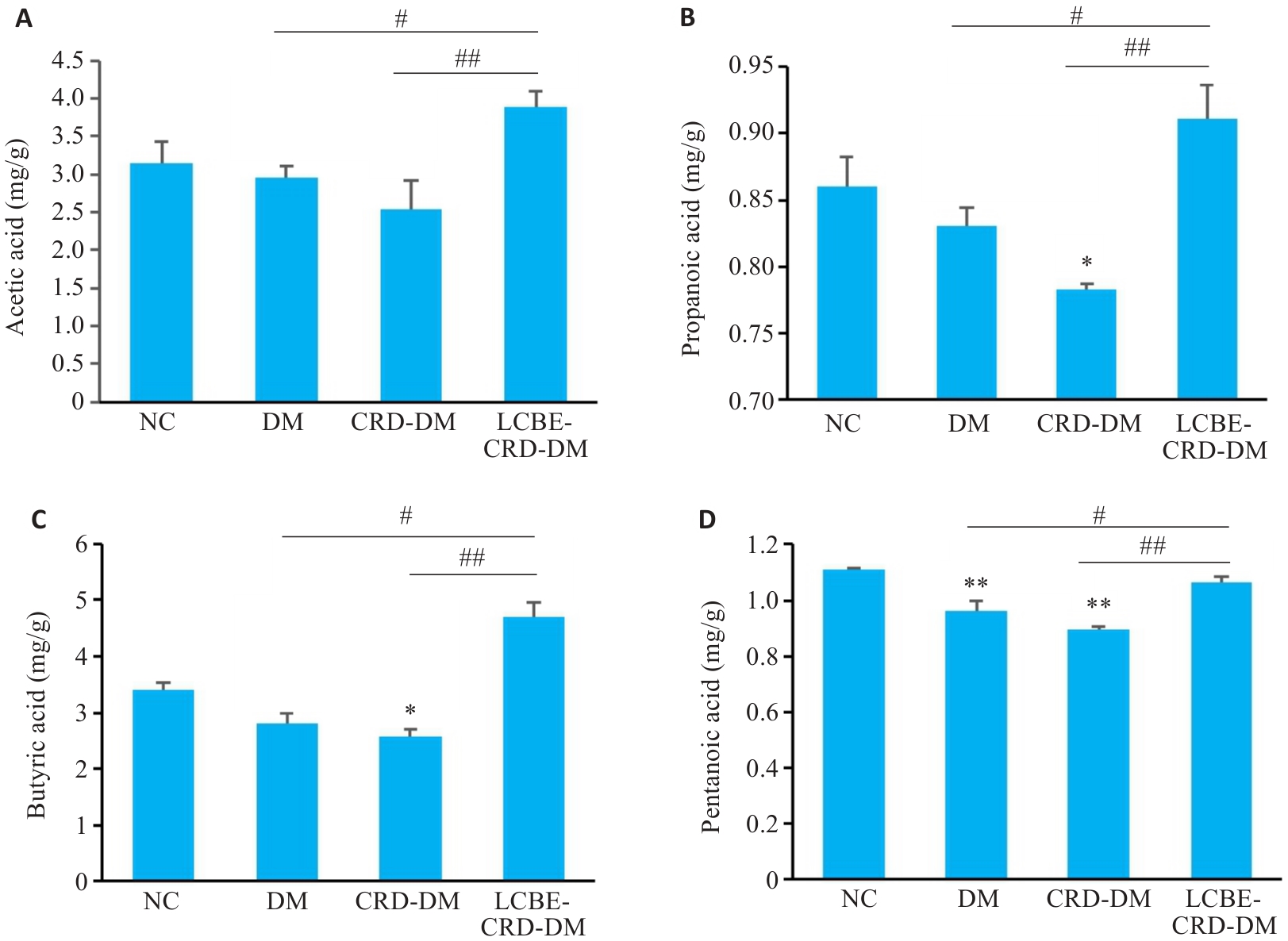
Fig. 9 Fecal levels of short-chain fatty acid in each group. A: Acetic acid level. B: Propanoic acid level. C: Butyric acid level. D: Pentanoic acid level. *P<0.05, **P<0.001 vs NC group; #P<0.05, ##P<0.001.
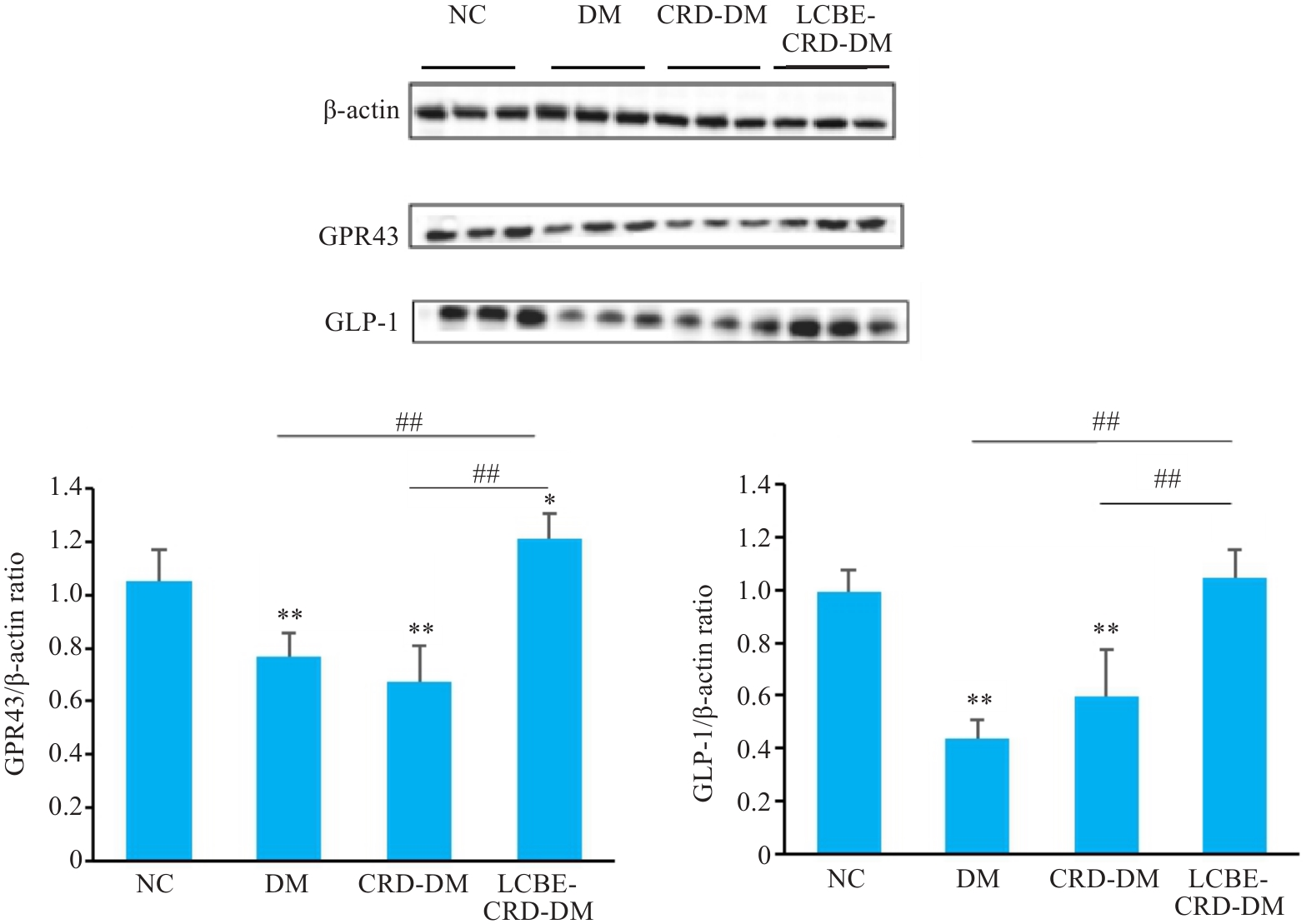
Fig. 11 GPR43 and GLP-1 protein levels in the colon of the mice in each group detected by Western blotting. *P<0.05, **P<0.001 vs NC group; ##P<0.001.
| [1] | Malone JI, Hansen BC. Does obesity cause type 2 diabetes mellitus (T2DM)? Or is it the opposite[J]? Pediatr Diabetes, 2019, 20(1): 5-9. doi:10.1111/pedi.12787 |
| [2] | Sun H, Saeedi P, Karuranga S, et al. IDF Diabetes Atlas: Global, regional and country-level diabetes prevalence estimates for 2021 and projections for 2045[J]. Diabetes Res Clin Pract, 2022, 183: 109119. doi:10.1016/j.diabres.2023.110945 |
| [3] | Snoek FJ, Bremmer MA, Hermanns N. Constructs of depression and distress in diabetes: time for an appraisal[J]. Lancet Diabetes Endocrinol, 2015, 3(6): 450-60. doi:10.1016/s2213-8587(15)00135-7 |
| [4] | Perrin NE, Davies MJ, Robertson N, et al. The prevalence of diabetes-specific emotional distress in people with Type 2 diabetes: a systematic review and meta-analysis[J]. Diabet Med, 2017, 34(11): 1508-20. doi:10.1111/dme.13448 |
| [5] | Cole JB, Florez JC. Genetics of diabetes mellitus and diabetes complications[J]. Nat Rev Nephrol, 2020, 16(7): 377-90. doi:10.1038/s41581-020-0278-5 |
| [6] | Ding L, Xiao XH. Gut microbiota: closely tied to the regulation of circadian clock in the development of type 2 diabetes mellitus[J]. Chin Med J: Engl, 2020, 133(7): 817-25. doi:10.1097/cm9.0000000000000702 |
| [7] | Butler TD, Gibbs JE. Circadian host-microbiome interactions in immunity[J]. Front Immunol, 2020, 11: 1783. doi:10.3389/fimmu.2020.01783 |
| [8] | 赵国杰, 卢 悦, 崔 博, 等. 昼夜节律紊乱对大鼠肠道菌群及肠道屏障的影响[J]. 现代预防医学, 2022, 49(8): 1495-500. |
| [9] | Abildinova GZ, Benberin VV, Vochshenkova TA, et al. Global trends and collaborative networks in gut microbiota-insulin resistance research: a comprehensive bibliometric analysis (2000-2024)[J]. Front Med: Lausanne, 2024, 11: 1452227. doi:10.3389/fmed.2024.1452227 |
| [10] | Qin J, Li Y, Cai Z, et al. A metagenome-wide association study of gut microbiota in type 2 diabetes[J]. Nature, 2012, 490(7418): 55-60. doi:10.1038/nature11450 |
| [11] | Karlsson FH, Tremaroli V, Nookaew I, et al. Gut metagenome in European women with normal, impaired and diabetic glucose control[J]. Nature, 2013, 498(7452): 99-103. doi:10.1038/nature12198 |
| [12] | Sanders ME, Merenstein DJ, Reid G, et al. Author correction: probiotics and prebiotics in intestinal health and disease: from biology to the clinic[J]. Nat Rev Gastroenterol Hepatol, 2019, 16(10): 642. doi:10.1038/s41575-019-0199-6 |
| [13] | Xie K, Tashkin DP, Luo MZ, et al. Pharmacokinetic study of thymol after intravenous injection and high-dose inhalation in mouse model[J]. Pharmacol Res Perspect, 2019, 7(5): e00515. doi:10.1002/prp2.515 |
| [14] | Altaha B, Heddes M, Pilorz V, et al. Genetic and environmental circadian disruption induce weight gain through changes in the gut microbiome[J]. Mol Metab, 2022, 66: 101628. doi:10.1016/j.molmet.2022.101628 |
| [15] | Hutchison AT, Wittert GA, Heilbronn LK. Matching meals to body clocks-impact on weight and glucose metabolism[J]. Nutrients, 2017, 9(3): E222. doi:10.3390/nu9030222 |
| [16] | Bhadra U, Thakkar N, Das P, et al. Evolution of circadian rhythms: from bacteria to human[J]. Sleep Med, 2017, 35: 49-61. doi:10.1016/j.sleep.2017.04.008 |
| [17] | Shi SQ, Ansari TS, McGuinness OP, et al. Circadian disruption leads to insulin resistance and obesity[J]. Curr Biol, 2013, 23(5): 372-81. doi:10.1016/j.cub.2013.01.048 |
| [18] | Reitmeier S, Kiessling S, Clavel T, et al. Arrhythmic gut microbiome signatures predict risk of type 2 diabetes[J]. Cell Host Microbe, 2020, 28(2): 258-72. e6. doi:10.1016/j.chom.2020.06.004 |
| [19] | Bishehsari F, Voigt RM, Keshavarzian A. Circadian rhythms and the gut microbiota: from the metabolic syndrome to cancer[J]. Nat Rev Endocrinol, 2020, 16(12): 731-9. doi:10.1038/s41574-020-00427-4 |
| [20] | Gan Y, Yang C, Tong X, et al. Shift work and diabetes mellitus: a meta-analysis of observational studies[J]. Occup Environ Med, 2015, 72(1): 72-8. doi:10.1136/oemed-2014-102150 |
| [21] | Xie F, Hu K, Fu R, et al. Association between night shift work and the risk of type 2 diabetes mellitus: a cohort-based meta-analysis[J]. BMC Endocr Disord, 2024, 24(1): 268. doi:10.1186/s12902-024-01808-w |
| [22] | Leung GKW, Huggins CE, Ware RS, et al. Time of day difference in postprandial glucose and insulin responses: Systematic review and meta-analysis of acute postprandial studies[J]. Chronobiol Int, 2020, 37(3): 311-26. doi:10.1080/07420528.2019.1683856 |
| [23] | Viklund A, Andersson T, Selander J, et al. Night and shift work patterns and incidence of type 2 diabetes and hypertension in a prospective cohort study of healthcare employees[J]. Scand J Work Environ Health, 2023, 49(6): 439-48. doi:10.5271/sjweh.4104 |
| [24] | Mokhlesi B, Temple KA, Tjaden AH, et al. Association of self-reported sleep and circadian measures with glycemia in adults with prediabetes or recently diagnosed untreated type 2 diabetes[J]. Diabetes Care, 2019, 42(7): 1326-32. doi:10.2337/dc19-0298 |
| [25] | Gao Y, Gan T, Jiang L, et al. Association between shift work and risk of type 2 diabetes mellitus: a systematic review and dose-response meta-analysis of observational studies[J]. Chronobiol Int, 2020, 37(1): 29-46. doi:10.1080/07420528.2019.1683570 |
| [26] | Voigt RM, Forsyth CB, Green SJ, et al. Circadian disorganization alters intestinal microbiota[J]. PLoS One, 2014, 9(5): e97500. doi:10.1371/journal.pone.0097500 |
| [27] | Thaiss CA, Levy M, Elinav E. Chronobiomics: the biological clock as a new principle in host-microbial interactions[J]. PLoS Pathog, 2015, 11(10): e1005113. doi:10.1371/journal.ppat.1005113 |
| [28] | Fatima N, Rana S. Metabolic implications of circadian disruption[J]. Pflügers Arch Eur J Physiol, 2020, 472(5): 513-26. doi:10.1007/s00424-020-02381-6 |
| [29] | Fan Y, Pedersen O. Gut microbiota in human metabolic health and disease[J]. Nat Rev Microbiol, 2021, 19(1): 55-71. doi:10.1038/s41579-020-0433-9 |
| [30] | Jayedi A, Aletaha A, Zeraattalab-Motlagh S, et al. Comparative efficacy and safety of probiotics, prebiotics, and synbiotics for type 2 diabetes management: a systematic review and network meta-analysis[J]. Diabetes Metab Syndr Clin Res Rev, 2024, 18(1): 102923. doi:10.1016/j.dsx.2023.102923 |
| [31] | 李宜航. 四君子汤改善CKD小鼠肠道微生态的作用机制研究[D]. 沈阳: 辽宁中医药大学, 2023. |
| [32] | Everard A, Belzer C, Geurts L, et al. Cross-talk between Akkermansia muciniphila and intestinal epithelium controls diet-induced obesity[J]. Proc Natl Acad Sci USA, 2013, 110(22): 9066-71. doi:10.1073/pnas.1219451110 |
| [33] | Reutrakul S, Van Cauter E. Sleep influences on obesity, insulin resistance, and risk of type 2 diabetes[J]. Metabolism, 2018, 84: 56-66. doi:10.1016/j.metabol.2018.02.010 |
| [34] | Zarrinpar A, Chaix A, Yooseph S, et al. Diet and feeding pattern affect the diurnal dynamics of the gut microbiome[J]. Cell Metab, 2014, 20(6): 1006-17. doi:10.1016/j.cmet.2014.11.008 |
| [35] | Jiang J, Xiong J, Ni JB, et al. Live combined B. subtilis and E. faecium alleviate liver inflammation, improve intestinal barrier function, and modulate gut microbiota in mice with non-alcoholic fatty liver disease[J]. Med Sci Monit, 2021, 27: 931143-1 -931143-12. doi:10.12659/msm.931143 |
| [36] | Pi X, Teng W, Fei D, et al. Effects of live combined Bacillus subtilis and Enterococcus faecium on gut microbiota composition in C57BL/6 mice and in humans[J]. Front Cell Infect Microbiol, 2022, 12: 821662. doi:10.3389/fcimb.2022.821662 |
| [37] | Huang JL, Xu YF, Wang MH, et al. Enterococcus faecium R-026 combined with Bacillus subtilis R-179 alleviate hypercho-lesterolemia and modulate the gut microbiota in C57BL/6 mice[J]. FEMS Microbiol Lett, 2023, 37010.1093: femsle. doi:10.1093/femsle/fnad118 |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||