南方医科大学学报 ›› 2025, Vol. 45 ›› Issue (5): 1074-1081.doi: 10.12122/j.issn.1673-4254.2025.05.21
张柳攀1,2( ), 石晓彤3, 李露兰1, 师瑞4, 安胜利3, 曾振华1(
), 石晓彤3, 李露兰1, 师瑞4, 安胜利3, 曾振华1( )
)
收稿日期:2025-02-06
出版日期:2025-05-20
发布日期:2025-05-23
通讯作者:
曾振华
E-mail:50804260@qq.com;zhenhuazeng.2008@163.com
作者简介:张柳攀,硕士,主治医师,E-mail: 50804260@qq.com
基金资助:
Liupan ZHANG1,2( ), Xiaotong SHI3, Lulan LI1, Rui SHI4, Shengli AN3, Zhenhua ZENG1(
), Xiaotong SHI3, Lulan LI1, Rui SHI4, Shengli AN3, Zhenhua ZENG1( )
)
Received:2025-02-06
Online:2025-05-20
Published:2025-05-23
Contact:
Zhenhua ZENG
E-mail:50804260@qq.com;zhenhuazeng.2008@163.com
Supported by:摘要:
目的 探讨危重症急性肾损伤(AKI)患者输注人血白蛋白后不同血清白蛋白水平与28 d死亡率的关系及其对90 d死亡率、液体出入量、持续肾脏替代治疗、机械通气比例及时间等的影响。 方法 回顾性纳入MIMIC IV数据库(2008~2019年)5918例在ICU内接受白蛋白治疗的AKI患者的资料,根据输注后72 h内血清白蛋白水平将其分为低白蛋白组(LA,<30 g/L)、中等白蛋白组(MA,30~35 g/L)和高白蛋白组(HA,>35 g/L) 3组,采用限制性立方样条回归及多因素Logistic回归分析白蛋白水平与死亡率的关系。另纳入南方医科大学南方医院2017年1月~2022年2月的110例脓毒症AKI患者作为外部验证队列,通过生存分析和多因素校正验证结果。 结果 在MIMIC训练队列中,多因素Logistic回归分析显示不同白蛋白分组与危重症AKI患者28 d死亡率无相关性(P>0.05),但限制性立方样条分析提示白蛋白水平与28 d死亡率呈非线性剂量反应关系(阈值效应:>36 g/L时风险升高)。次要终点分析显示,与LA组相比,HA组机械通气时间更短(P<0.001),但ICU住院时间延长(P<0.001)。外部验证队列中,白蛋白水平≥30 g/L与28 d死亡率降低相关(P<0.05)。 结论 输注人血白蛋白以提高血清白蛋白水平与AKI危重患者28 d死亡率的关系存在队列依赖性,可能受疾病类型及严重程度、输注策略及统计方法等多因素影响。
张柳攀, 石晓彤, 李露兰, 师瑞, 安胜利, 曾振华. 合并急性肾损伤的危重症患者输注白蛋白后血清白蛋白水平与28 d死亡率的相关性[J]. 南方医科大学学报, 2025, 45(5): 1074-1081.
Liupan ZHANG, Xiaotong SHI, Lulan LI, Rui SHI, Shengli AN, Zhenhua ZENG. Association between serum albumin levels after albumin infusion and 28-day mortality in critically ill patients with acute kidney injury[J]. Journal of Southern Medical University, 2025, 45(5): 1074-1081.
| Variable | Total (n=7126) | NKD (n=1208) | AKI (n=5918) | P |
|---|---|---|---|---|
| Age [year, Median (P25, P75)] | 68.05(58.97, 76.40) | 66.11(58.17, 73.55) | 68.49(59.21, 76.95) | <0.001 |
| Female [n (%)] | 2785(39.08) | 403(33.36) | 2382(40.25) | <0.001 |
| Emergency [n (%)] | 2148 (30.14) | 210 (17.38) | 1938 (32.75) | <0.001 |
| Weight [kg, Median (P25, P75)] | 80.25(68.50, 94.30) | 74.80 (65.00, 85.40) | 81.80 (69.60, 96.30) | <0.001 |
| Height (cm, Mean±SD) | 169.96±10.51 | 169.98±10.26 | 169.96±10.56 | 0.953 |
| Comorbidity [n (%)] | ||||
| Diabetes | 1861 (26.12) | 287 (23.76) | 1574 (26.60) | 0.044 |
| Coronary atherosclerotic heart disease | 3757 (52.72) | 729 (60.35) | 3028 (51.17) | <0.001 |
| Hypertension | 4346 (60.99) | 742 (61.42) | 3604 (60.90) | 0.758 |
| Cerebral Infarction | 202 (2.83) | 13 (1.08) | 189 (3.19) | <0.001 |
| Heart failure | 1619 (22.72) | 190 (15.73) | 1429 (24.15) | <0.001 |
| Cancer | 680 (9.54) | 91 (7.53) | 589 (9.95) | 0.011 |
| Gastrointestinal related diseases | 365 (5.12) | 33 (2.73) | 332 (5.61) | <0.001 |
| Chronic obstructive pulmonary disease | 1606 (22.54) | 245 (20.28) | 1361 (23.00) | 0.043 |
| Sepsis | 4379 (61.45) | 594 (49.17) | 3785 (63.96) | <0.001 |
| Burns | 8 (0.11) | 0 (0.00) | 8 (0.14) | 0.420 |
| RR [min, Median (P25, P75)] | 16.00 (14.00, 19.00) | 16.00 (14.00, 17.00) | 16.00 (14.00, 20.00) | <0.001 |
| HR [b/min, Median (P25, P75)] | 82.00 (76.00, 94.00) | 80.00 (75.00, 88.00) | 83.00 (77.00, 95.00) | <0.001 |
| T [°C, Median (P25, P75)] | 36.50 (36.00, 36.83) | 36.44 (35.80, 36.72) | 36.50 (36.10, 36.83) | <0.001 |
| MAP [mmHg, Median (P25, P75)] | 77.00 (69.00, 87.00) | 78.00 (70.00, 86.00) | 77.00 (68.00, 87.00) | 0.633 |
| SpO2 [%, Median (P25, P75)] | 100.00 (98.00, 100.00) | 100.00 (99.00, 100.00) | 100.00 (97.00, 100.00) | <0.001 |
| Albumin level (g/dL, Mean±SD) | 2.84±0.72 | 3.02±0.74 | 2.83±0.72 | 0.002 |
| WBCs [×109, Median (P25, P75)] | 11.80 (8.40, 16.10) | 11.50 (8.45, 15.45) | 11.90 (8.40, 16.30) | 0.105 |
| Hemoglobin, [g/dL, Median (P25, P75)] | 11.90 (10.10, 13.30) | 12.50 (11.10, 13.60) | 11.70 (10.00, 13.20) | <0.001 |
| PLT [×109, Median (P25, P75)] | 157.00 (117.00, 216.00) | 150.00 (116.00, 195.00) | 159.00 (117.00, 222.00) | <0.001 |
| Glucose [mg/dL, Median (P25, P75)] | 114.00 (99.00, 146.00) | 107.00 (96.00, 131.00) | 115.00 (100.00, 149.00) | <0.001 |
| Cr [mg/dL, Median (P25, P75)] | 0.90 (0.70, 1.10) | 0.80 (0.60, 0.90) | 0.90 (0.70, 1.10) | <0.001 |
| Lac [mmol/L, Median (P25, P75)] | 1.50 (1.10, 2.10) | 1.40 (1.10, 1.80) | 1.50 (1.10, 2.20) | <0.001 |
| SAPS II [Median (P25, P75)] | 38.00 (31.00, 46.00) | 33.00 (28.00, 40.00) | 39.00 (32.00, 48.00) | <0.001 |
| SOFA [Median (P25, P75)] | 6.00 (4.00, 9.00) | 5.00 (4.00, 7.00) | 7.00 (5.00, 9.00) | <0.001 |
| CCI [Median (P25, P75)] | 4.00 (3.00, 5.00) | 3.00 (2.00, 5.00) | 4.00 (3.00, 6.00) | <0.001 |
| GCS [Median (P25, P75)] | 14.00 (11.00, 15.00) | 15.00 (14.00, 15.00) | 14.00 (11.00, 15.00) | <0.001 |
Fluid input within 24 h [mL, Median (P25, P75)] | 11188.35 (8524.44, 14410.81) | 10332.90 (8432.29, 12367.03) | 11415.04 (8575.50, 15023.15) | <0.001 |
Fluid output within 24 h [mL, Median (P25, P75)] | 2775.00 (1975.00, 3717.00) | 3550.00 (2836.25, 4380.75) | 2601.00 (1830.00, 3529.50) | <0.001 |
表 1 训练队列NKD组和AKI组患者的基线特征
Tab.1 Baseline characteristics of the patients with normal kidney function (NKD) and those with acute kidney injury (AKI) in the training cohort
| Variable | Total (n=7126) | NKD (n=1208) | AKI (n=5918) | P |
|---|---|---|---|---|
| Age [year, Median (P25, P75)] | 68.05(58.97, 76.40) | 66.11(58.17, 73.55) | 68.49(59.21, 76.95) | <0.001 |
| Female [n (%)] | 2785(39.08) | 403(33.36) | 2382(40.25) | <0.001 |
| Emergency [n (%)] | 2148 (30.14) | 210 (17.38) | 1938 (32.75) | <0.001 |
| Weight [kg, Median (P25, P75)] | 80.25(68.50, 94.30) | 74.80 (65.00, 85.40) | 81.80 (69.60, 96.30) | <0.001 |
| Height (cm, Mean±SD) | 169.96±10.51 | 169.98±10.26 | 169.96±10.56 | 0.953 |
| Comorbidity [n (%)] | ||||
| Diabetes | 1861 (26.12) | 287 (23.76) | 1574 (26.60) | 0.044 |
| Coronary atherosclerotic heart disease | 3757 (52.72) | 729 (60.35) | 3028 (51.17) | <0.001 |
| Hypertension | 4346 (60.99) | 742 (61.42) | 3604 (60.90) | 0.758 |
| Cerebral Infarction | 202 (2.83) | 13 (1.08) | 189 (3.19) | <0.001 |
| Heart failure | 1619 (22.72) | 190 (15.73) | 1429 (24.15) | <0.001 |
| Cancer | 680 (9.54) | 91 (7.53) | 589 (9.95) | 0.011 |
| Gastrointestinal related diseases | 365 (5.12) | 33 (2.73) | 332 (5.61) | <0.001 |
| Chronic obstructive pulmonary disease | 1606 (22.54) | 245 (20.28) | 1361 (23.00) | 0.043 |
| Sepsis | 4379 (61.45) | 594 (49.17) | 3785 (63.96) | <0.001 |
| Burns | 8 (0.11) | 0 (0.00) | 8 (0.14) | 0.420 |
| RR [min, Median (P25, P75)] | 16.00 (14.00, 19.00) | 16.00 (14.00, 17.00) | 16.00 (14.00, 20.00) | <0.001 |
| HR [b/min, Median (P25, P75)] | 82.00 (76.00, 94.00) | 80.00 (75.00, 88.00) | 83.00 (77.00, 95.00) | <0.001 |
| T [°C, Median (P25, P75)] | 36.50 (36.00, 36.83) | 36.44 (35.80, 36.72) | 36.50 (36.10, 36.83) | <0.001 |
| MAP [mmHg, Median (P25, P75)] | 77.00 (69.00, 87.00) | 78.00 (70.00, 86.00) | 77.00 (68.00, 87.00) | 0.633 |
| SpO2 [%, Median (P25, P75)] | 100.00 (98.00, 100.00) | 100.00 (99.00, 100.00) | 100.00 (97.00, 100.00) | <0.001 |
| Albumin level (g/dL, Mean±SD) | 2.84±0.72 | 3.02±0.74 | 2.83±0.72 | 0.002 |
| WBCs [×109, Median (P25, P75)] | 11.80 (8.40, 16.10) | 11.50 (8.45, 15.45) | 11.90 (8.40, 16.30) | 0.105 |
| Hemoglobin, [g/dL, Median (P25, P75)] | 11.90 (10.10, 13.30) | 12.50 (11.10, 13.60) | 11.70 (10.00, 13.20) | <0.001 |
| PLT [×109, Median (P25, P75)] | 157.00 (117.00, 216.00) | 150.00 (116.00, 195.00) | 159.00 (117.00, 222.00) | <0.001 |
| Glucose [mg/dL, Median (P25, P75)] | 114.00 (99.00, 146.00) | 107.00 (96.00, 131.00) | 115.00 (100.00, 149.00) | <0.001 |
| Cr [mg/dL, Median (P25, P75)] | 0.90 (0.70, 1.10) | 0.80 (0.60, 0.90) | 0.90 (0.70, 1.10) | <0.001 |
| Lac [mmol/L, Median (P25, P75)] | 1.50 (1.10, 2.10) | 1.40 (1.10, 1.80) | 1.50 (1.10, 2.20) | <0.001 |
| SAPS II [Median (P25, P75)] | 38.00 (31.00, 46.00) | 33.00 (28.00, 40.00) | 39.00 (32.00, 48.00) | <0.001 |
| SOFA [Median (P25, P75)] | 6.00 (4.00, 9.00) | 5.00 (4.00, 7.00) | 7.00 (5.00, 9.00) | <0.001 |
| CCI [Median (P25, P75)] | 4.00 (3.00, 5.00) | 3.00 (2.00, 5.00) | 4.00 (3.00, 6.00) | <0.001 |
| GCS [Median (P25, P75)] | 14.00 (11.00, 15.00) | 15.00 (14.00, 15.00) | 14.00 (11.00, 15.00) | <0.001 |
Fluid input within 24 h [mL, Median (P25, P75)] | 11188.35 (8524.44, 14410.81) | 10332.90 (8432.29, 12367.03) | 11415.04 (8575.50, 15023.15) | <0.001 |
Fluid output within 24 h [mL, Median (P25, P75)] | 2775.00 (1975.00, 3717.00) | 3550.00 (2836.25, 4380.75) | 2601.00 (1830.00, 3529.50) | <0.001 |
| Outcome | Total (n=7126) | NKD (n=1208) | AKI (n=5918) | P |
|---|---|---|---|---|
| Ventilation [n (%)] | 5506 (77.27) | 877 (72.60) | 4629 (78.22) | <0.001 |
| Duration of ventilation [h, Median (P25, P75)] | 9.38 (3.00, 26.00) | 5.73 (0.00, 11.00) | 11.05 (3.50, 35.30) | <0.001 |
| CRRT [n (%)] | 286 (4.01) | 0 (0.00) | 286 (4.83) | <0.001 |
| Length of ICU [day, Median (P25, P75)] | 2.53 (1.46, 4.85) | 1.35 (1.20, 2.17) | 3.05 (1.91, 5.40) | <0.001 |
| Length of hospital stay [day, Median (P25, P75)] | 8.23 (5.77, 13.75) | 6.31 (4.99, 8.88) | 8.93 (6.06, 15.03) | <0.001 |
| 28 d mortality [n (%)] | 682 (9.57) | 16 (1.32) | 666 (11.25) | <0.001 |
| 90 d mortality [n (%)] | 932 (13.08) | 37 (3.06) | 895 (15.12) | <0.001 |
表 2 训练队列NKD组和AKI组患者的研究终点比较
Tab.2 Comparison of outcomes between NKD and AKI groups in the training cohort
| Outcome | Total (n=7126) | NKD (n=1208) | AKI (n=5918) | P |
|---|---|---|---|---|
| Ventilation [n (%)] | 5506 (77.27) | 877 (72.60) | 4629 (78.22) | <0.001 |
| Duration of ventilation [h, Median (P25, P75)] | 9.38 (3.00, 26.00) | 5.73 (0.00, 11.00) | 11.05 (3.50, 35.30) | <0.001 |
| CRRT [n (%)] | 286 (4.01) | 0 (0.00) | 286 (4.83) | <0.001 |
| Length of ICU [day, Median (P25, P75)] | 2.53 (1.46, 4.85) | 1.35 (1.20, 2.17) | 3.05 (1.91, 5.40) | <0.001 |
| Length of hospital stay [day, Median (P25, P75)] | 8.23 (5.77, 13.75) | 6.31 (4.99, 8.88) | 8.93 (6.06, 15.03) | <0.001 |
| 28 d mortality [n (%)] | 682 (9.57) | 16 (1.32) | 666 (11.25) | <0.001 |
| 90 d mortality [n (%)] | 932 (13.08) | 37 (3.06) | 895 (15.12) | <0.001 |
| Outcome | LA (<30 g/L) | MA (30-35 g/L) | HA (>35 g/L) | P |
|---|---|---|---|---|
| CRRT [n (%)] | 139 (17.96) | 50 (16.89) | 32 (24.06) | 0.184 |
| Ventilation [n (%)] | 678 (87.60) | 263 (88.85) | 115 (86.47) | 0.758 |
| Duration of ventilation [h, Median (P25, P75)] | 120.42 (33.07, 254.00) | 68.21 (15.00, 158.76) | 59.00 (15.00, 178.00) | <0.001 |
| Fluid input within 72 h [mL, Median (P25, P75)] | 28821.47 (18874.31, 43478.88) | 24942.46 (17068.04, 37728.76) | 20563.86 (14194.31, 32221.87) | <0.001 |
| Amount of albumin infusion within 72 h [g, Median (P25, P75)] | 37.50 (25.00, 75.00) | 50.00 (25.00, 102.48) | 100.00 (62.50, 187.50) | <0.001 |
| Serum albumin level at 72 h after albumin infusion [g/dL, Median (P25, P75)] | 2.50 (2.10, 2.90) | 2.90 (2.40, 3.40) | 3.30 (2.70, 3.80) | <0.001 |
| Length of ICU stay [d, Median (P25, P75)] | 10.78 (6.17, 17.16) | 8.21 (5.18, 14.39) | 8.84 (5.56, 14.09) | <0.001 |
| Length of hospital stay [d, Median (P25, P75)] | 20.82 (13.82, 30.68) | 15.98 (10.86, 24.36) | 17.78 (11.89, 27.58) | <0.001 |
| 28 d mortality [n (%)] | 176 (22.74) | 63 (21.28) | 33 (24.81) | 0.714 |
| 90 d mortality [n (%)] | 258 (33.33) | 84 (28.38) | 47 (35.34) | 0.221 |
表3 不同白蛋白分组下训练队列AKI危重症患者的结局指标
Tab.3 Outcomes of AKI patients with different albumin levels in the training cohort
| Outcome | LA (<30 g/L) | MA (30-35 g/L) | HA (>35 g/L) | P |
|---|---|---|---|---|
| CRRT [n (%)] | 139 (17.96) | 50 (16.89) | 32 (24.06) | 0.184 |
| Ventilation [n (%)] | 678 (87.60) | 263 (88.85) | 115 (86.47) | 0.758 |
| Duration of ventilation [h, Median (P25, P75)] | 120.42 (33.07, 254.00) | 68.21 (15.00, 158.76) | 59.00 (15.00, 178.00) | <0.001 |
| Fluid input within 72 h [mL, Median (P25, P75)] | 28821.47 (18874.31, 43478.88) | 24942.46 (17068.04, 37728.76) | 20563.86 (14194.31, 32221.87) | <0.001 |
| Amount of albumin infusion within 72 h [g, Median (P25, P75)] | 37.50 (25.00, 75.00) | 50.00 (25.00, 102.48) | 100.00 (62.50, 187.50) | <0.001 |
| Serum albumin level at 72 h after albumin infusion [g/dL, Median (P25, P75)] | 2.50 (2.10, 2.90) | 2.90 (2.40, 3.40) | 3.30 (2.70, 3.80) | <0.001 |
| Length of ICU stay [d, Median (P25, P75)] | 10.78 (6.17, 17.16) | 8.21 (5.18, 14.39) | 8.84 (5.56, 14.09) | <0.001 |
| Length of hospital stay [d, Median (P25, P75)] | 20.82 (13.82, 30.68) | 15.98 (10.86, 24.36) | 17.78 (11.89, 27.58) | <0.001 |
| 28 d mortality [n (%)] | 176 (22.74) | 63 (21.28) | 33 (24.81) | 0.714 |
| 90 d mortality [n (%)] | 258 (33.33) | 84 (28.38) | 47 (35.34) | 0.221 |
| Variable | Model 1 | Model 2 | Model 3 | |||
|---|---|---|---|---|---|---|
| OR (95% CI) | P | OR(95% CI) | P | OR (95% CI) | P | |
| 28-day mortality | 1203 | 1203 | 855 | |||
| All | 1.03 (0.84, 1.27) | 0.768 | 1.04 (0.84, 1.28) | 0.741 | 0.74 (0.51, 1.06) | 0.768 |
| LA | Ref | Ref | Ref | |||
| MA | 0.92 (0.66, 1.27) | 0.609 | 0.93 (0.67, 1.28) | 0.653 | 0.82 (0.48, 1.38) | 0.457 |
| HA | 1.12 (0.72, 1.70) | 0.600 | 1.14 (0.73, 1.73) | 0.562 | 0.91 (0.43, 1.88) | 0.810 |
| 90-day mortality | 1203 | 1203 | 915 | |||
| All | 0.99 (0.82, 1.19) | 0.908 | 0.99 (0.82, 1.20) | 0.946 | 0.89 (0.68, 1.19) | 0.366 |
| LA | Ref | Ref | Ref | |||
| MA | 0.79 (0.59, 1.06) | 0.120 | 0.80 (0.59, 1.07) | 0.133 | 1.21 (0.51, 1.81) | 0.345 |
| HA | 1.09 (0.74, 1.60) | 0.651 | 1.11 (0.75, 1.63) | 0.602 | 0.99 (0.55, 1.73) | 0.964 |
表4 不同白蛋白分组对训练队列AKI危重症患者死亡率的Logistic回归分析
Tab.4 Logistic regression analysis of the association between albumin levels and mortality in critically ill AKI patients in the training cohort
| Variable | Model 1 | Model 2 | Model 3 | |||
|---|---|---|---|---|---|---|
| OR (95% CI) | P | OR(95% CI) | P | OR (95% CI) | P | |
| 28-day mortality | 1203 | 1203 | 855 | |||
| All | 1.03 (0.84, 1.27) | 0.768 | 1.04 (0.84, 1.28) | 0.741 | 0.74 (0.51, 1.06) | 0.768 |
| LA | Ref | Ref | Ref | |||
| MA | 0.92 (0.66, 1.27) | 0.609 | 0.93 (0.67, 1.28) | 0.653 | 0.82 (0.48, 1.38) | 0.457 |
| HA | 1.12 (0.72, 1.70) | 0.600 | 1.14 (0.73, 1.73) | 0.562 | 0.91 (0.43, 1.88) | 0.810 |
| 90-day mortality | 1203 | 1203 | 915 | |||
| All | 0.99 (0.82, 1.19) | 0.908 | 0.99 (0.82, 1.20) | 0.946 | 0.89 (0.68, 1.19) | 0.366 |
| LA | Ref | Ref | Ref | |||
| MA | 0.79 (0.59, 1.06) | 0.120 | 0.80 (0.59, 1.07) | 0.133 | 1.21 (0.51, 1.81) | 0.345 |
| HA | 1.09 (0.74, 1.60) | 0.651 | 1.11 (0.75, 1.63) | 0.602 | 0.99 (0.55, 1.73) | 0.964 |
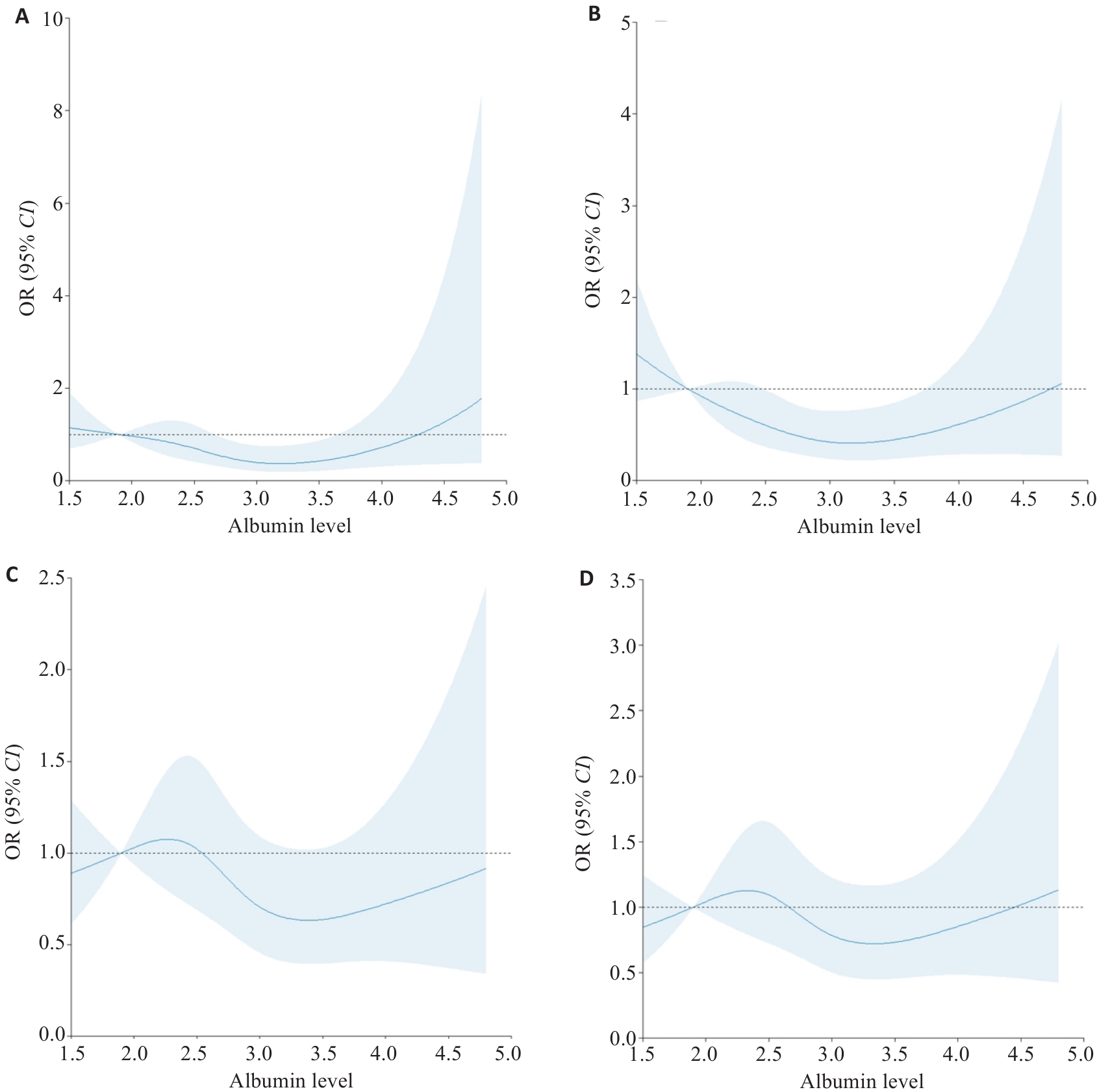
图1 训练队列AKI患者血清白蛋白与28 d 和90 d死亡率的关系
Fig.1 Association between serum albumin level and 28- and 90-day mortality in AKI patients in the training cohort. A,B: 28-day mortality rates of the total population and AKI patients. C, D: 90-day mortality rates of the total population and AKI patients. The OR had been adjusted for the covariates listed in Tab.1.
| Variable | OR (95%CI) | P | aOR (95% CI) | aP |
|---|---|---|---|---|
| Female | 0.35 (0.60, 3.75) | <0.001 | ||
| Diabetes | 0.37(0.45,3.96) | <0.001 | ||
| Hypertension | 0.43(0.32,1.95) | 0.001 | ||
| History of gastrointestinal tumors | 0.36(0.55,5.03) | <0.001 | ||
| History of other gastrointestinal tumors | 0.35(0.67,6.74) | <0.001 | ||
| Albumin level | 0.93 (0.87, 1.00) | 0.035 | ||
| Cr | 0.37(0.99,1.00) | 0.012 | ||
| Lactate | 1.20 (1.04, 1.38) | 0.014 | ||
| APACHE II group | 10.17 (1.30, 79.46) | 0.027 | ||
| MA | 5.99 (1.63, 22.04) | 0.007 | 4.24 (1.09, 16.52) | 0.037 |
| HA | 15.00 (3.22, 69.84) | 0.001 | 13.22(2.33, 75.10) | 0.004 |
表5 外部验证队列下脓毒症AKI患者28 d内死亡的危险因素分析
Tab.5 Risk factors for 28-day mortality in AKI patients with sepsis in the external validation cohort
| Variable | OR (95%CI) | P | aOR (95% CI) | aP |
|---|---|---|---|---|
| Female | 0.35 (0.60, 3.75) | <0.001 | ||
| Diabetes | 0.37(0.45,3.96) | <0.001 | ||
| Hypertension | 0.43(0.32,1.95) | 0.001 | ||
| History of gastrointestinal tumors | 0.36(0.55,5.03) | <0.001 | ||
| History of other gastrointestinal tumors | 0.35(0.67,6.74) | <0.001 | ||
| Albumin level | 0.93 (0.87, 1.00) | 0.035 | ||
| Cr | 0.37(0.99,1.00) | 0.012 | ||
| Lactate | 1.20 (1.04, 1.38) | 0.014 | ||
| APACHE II group | 10.17 (1.30, 79.46) | 0.027 | ||
| MA | 5.99 (1.63, 22.04) | 0.007 | 4.24 (1.09, 16.52) | 0.037 |
| HA | 15.00 (3.22, 69.84) | 0.001 | 13.22(2.33, 75.10) | 0.004 |
| 1 | Guo YF, Qiu Y, Xue TQ, et al. Association between glycemic variability and short-term mortality in patients with acute kidney injury: a retrospective cohort study of the MIMIC-IV database[J]. Sci Rep, 2024, 14(1): 5945. |
| 2 | Koeze J, Keus F, Dieperink W, et al. Incidence, timing and outcome of AKI in critically ill patients varies with the definition used and the addition of urine output criteria[J]. BMC Nephrol, 2017, 18(1): 70. |
| 3 | Ostermann M, Chang RE, Group RIPU. Correlation between the AKI classification and outcome[J]. Crit Care, 2008, 12(6): R144. |
| 4 | Yang C, Lu JT, Shen F, et al. Serum albumin level is associated with mortality and hospital stays: a real-world data analysis[J]. Clin Nutr ESPEN, 2024, 64: 215-20. |
| 5 | Ostermann M, Liu K, Kashani K. Fluid management in acute kidney injury[J]. Chest, 2019, 156(3): 594-603. |
| 6 | Finfer S, Bellomo R, Boyce N, et al. A comparison of albumin and saline for fluid resuscitation in the intensive care unit[J]. N Engl J Med, 2004, 350(22): 2247-56. |
| 7 | Caironi P, Tognoni G, Masson S, et al. Albumin replacement in patients with severe sepsis or septic shock[J]. N Engl J Med, 2014, 370(15): 1412-21. |
| 8 | Ge CL, Peng QY, Chen W, et al. Association between albumin infusion and outcomes in patients with acute kidney injury and septic shock[J]. Sci Rep, 2021, 11(1): 24083. |
| 9 | Vincent JL, Dubois MJ, Navickis RJ, et al. Hypoalbuminemia in acute illness: is there a rationale for intervention? A meta-analysis of cohort studies and controlled trials[J]. Ann Surg, 2003, 237(3): 319-34. |
| 10 | Yang KB, Yang N, Sun WB, et al. The association between albumin and mortality in patients with acute kidney injury: a retrospective observational study[J]. BMC Nephrol, 2023, 24(1): 332. |
| 11 | Wiedermann CJ, Wiedermann W, Joannidis M. Hypoalbuminemia and acute kidney injury: a meta-analysis of observational clinical studies[J]. Intensive Care Med, 2010, 36(10): 1657-65. |
| 12 | Zhang LR, Yu WB, Zhao YW, et al. Albumin infusion may improve the prognosis of critical COVID-19 patients with hypoalbuminemia in the intensive care unit: a retrospective cohort study[J]. Infect Drug Resist, 2022, 15: 6039-50. |
| 13 | Pulimood TB, Park GR. Debate: Albumin administration should be avoided in the critically ill[J]. Crit Care, 2000, 4(3): 151-5. |
| 14 | Li MQ, Ge YD, Wang JJ, et al. Impact of albumin infusion on prognosis in ICU patients with cirrhosis and AKI: insights from the MIMIC-IV database[J]. Front Pharmacol, 2024, 15: 1467752. |
| 15 | Zheng LJ, Jiang WM, Pan LL, et al. Reduced serum albumin as a risk factor for poor prognosis in critically ill patients receiving renal replacement therapy[J]. BMC Nephrol, 2021, 22(1): 305. |
| 16 | Tigabu BM, Davari M, Kebriaeezadeh A, et al. A cost-effectiveness analysis of albumin in septic shock: a patient-level data analysis[J]. Clin Ther, 2019, 41(11): 2297-307.e2. |
| 17 | Raghunathan K, Kempker JA, Anne Davis E, et al. Early albumin infusion is associated with greater survival to discharge among patients with sepsis/septic shock who develop severe acute kidney injury among patients with sepsis/septic shock who develop severe acute kidney injury[J]. Crit Care Explor, 2022, 4(12): e0793. |
| 18 | Shasthry SM, Kumar M, Khumuckham JS, et al. Changes in cardiac output and incidence of volume overload in cirrhotics receiving 20% albumin infusion[J]. Liver Int, 2017, 37(8): 1167-76. |
| 19 | Jiang CF, Wang BY, Li YB, et al. U-shaped association between serum albumin and development of chronic kidney disease in general hypertensive patients[J]. Clin Nutr, 2020, 39(1): 258-64. |
| 20 | Zhang XP, Zhang LF, Wei CZ, et al. U-shaped association between serum albumin and pediatric intensive care unit mortality in critically ill children[J]. Front Nutr, 2022, 9: 931599. |
| 21 | Kim S, McClave SA, Martindale RG, et al. Hypoalbuminemia and clinical outcomes: what is the mechanism behind the relationship?[J]. Am Surg, 2017, 83(11): 1220-7. |
| 22 | Trow AV, Rozanski EA, Delaforcade AM, et al. Evaluation of use of human albumin in critically ill dogs: 73 cases (2003-2006)[J]. J Am Vet Med Assoc, 2008, 233(4): 607-12. |
| 23 | Austin PC, Lee DS, Fine JP. Introduction to the analysis of survival data in the presence of competing risks[J]. Circulation, 2016, 133(6): 601-9. |
| 24 | Dubois MJ, Orellana-Jimenez C, Melot C, et al. Albumin administration improves organ function in critically ill hypo-albuminemic patients: a prospective, randomized, controlled, pilot study[J]. Crit Care Med, 2006, 34(10): 2536-40. |
| 25 | Ye ZW, Gao M, Ge CL, et al. Association between albumin infusion and septic patients with coronary heart disease: a retrospective study based on medical information mart for intensive care III database[J]. Front Cardiovasc Med, 2022, 9: 982969. |
| 26 | Hou L, Wu X, Sun ZG. Risk factors and prognosis of acute kidney injury in hospitalised sepsis patients[J]. Arch Esp Urol, 2024, 77(3): 263-9. |
| 27 | Ji MS, Wu R, Feng Z, et al. Incidence, risk factors and prognosis of acute kidney injury in patients treated with immune checkpoint inhibitors: a retrospective study[J]. Sci Rep, 2022, 12(1): 18752. |
| 28 | Chen XL, Zhou JJ, Wang RC, et al. Blood urea nitrogen to albumin ratio predicts risk of acute kidney injury and in-hospital mortality associated with immunological and surgical diseases: a retrospective analysis of 1994 patients[J]. Int Immunopharmacol, 2024, 143(Pt 3): 113600. |
| 29 | 齐 霜, 毛 智, 胡 新, 等. 基于专科信息系统建立的重症医学数据库: 大型三甲医院重症医学数据库的模式 [J]. 中华危重病急救医学, 2020, 32(6): 743-9. DOI: 10.3760/cma.j.cn121430-20200520-00393 |
| 30 | Qian F, van den Boom W, See KC. The new global definition of acute respiratory distress syndrome: insights from the MIMIC-IV database[J]. Intensive Care Med, 2024, 50(4): 608-9. |
| [1] | 王子皓, 陶丽丽, 邹碧清, 安胜利. 重症监护病房急性肾损伤患者首次24 h动脉氧分压与死亡率相关:基于MIMIC-IV数据库[J]. 南方医科大学学报, 2025, 45(5): 1056-1062. |
| [2] | 房尚萍, 孙任珂, 苏 慧, 翟科程, 项 毓, 高杨梦娜, 郭文俊. 绿原酸减轻脓毒症诱导的小鼠急性肾损伤:基于抑制caspase-1经典细胞焦亡信号通路[J]. 南方医科大学学报, 2024, 44(2): 317-323. |
| [3] | 李佳馨, 刘毅, 刘向杰, 徐龙河, 刘永哲. 肾素-血管紧张素系统可预测腹腔镜肾根治术后的急性肾损伤[J]. 南方医科大学学报, 2024, 44(11): 2220-2226. |
| [4] | 郭晶晶, 张文龙, 梁 飘, 张龙军, 彭凌音, 闵钰琦, 潘小珍, 杨志英, 邓华菲. 葛根素减轻LPS诱导的小鼠急性肾损伤:基于调节SIRT1/NF-κB信号通路[J]. 南方医科大学学报, 2023, 43(7): 1248-1253. |
| [5] | 苏雨薇, 孙 闻, 王 迪, 董钰妍, 丁 莹, 徐龙河, 刘永哲. 右美托咪定不能降低腹腔镜下根治性肾切除术后急性和慢性肾脏病的发病率:基于倾向性评分匹配法[J]. 南方医科大学学报, 2023, 43(4): 654-659. |
| [6] | 张 舒, 苏保林, 王亮亮, 汤水福, 陈刚毅. 丹参酮IIA通过抑制RIP3/FUNDC1信号通路减轻LPS诱导的小鼠肾小管上皮细胞凋亡[J]. 南方医科大学学报, 2022, 42(12): 1852-1857. |
| [7] | 肖冠华, 胡鸿彬, 吴 凤, 沙 桐, 曾振华, 黄巧冰, 李海军, 韩家发, 宋文鸿, 陈仲清, 蔡淑敏. 武汉市COVID-19住院患者急性肾损伤的发生:287例单中心回顾性分析[J]. 南方医科大学学报, 2021, 41(2): 157-163. |
| [8] | 谭继翔,何进,秦文熠,赵林. 槲皮素通过抑制TLR4/NF-κB通路缓解脂多糖诱导的急性肾损伤[J]. 南方医科大学学报, 2019, 39(05): 598-. |
| [9] | 刘崇斌,黄柳维,李彩珍,沈燕婷,王骏. 阻断Pannexin-1 可减轻肾脏组织炎症细胞浸润和缓解顺铂诱导的急性肾损伤[J]. 南方医科大学学报, 2019, 39(05): 508-. |
| [10] | 霍锐,戴敏,樊艺,周竞峥,李莉,祖建. miRNA-29a和miRNA-10a-5p 对脓毒症所致急性肾损伤患者28 d 死亡率的预测价值[J]. 南方医科大学学报, 2017, 37(05): 646-. |
| [11] | 吴光勇,庄恺,刘宇,王知非. 尿肝型脂肪酸结合蛋白在颅脑外伤中应用价值[J]. 南方医科大学学报, 2016, 36(11): 1527-. |
| [12] | 雷莹,聂晟,孙丹华,宾伟,徐欣. 中国危重症住院患者急性肾损伤的流行病学分析[J]. 南方医科大学学报, 2016, 36(06): 744-. |
| [13] | 张颖,刘宁,任青爱,张海峰,谢晓华. 硫氢化钠防治截肢术后大鼠肾脏损伤的机制[J]. 南方医科大学学报, 2013, 33(08): 1146-. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||