Journal of Southern Medical University ›› 2024, Vol. 44 ›› Issue (7): 1236-1242.doi: 10.12122/j.issn.1673-4254.2024.07.03
Previous Articles Next Articles
Benju LIU1( ), Yelei WANG1,3(
), Yelei WANG1,3( ), Haiwen REN2,4, Liwen OU1, Xuan DENG1, Mengxin HUANG1, Xin WU1, Quan GONG2(
), Haiwen REN2,4, Liwen OU1, Xuan DENG1, Mengxin HUANG1, Xin WU1, Quan GONG2( )
)
Received:2024-01-07
Online:2024-07-20
Published:2024-07-25
Contact:
Quan GONG
E-mail:liubenju1981@aliyun.com;568862187@qq.com;gongquan1998@163.com
Supported by:Benju LIU, Yelei WANG, Haiwen REN, Liwen OU, Xuan DENG, Mengxin HUANG, Xin WU, Quan GONG. 3-Methyladenine alleviates early renal injury in diabetic mice by inhibiting AKT signaling[J]. Journal of Southern Medical University, 2024, 44(7): 1236-1242.
Add to citation manager EndNote|Ris|BibTeX
URL: https://www.j-smu.com/EN/10.12122/j.issn.1673-4254.2024.07.03
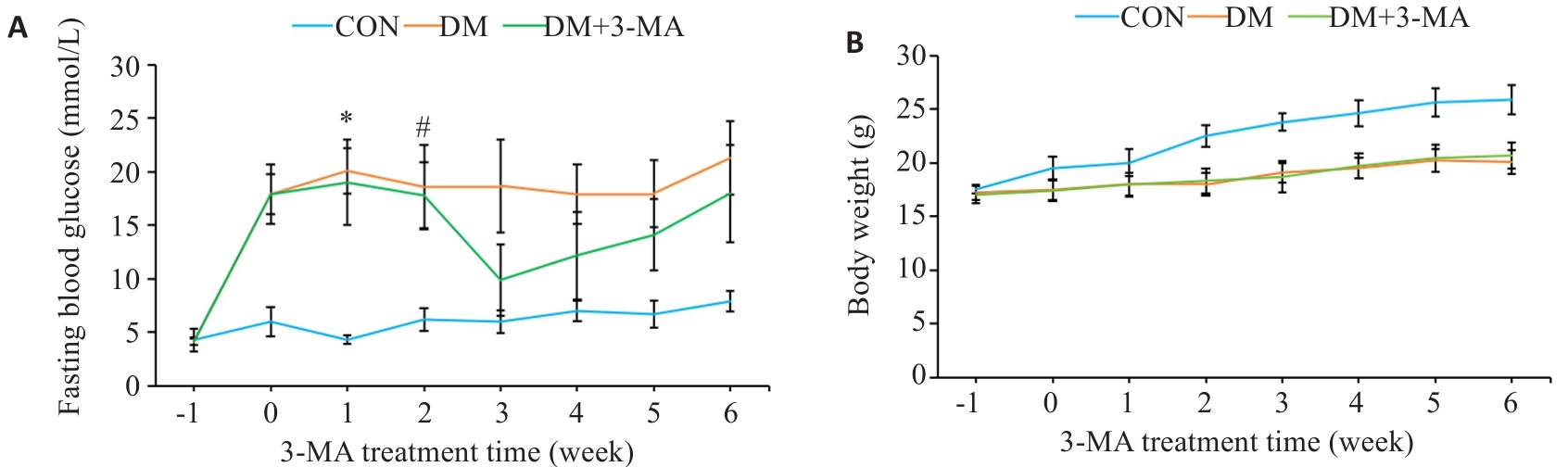
Fig.1 Effects of 3-MA on fasting blood glucose and body weight of diabetic mice (Mean±SD, n=8). A: Fasting blood glucose. B: Body weight. *P<0.001 vs CON group; #P<0.001 vs DM+3-MA group.
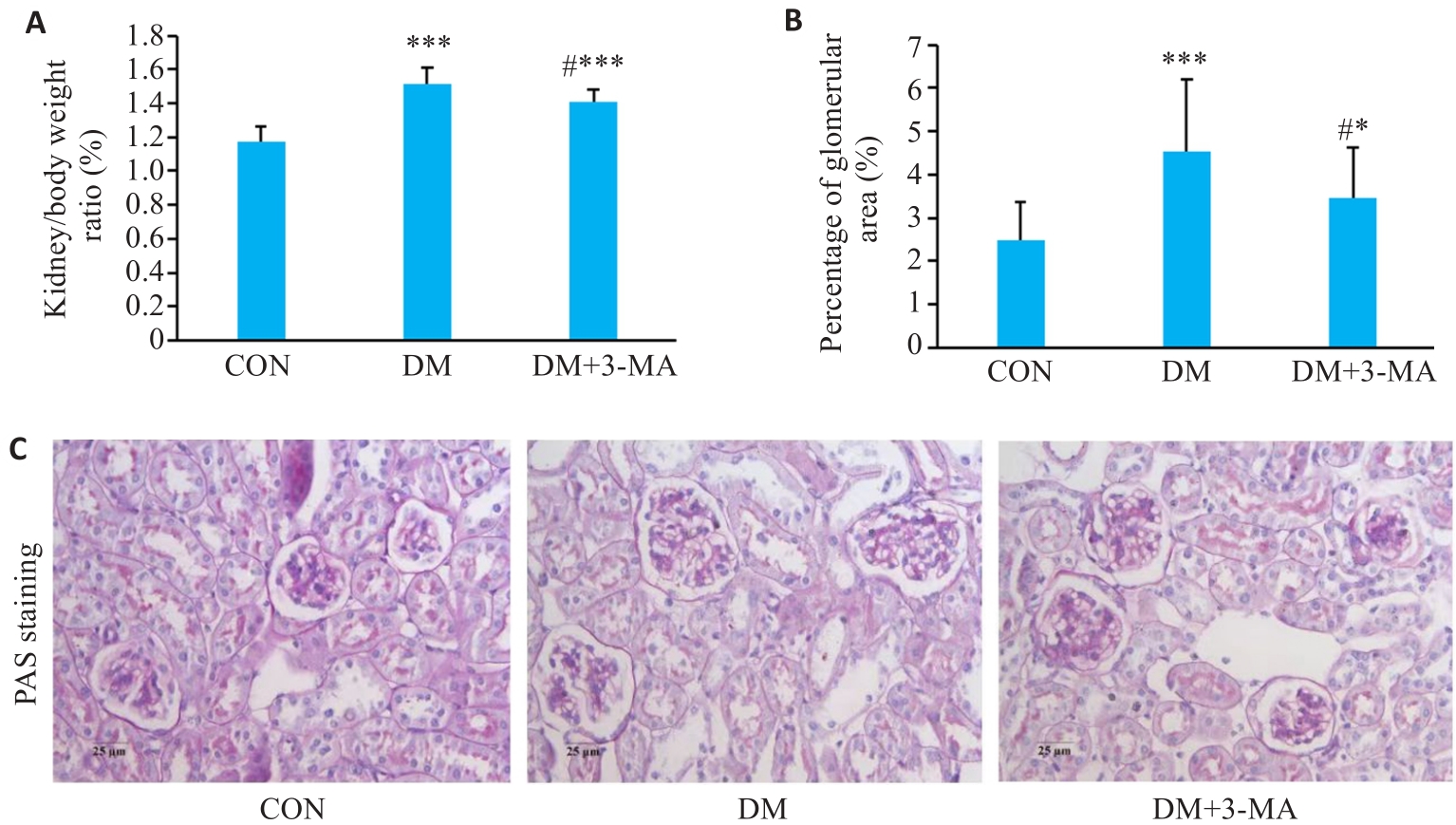
Fig.2 Effects of 3-MA on kidney/body weight ratio and glomerular size of diabetic mice (Mean±SD, n=8). A: Kidney/body weight ratio. B: Percentage of glomerular area to field of view. C: Pepresentative images of PAS staining (Original magnification: ×400). *P<0.05, ***P<0.001 vs CON group; #P<0.05 vs DM group.
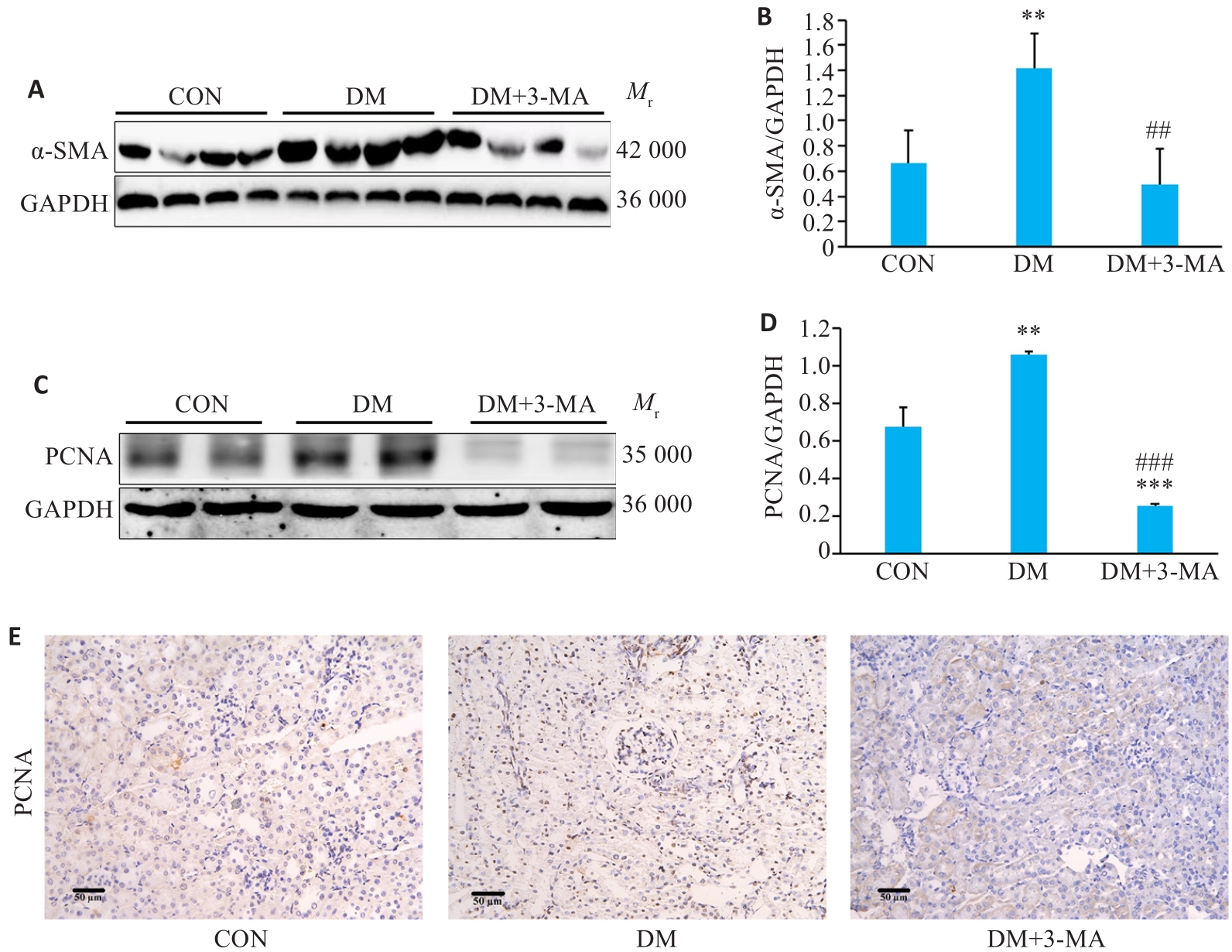
Fig.3 Effects of 3-MA on the protein expressions of α-SMA and PCNA in the renal cortex of the diabetic mice (Mean±SD, n=4). A: Western blotting of α-SMA expression. B: Quantification of α-SMA protein expression. C: Western blotting of PCNA expression. D: Quantification of PCNA protein expression. E: Immunohistochemical staining of PCNA. **P<0.01 vs CON group; ##P<0.01, ###P<0.001 vs DM group.
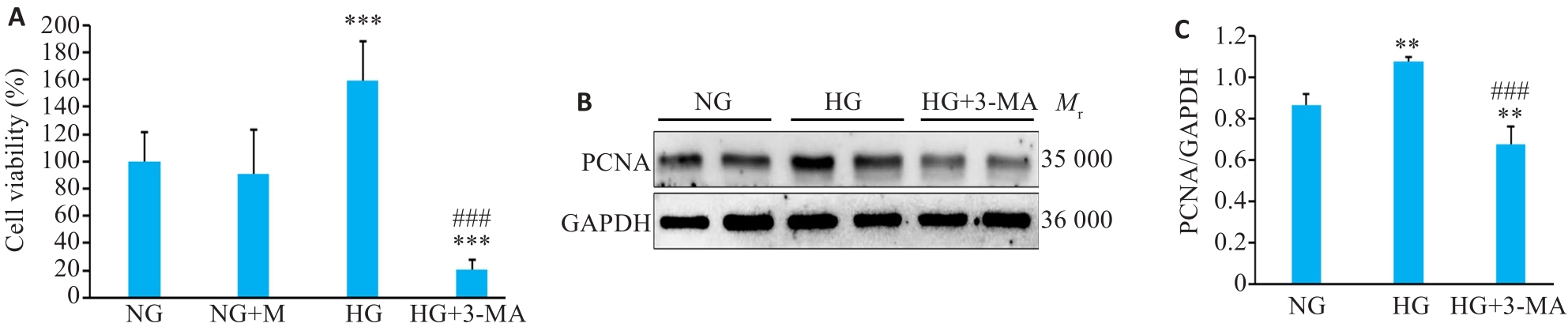
Fig.4 Effects of 3-MA on cell viability and PCNA expression of SV40 MES 13 cells exposed to high glucose (Mean±SD, n=4). A: Cell viability. B: Western blotting of PCNA expression. C: Quantification of PCNA protein expression. **P<0.01, ***P<0.001 vs NG group; ###P<0.001 vs HG group.
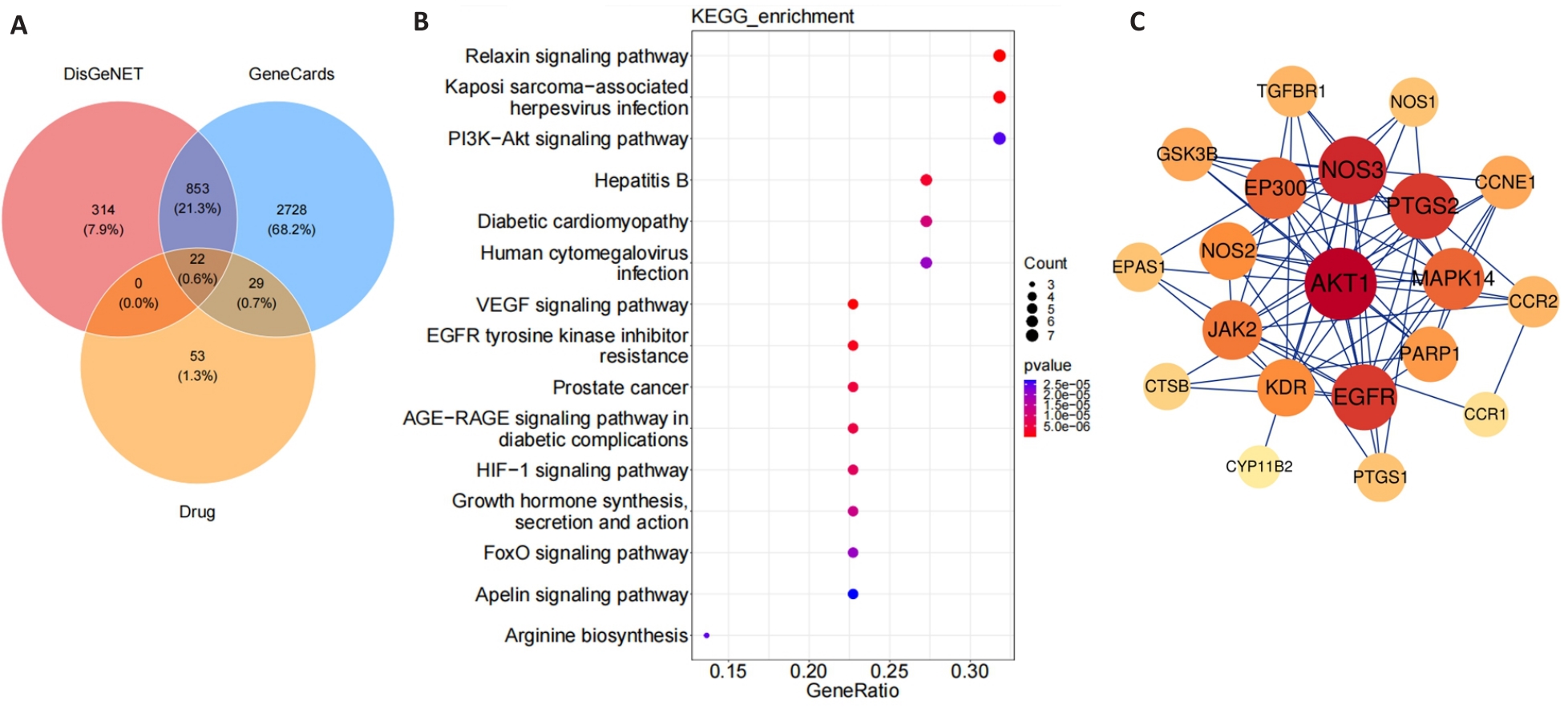
Fig.5 Bioinformatic analysis of 3-MA on diabetic kidney disease. A: Venn diagram of intersecting genes between diabetic kidney disease targets and 3-MA predicted targets. B: KEGG enrichment analysis. C: Protein-protein interaction analysis network.
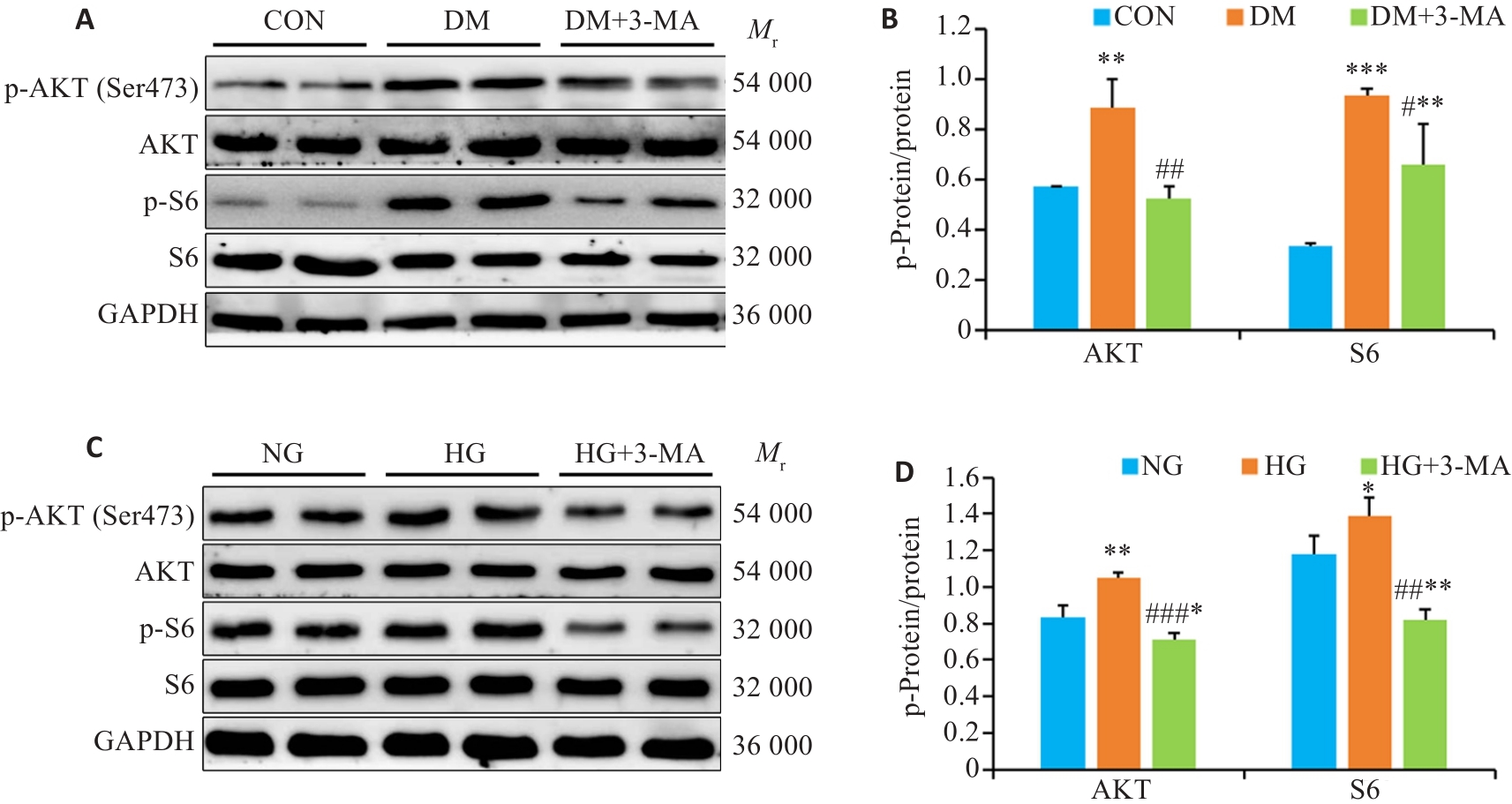
Fig.6 Effects of 3-MA on AKT signaling molecules in diabetic mice and high glucose treated SV40 MES 13 cells (Mean±SD, n=4). A: Western blotting of p-AKT (Ser473), AKT, p-S6, and S6 in the renal cortex of mice. B: Quantification of the ratio of p-AKT/AKT and p-S6/S6 in the renal cortex of mice. C: Western blotting of p-AKT (Ser473), AKT, p-S6, and S6 in SV40 MES 13 cells. D: Quantification of the ratio of p-AKT/AKT and p-S6/S6 in SV40 MES 13 cells. *P<0.05, **P<0.01, ***P<0.001 vs CON or NG group; #P<0.05, ##P<0.01, ###P<0.001 vs DM or HG group.
| 1 | Tuttle KR, Bakris GL, Bilous RW, et al. Diabetic kidney disease: a report from an ADA Consensus Conference[J]. Diabetes Care, 2014, 37(10): 2864-83. |
| 2 | Attie AD, Schueler KM, Keller MP, et al. Reversal of hypertriglyceridemia in diabetic BTBR ob/ob mice does not prevent nephropathy[J]. Lab Invest, 2021, 101(7): 935-41. |
| 3 | Mason RM, Wahab NA. Extracellular matrix metabolism in diabetic nephropathy[J]. J Am Soc Nephrol, 2003, 14(5): 1358-73. |
| 4 | A/L B Vasanth Rao VR, Tan SH, Candasamy M, et al. Diabetic nephropathy: an update on pathogenesis and drug development[J]. Diabetes Metab Syndr, 2019, 13(1): 754-62. |
| 5 | Seglen PO, Gordon PB. 3-Methyladenine: specific inhibitor of autophagic/lysosomal protein degradation in isolated rat hepatocytes[J]. Proc Natl Acad Sci U S A, 1982, 79(6): 1889-92. |
| 6 | 刘本菊, 任海文, 王 朵, 等. 3-甲基腺嘌呤抑制VEGF信号减轻早期糖尿病肾病细胞外基质沉积[J]. 中华内分泌代谢杂志, 2023, 39(10): 876-81. |
| 7 | Ren HW, Yu W, Wang YN, et al. Effects of autophagy inhibitor 3-methyladenine on a diabetic mice model[J]. Int J Ophthalmol, 2023, 16(9): 1456-64. |
| 8 | Dai S, Wang B, Li W, et al. Systemic application of 3-methyladenine markedly inhibited atherosclerotic lesion in ApoE-/- mice by modulating autophagy, foam cell formation and immune-negative molecules[J]. Cell Death Dis, 2016, 7(12): e2498. |
| 9 | Slavin SA, Leonard A, Grose V, et al. Autophagy inhibitor 3-methyladenine protects against endothelial cell barrier dysfunction in acute lung injury[J]. Am J Physiol Lung Cell Mol Physiol, 2018, 314(3): L388-L396. |
| 10 | Liu H, Lei H, Shi Y, et al. Autophagy inhibitor 3-methyladenine alleviates overload-exercise-induced cardiac injury in rats[J]. Acta Pharmacol Sin, 2017, 38(7): 990-7. |
| 11 | Wang XR, Wu YY. Protective effects of autophagy inhibitor 3-methyladenine on ischemia-reperfusion-induced retinal injury[J]. Int Ophthalmol, 2020, 40(5): 1095-101. |
| 12 | Kwon Y, Haam CE, Byeon S, et al. Effects of 3-methyladenine, an autophagy inhibitor, on the elevated blood pressure and arterial dysfunction of angiotensin II-induced hypertensive mice[J]. Biomedecine Pharmacother, 2022, 154: 113588. |
| 13 | Wang XH, Zhou GX, Liu C, et al. Acanthopanax versus 3-methyladenine ameliorates sodium taurocholate-induced severe acute pancreatitis by inhibiting the autophagic pathway in rats[J]. Mediators Inflamm, 2016: 8369704. |
| 14 | Shi YF, Tao M, Ma XY, et al. Delayed treatment with an autophagy inhibitor 3-MA alleviates the progression of hyperuricemic nephropathy[J]. Cell Death Dis, 2020, 11(6): 467. |
| 15 | Qian X, He LL, Hao M, et al. YAP mediates the interaction between the Hippo and PI3K/Akt pathways in mesangial cell proliferation in diabetic nephropathy[J]. Acta Diabetol, 2021, 58(1): 47-62. |
| 16 | Tan HT, Chen JX, Li YC, et al. Glabridin, a bioactive component of licorice, ameliorates diabetic nephropathy by regulating ferroptosis and the VEGF/Akt/ERK pathways[J]. Mol Med, 2022, 28(1): 58. |
| 17 | Tang D, He WJ, Zhang ZT, et al. Protective effects of Huang-Lian-Jie-Du Decoction on diabetic nephropathy through regulating AGEs/RAGE/Akt/Nrf2 pathway and metabolic profiling in db/db mice[J]. Phytomedicine, 2022, 95: 153777. |
| 18 | Wu W, Hu W, Han WB, et al. Inhibition of akt/mTOR/p70S6K signaling activity with Huangkui capsule alleviates the early glomerular pathological changes in diabetic nephropathy[J]. Front Pharmacol, 2018, 9: 443. |
| 19 | Johnson RJ, Floege J, Yoshimura A, et al. The activated mesangial cell: a glomerular "myofibroblast"[J]? J Am Soc Nephrol, 1992, 2(10 ): S190-7. |
| 20 | Young BA, Johnson RJ, Alpers CE, et al. Cellular events in the evolution of experimental diabetic nephropathy[J]. Kidney Int, 1995, 47(3): 935-44. |
| 21 | Wang MG, Shi QL, Zhang RZ, et al. Herbal compound “jiedu Huayu” reduces liver injury in rats via regulation of IL-2, TLR4, and PCNA expression levels[J]. Evid Based Complement Alternat Med, 2017: 9819350. |
| 22 | Thomas MC, Brownlee M, Susztak K, et al. Diabetic kidney disease[J]. Nat Rev Dis Primers, 2015, 1: 15018. |
| 23 | Heckmann BL, Yang XY, Zhang XD, et al. The autophagic inhibitor 3-methyladenine potently stimulates PKA-dependent lipolysis in adipocytes[J]. Br J Pharmacol, 2013, 168(1): 163-71. |
| 24 | Sheng Y, Sun B, Guo WT, et al. 3-Methyladenine induces cell death and its interaction with chemotherapeutic drugs is independent of autophagy[J]. Biochem Biophys Res Commun, 2013, 432(1): 5-9. |
| 25 | Jung JY, Choi H, Son ED, et al. 3-methyladenine inhibits procollagen-1 and fibronectin expression in dermal fibroblasts independent of autophagy[J]. Curr Mol Med, 2020, 20(9): 741-50. |
| 26 | Ichinose K, Kawasaki E, Eguchi K. Recent advancement of understanding pathogenesis of type 1 diabetes and potential relevance to diabetic nephropathy[J]. Am J Nephrol, 2007, 27(6): 554-64. |
| 27 | Lin W, Pan J, Huang EJ, et al. Ginkgetin alleviates high glucose-evoked mesangial cell oxidative stress injury, inflammation, and extracellular matrix (ECM) deposition in an AMPK/mTOR-mediated autophagy axis[J]. Chem Biol Drug Des, 2021, 98(4): 620-30. |
| 28 | Wang XL, Gao YB, Tian NX, et al. Astragaloside IV represses high glucose-induced mesangial cells activation by enhancing autophagy via SIRT1 deacetylation of NF-κB p65 subunit[J]. Drug Des Devel Ther, 2018, 12: 2971-80. |
| 29 | Alessi DR, James SR, Downes CP, et al. Characterization of a 3-phosphoinositide-dependent protein kinase which phosphorylates and activates protein kinase Balpha[J]. Curr Biol, 1997, 7(4): 261-9. |
| 30 | Wu YT, Tan HL, Shui GH, et al. Dual role of 3-methyladenine in modulation of autophagy via different temporal patterns of inhibition on class I and III phosphoinositide 3-kinase[J]. J Biol Chem, 2010, 285(14): 10850-61. |
| 31 | Fioretto P, Bruseghin M, Berto I, et al. Renal protection in diabetes: role of glycemic control[J]. J Am Soc Nephrol, 2006, 17(4 ): S86-9. |
| 32 | Boland BB, Alarcón C, Ali A, et al. Monomethylated-adenines potentiate glucose-induced insulin production and secretion via inhibition of phosphodiesterase activity in rat pancreatic islets[J]. Islets, 2015, 7(2): e1073435. |
| [1] | Jinjin WANG, Wenfei CUI, Xuewei DOU, Binglei YIN, Yuqi NIU, Ling NIU, Guoli YAN. Euonymus alatus delays progression of diabetic kidney disease in mice by regulating EGFR tyrosine kinase inhibitor resistance signaling pathway [J]. Journal of Southern Medical University, 2024, 44(7): 1243-1255. |
| [2] | WU Xianan, YANG Ming, GUO Wentao, HU Jie, DONG Ke, GAO Zhaowei. CD5L is elevated in the serum of patients with candidemia and promotes disease progression in mouse models [J]. Journal of Southern Medical University, 2023, 43(3): 368-374. |
| [3] | WAN Lu, QIAN Yuchi, NI Wenjing, LU Yuxin, LI Wei, PAN Yan, CHEN Weidong. Linagliptin improves diabetic kidney disease in rats by promoting mitochondrial biogenesis through the AMPK/PGC-1α/TFAM pathway [J]. Journal of Southern Medical University, 2023, 43(12): 2053-2060. |
| [4] | REN Yi, LU Jinying, YU Lu, LI Zongzhe, WANG Gao, YANG Jing. Carnosine protects against diabetic nephropathy in rats by activating the AKT/mTOR pathway and restoring autophagy in the renal tissue [J]. Journal of Southern Medical University, 2023, 43(11): 1965-1970. |
| [5] | XING Lei, XING wenwen, GUO Hongmin. Exploring the therapeutic mechanism of Longqi Fang for diabetic kidney disease based on network pharmacology and verification in rats [J]. Journal of Southern Medical University, 2022, 42(2): 171-180. |
| [6] | ZHANG Shu, SU Baolin, WANG Liangliang, TANG Shuifu, CHEN Gangyi. Tanshinone IIA alleviates lipopolysaccharide-induced renal tubular epithelial cell apoptosis by inhibiting RIP3/FUNDC1 signaling pathway [J]. Journal of Southern Medical University, 2022, 42(12): 1852-1857. |
| [7] | LI Zhiyang, LIANG Dan, XIAO Yawen, DAI Yunli, AI Fujun, DING Jing, SHI Mingjun, XIAO Ying, GUO Bing. Oxymatrine improves renal fibrosis and inflammation in diabetic rats by modulating CHK1/2 phosphorylation [J]. Journal of Southern Medical University, 2021, 41(10): 1519-1526. |
| [8] | . Arctiin antagonizes triptolide-induced renal toxicity in rats via anti-inflammatory pathway [J]. Journal of Southern Medical University, 2020, 40(10): 1399-1405. |
| [9] |
.
Effects of beraprost sodium on extracellular matrix metabolism in cultured rat mesangial cells induced by high glucose [J]. Journal of Southern Medical University, 2013, 33(12): 1819-. |
| [10] | . Role of TRB3 in the inhibitory effect of fenofibrate against high glucose-induced proliferation of glomerular mesangial cells [J]. Journal of Southern Medical University, 2013, 33(03): 391-. |
| [11] | . Effects of Qufengtongluo Recipe on expressions of cell cycle regulatory proteins in rat mesangial cells [J]. Journal of Southern Medical University, 2012, 32(12): 1699-. |
| [12] | . Protective effect of amlodipine against contrast agent-induced renal injury in elderly patients with coronary heart disease [J]. Journal of Southern Medical University, 2012, 32(11): 1580-. |
| [13] | ZHENG Yong1, LIU Zhi-quan1, YE Tao1, HE Lan2, WANG Yi2, FANG Yuan1, LI Jian- ning2, LIU Ping2, YE Feng2. Effect of high salt diet on expression of osteopontin mRNA in [J]. Journal of Southern Medical University, 2005, 25(05): 595-597. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||