南方医科大学学报 ›› 2025, Vol. 45 ›› Issue (7): 1519-1526.doi: 10.12122/j.issn.1673-4254.2025.07.19
常馨月1,2( ), 姚宁宁3, 赵燕1,2, 王银凤4, 王岸聪1,2, 张慧辉1,2, 张静1,2,5(
), 姚宁宁3, 赵燕1,2, 王银凤4, 王岸聪1,2, 张慧辉1,2, 张静1,2,5( )
)
收稿日期:2025-05-31
出版日期:2025-07-20
发布日期:2025-07-17
通讯作者:
张静
E-mail:chang_xy@126.com;2253113841@qq.com
作者简介:常馨月,硕士,主治医师,E-mail: chang_xy@126.com
基金资助:
Xinyue CHANG1,2( ), Ningning YAO3, Yan ZHAO1,2, Yinfeng WANG4, Ancong WANG1,2, Huihui ZHANG1,2, Jing ZHANG1,2,5(
), Ningning YAO3, Yan ZHAO1,2, Yinfeng WANG4, Ancong WANG1,2, Huihui ZHANG1,2, Jing ZHANG1,2,5( )
)
Received:2025-05-31
Online:2025-07-20
Published:2025-07-17
Contact:
Jing ZHANG
E-mail:chang_xy@126.com;2253113841@qq.com
摘要:
目的 评估使用外源性药物(hCG/GnRHa)扳机对卵巢储备减退患者自然周期体外受精/卵胞浆内单精子注射(NC-IVF/ICSI)助孕生殖预后的影响。 方法 回顾性分析2013年1月~2024年1月两家生殖中心的1118个NC-IVF/ICSI周期。采用倾向性评分匹配(PSM)和多因素Logistic回归校正混杂因素,并通过受试者工作特征(ROC)曲线确定扳机日促黄体生成素(LH)阈值。评估指标包括获卵率、2PN受精率、可移植胚胎率、优质胚胎率、新鲜周期临床妊娠率(CPR)及活产率。 结果 经PSM和Logistic回归校正混杂因素后,外源性扳机组在所有结局指标(获卵率、2PN率、可移植胚胎率、优质胚胎率、鲜胚周期临床妊娠率及活产率)上均优于内源性LH组(P<0.05)。年龄分层分析显示,对于全年龄段患者,外源性扳机策略提高了可利用胚胎率及优质胚胎率(P<0.001);在35~39岁亚组中,扳机组患者在获卵率、优质胚胎率、CPR及活产率方面均展现出优势(P<0.05),其中活产率的提升尤为明显(OR=6.25,95% CI:1.34~29.23)。ROC分析确立了决策日LH阈值19.055 mIU/mL(AUC=0.945,特异度=93.3%),该阈值可用于指导临床路径的精准分层。 结论 在卵巢储备减退患者的NC-IVF/ICSI助孕中,采用外源性扳机可全面优化生殖结局,尤其使35~39岁患者获得显著活产获益。依据LH阈值(19.055 mIU/mL)的个体化决策能有效提升胚胎潜能和活产率。
常馨月, 姚宁宁, 赵燕, 王银凤, 王岸聪, 张慧辉, 张静. 外源性药物扳机可改善卵巢功能减退患者自然周期体外受精/卵胞浆内单精子注射助孕的结局:一项倾向性评分匹配及Logistic回归分析[J]. 南方医科大学学报, 2025, 45(7): 1519-1526.
Xinyue CHANG, Ningning YAO, Yan ZHAO, Yinfeng WANG, Ancong WANG, Huihui ZHANG, Jing ZHANG. Exogenous triggering with hCG/GnRHa improves outcomes of natural cycle IVF/ICSI in patients with diminished ovarian reserve: a propensity score matching and logistic regression analysis[J]. Journal of Southern Medical University, 2025, 45(7): 1519-1526.
| Variable | Endogenous LH group (n=397) | Exogenous trigger group (n=721) | P |
|---|---|---|---|
| Center | 0.1898 | ||
| Linyi people's hospital | 374 (94.21%) | 664 (92.09%) | |
| Heze TCM hospital | 23 (5.79%) | 57 (7.91%) | |
| Age (year) | 40.0 (35.0-42.0) | 40.0 (35.0-43.0) | 0.4998 |
| Age group (years) | 0.9400 | ||
| <35 | 99 (24.94%) | 173 (23.99%) | |
| 35-39 | 95 (23.93%) | 175 (24.27%) | |
| ≥40 | 203 (51.13%) | 373 (51.73%) | |
| Infertility type: Primary | 89 (22.42%) | 159 (22.05%) | 0.8881 |
| Infertility duration (years) | 0.58 (0.25-3.08) | 0.83 (0.25-5.50) | 0.0129 |
| BMI (kg/m²) | 23.43 (21.09-25.64) | 23.70 (21.50-25.71) | 0.0504 |
| Basal FSH (mIU/mL) | 11.26 (7.70-17.14) | 9.47 (7.17-14.40) | 0.0002 |
| Basal LH (mIU/mL) | 4.57 (3.20-6.45) | 3.90 (2.64-5.70) | <0.0001 |
| Basal E₂ (pg/mL) | 42.11 (25.00-67.25) | 46.07 (28.83-69.32) | 0.0271 |
| Basal P (ng/mL) | 0.40 (0.29-0.65) | 0.38 (0.25-0.60) | 0.0307 |
| AFC (n) | 1.50 (1.00-3.00) | 1.50 (1.00-2.50) | 0.7408 |
| Trigger day follicle diameter (mm) | 16.50 (15.00-18.00) | 16.00 (14.50-17.00) | 0.0013 |
| Trigger day E₂ (pg/mL) | 195.10 (148.15-261.24) | 228.56 (187.40-295.66) | <0.0001 |
| Trigger day LH (mIU/mL) | 34.43 (22.61-48.27) | 8.88 (6.17-12.35) | <0.0001 |
| Trigger day P (ng/mL) | 0.83 (0.54-1.11) | 0.37 (0.23-0.59) | <0.0001 |
| Endometrial thickness (mm) | 9.00 (7.50-10.40) | 8.00 (7.00-10.00) | <0.0001 |
表1 患者基线特征及促排特征
Tab.1 Baseline and ovarian stimulation characteristics of the patients
| Variable | Endogenous LH group (n=397) | Exogenous trigger group (n=721) | P |
|---|---|---|---|
| Center | 0.1898 | ||
| Linyi people's hospital | 374 (94.21%) | 664 (92.09%) | |
| Heze TCM hospital | 23 (5.79%) | 57 (7.91%) | |
| Age (year) | 40.0 (35.0-42.0) | 40.0 (35.0-43.0) | 0.4998 |
| Age group (years) | 0.9400 | ||
| <35 | 99 (24.94%) | 173 (23.99%) | |
| 35-39 | 95 (23.93%) | 175 (24.27%) | |
| ≥40 | 203 (51.13%) | 373 (51.73%) | |
| Infertility type: Primary | 89 (22.42%) | 159 (22.05%) | 0.8881 |
| Infertility duration (years) | 0.58 (0.25-3.08) | 0.83 (0.25-5.50) | 0.0129 |
| BMI (kg/m²) | 23.43 (21.09-25.64) | 23.70 (21.50-25.71) | 0.0504 |
| Basal FSH (mIU/mL) | 11.26 (7.70-17.14) | 9.47 (7.17-14.40) | 0.0002 |
| Basal LH (mIU/mL) | 4.57 (3.20-6.45) | 3.90 (2.64-5.70) | <0.0001 |
| Basal E₂ (pg/mL) | 42.11 (25.00-67.25) | 46.07 (28.83-69.32) | 0.0271 |
| Basal P (ng/mL) | 0.40 (0.29-0.65) | 0.38 (0.25-0.60) | 0.0307 |
| AFC (n) | 1.50 (1.00-3.00) | 1.50 (1.00-2.50) | 0.7408 |
| Trigger day follicle diameter (mm) | 16.50 (15.00-18.00) | 16.00 (14.50-17.00) | 0.0013 |
| Trigger day E₂ (pg/mL) | 195.10 (148.15-261.24) | 228.56 (187.40-295.66) | <0.0001 |
| Trigger day LH (mIU/mL) | 34.43 (22.61-48.27) | 8.88 (6.17-12.35) | <0.0001 |
| Trigger day P (ng/mL) | 0.83 (0.54-1.11) | 0.37 (0.23-0.59) | <0.0001 |
| Endometrial thickness (mm) | 9.00 (7.50-10.40) | 8.00 (7.00-10.00) | <0.0001 |
| Variable | Endogenous LH group (n=397) | Exogenous trigger group (n=397) | P |
|---|---|---|---|
| Center | 1.0000 | ||
| Linyi people's hospital | 374 (94.21%) | 374 (94.21%) | |
| Heze TCM hospital | 23 (5.79%) | 23 (5.79%) | |
| Age (year) | 40.0 (35.0-42.0) | 40.0 (34.0-43.0) | 0.5198 |
| Age group (years) | 0.6941 | ||
| <35 | 99 (24.94%) | 101 (25.44%) | |
| 35-39 | 95 (23.93%) | 85 (21.41%) | |
| ≥40 | 203 (51.13%) | 211 (53.15%) | |
| Infertility type: Primary | 89 (22.42%) | 89 (22.42%) | 1.0000 |
| Infertility duration (years) | 0.58 (0.25-3.08) | 0.50 (0.25-3.08) | 0.3843 |
| BMI (kg/m²) | 23.43 (21.09-25.64) | 23.40 (21.10-25.70) | 0.5879 |
| Basal FSH (mIU/mL) | 11.26 (7.70-17.14) | 9.45 (7.10-14.57) | 0.0018 |
| Basal E₂ (pg/mL) | 42.11 (25.00-67.25) | 49.01 (30.43-71.20) | 0.0172 |
| Basal P (ng/mL) | 0.40 (0.29-0.65) | 0.40 (0.26-0.63) | 0.4502 |
| Basal LH (mIU/mL) | 4.57 (3.20-6.45) | 4.07 (2.87-5.81) | 0.0002 |
| AFC (n) | 1.50 (1.00-3.00) | 1.50 (1.00-2.50) | 0.6952 |
| Trigger day follicle diameter (mm) | 16.50 (15.00-18.00) | 16.00 (14.50-17.00) | 0.0030 |
| Trigger day E₂ (pg/mL) | 195.10 (148.15-261.24) | 228.78 (190.10-293.50) | <0.0001 |
| Trigger day LH (mIU/mL) | 34.43 (22.61-48.27) | 9.04 (6.20-12.47) | <0.0001 |
| Trigger day P (ng/mL) | 0.83 (0.54-1.11) | 0.39 (0.24-0.59) | <0.0001 |
| Endometrial thickness (mm) | 9.00 (7.50-10.40) | 8.00 (7.00-10.00) | 0.0036 |
表2 患者基线特征及促排特征 (PSM匹配后)
Tab.2 Baseline and ovarian stimulation characteristics after PSM
| Variable | Endogenous LH group (n=397) | Exogenous trigger group (n=397) | P |
|---|---|---|---|
| Center | 1.0000 | ||
| Linyi people's hospital | 374 (94.21%) | 374 (94.21%) | |
| Heze TCM hospital | 23 (5.79%) | 23 (5.79%) | |
| Age (year) | 40.0 (35.0-42.0) | 40.0 (34.0-43.0) | 0.5198 |
| Age group (years) | 0.6941 | ||
| <35 | 99 (24.94%) | 101 (25.44%) | |
| 35-39 | 95 (23.93%) | 85 (21.41%) | |
| ≥40 | 203 (51.13%) | 211 (53.15%) | |
| Infertility type: Primary | 89 (22.42%) | 89 (22.42%) | 1.0000 |
| Infertility duration (years) | 0.58 (0.25-3.08) | 0.50 (0.25-3.08) | 0.3843 |
| BMI (kg/m²) | 23.43 (21.09-25.64) | 23.40 (21.10-25.70) | 0.5879 |
| Basal FSH (mIU/mL) | 11.26 (7.70-17.14) | 9.45 (7.10-14.57) | 0.0018 |
| Basal E₂ (pg/mL) | 42.11 (25.00-67.25) | 49.01 (30.43-71.20) | 0.0172 |
| Basal P (ng/mL) | 0.40 (0.29-0.65) | 0.40 (0.26-0.63) | 0.4502 |
| Basal LH (mIU/mL) | 4.57 (3.20-6.45) | 4.07 (2.87-5.81) | 0.0002 |
| AFC (n) | 1.50 (1.00-3.00) | 1.50 (1.00-2.50) | 0.6952 |
| Trigger day follicle diameter (mm) | 16.50 (15.00-18.00) | 16.00 (14.50-17.00) | 0.0030 |
| Trigger day E₂ (pg/mL) | 195.10 (148.15-261.24) | 228.78 (190.10-293.50) | <0.0001 |
| Trigger day LH (mIU/mL) | 34.43 (22.61-48.27) | 9.04 (6.20-12.47) | <0.0001 |
| Trigger day P (ng/mL) | 0.83 (0.54-1.11) | 0.39 (0.24-0.59) | <0.0001 |
| Endometrial thickness (mm) | 9.00 (7.50-10.40) | 8.00 (7.00-10.00) | 0.0036 |
| Variable | Endogenous LH group (n=397) | Exogenous trigger group (n=397) | P |
|---|---|---|---|
| Oocytes retrieved | 0.0189 | ||
| 0 | 137 (34.51%) | 106 (26.70%) | |
| 1 | 258 (64.99%) | 291 (73.30%) | |
| 2 | 2 (0.50%) | 0 | |
| Fertilization method | 0.0061 | ||
| IVF | 197 (49.62%) | 223 (56.17%) | |
| ICSI | 31 (7.81%) | 46 (11.59%) | |
| 2PN | 101 (25.44%) | 189 (47.61%) | <0.0001 |
| Available embryos | 93 (23.43%) | 186 (46.85%) | <0.0001 |
| High-quality embryos | 44 (11.08%) | 128 (32.24%) | <0.0001 |
| Cycle outcomes | <0.0001 | ||
| Fresh transfer | 45 (11.34%) | 92 (23.17%) | |
| Embryo cryopreservation | 42 (10.58%) | 88 (22.17%) | |
| No available embryos | 287 (72.29%) | 194 (48.87%) | |
| Clinical pregnancy | 9 (2.27%) | 33 (8.31%) | 0.0001 |
| Live birth | 7 (1.76%) | 23 (5.79%) | 0.0029 |
表3 临床结局结局指标 (匹配后)
Tab.3 Clinical outcome measures after propensity score matching [n(%)]
| Variable | Endogenous LH group (n=397) | Exogenous trigger group (n=397) | P |
|---|---|---|---|
| Oocytes retrieved | 0.0189 | ||
| 0 | 137 (34.51%) | 106 (26.70%) | |
| 1 | 258 (64.99%) | 291 (73.30%) | |
| 2 | 2 (0.50%) | 0 | |
| Fertilization method | 0.0061 | ||
| IVF | 197 (49.62%) | 223 (56.17%) | |
| ICSI | 31 (7.81%) | 46 (11.59%) | |
| 2PN | 101 (25.44%) | 189 (47.61%) | <0.0001 |
| Available embryos | 93 (23.43%) | 186 (46.85%) | <0.0001 |
| High-quality embryos | 44 (11.08%) | 128 (32.24%) | <0.0001 |
| Cycle outcomes | <0.0001 | ||
| Fresh transfer | 45 (11.34%) | 92 (23.17%) | |
| Embryo cryopreservation | 42 (10.58%) | 88 (22.17%) | |
| No available embryos | 287 (72.29%) | 194 (48.87%) | |
| Clinical pregnancy | 9 (2.27%) | 33 (8.31%) | 0.0001 |
| Live birth | 7 (1.76%) | 23 (5.79%) | 0.0029 |
| Outcome | Factor | Before PSM | After PSM | ||
|---|---|---|---|---|---|
| OR (95%CI) | P | OR (95%CI) | P | ||
| Retrieved Oocyte number | Exogenous trigger (yes vs no) | 2.04 (1.35-3.08) | 0.0008 | 2.42 (1.53-3.83) | 0.0002 |
| Age (<35 vs 35-39 years) | 1.71 (1.13-2.59) | 0.0117 | - | - | |
| Age (≥40 vs 35-39 years) | 1.28 (0.91-1.79) | 0.1568 | - | - | |
| Infertility duration (years) | - | - | 1.08 (1.02-1.16) | 0.0139 | |
| BMI (kg/m²) | 0.96 (0.92-1.00) | 0.0376 | 0.93 (0.88-0.99) | 0.0176 | |
| Basal FSH (mIU/mL) | 0.97 (0.95-0.98) | <0.0001 | 0.97 (0.95-0.98) | 0.0002 | |
| Decision-day LH (mIU/mL) | 1.01 (1.00-1.02) | 0.0154 | 1.02 (1.01-1.03) | 0.0032 | |
| 2PN | Exogenous trigger (Yes vs No) | 2.32 (1.73-3.11) | <0.0001 | 2.65 (1.91-3.67) | <0.0001 |
| Infertility type (secondary vs primary) | 1.86 (1.33-2.59) | 0.0003 | 2.08 (1.38-3.14) | 0.0004 | |
| BMI (kg/m²) | 0.95 (0.91-0.99) | 0.0240 | - | - | |
| Basal FSH (mIU/mL) | 0.98 (0.96-0.99) | 0.0099 | - | - | |
| Available embryos | Exogenous trigger (Yes vs No) | 2.31 (1.72-3.10) | <0.0001 | 2.72 (1.97-3.78) | <0.0001 |
| Infertility type (secondary vs primary) | 1.56 (1.12-2.16) | 0.0077 | 2.01 (1.34-3.03) | 0.0008 | |
| Basal FSH (mIU/mL) | 0.98 (0.96-1.00) | 0.0118 | - | - | |
| High-quality embryos | Exogenous trigger (Yes vs No) | 3.38 (2.32-4.93) | <0.0001 | 3.78 (2.53-5.67) | <0.0001 |
| Age (<35 vs 35-39 years) | 0.81 (0.52-1.26) | 0.3412 | - | - | |
| Age (≥40 vs 35-39 years) | 0.62 (0.43-0.90) | 0.0108 | - | - | |
| Infertility type (secondary vs primary) | 1.73 (1.14-2.64) | 0.0108 | 2.08 (1.26-3.45) | 0.0044 | |
| Clinical pregnancy | Exogenous trigger (Yes vs No) | 2.95 (1.40-6.24) | 0.0045 | 4.13 (1.86-9.18) | 0.0005 |
| Age (<35 vs 35-39 years) | 0.79 (0.40-1.54) | 0.4882 | 1.14 (0.49-2.62) | 0.7618 | |
| Age (≥40 vs 35-39 years) | 0.25 (0.12-0.50) | 0.0001 | 0.16 (0.07-0.39) | <0.0001 | |
| Infertility type (secondary vs primary) | - | - | 3.97 (1.39-11.31) | 0.0098 | |
| Basal E2 (pg/mL) | 1.00 (1.00-1.01) | 0.0006 | 1.00 (1.00-1.01) | 0.0016 | |
| Live birth | Exogenous trigger (Yes vs No) | 2.94 (1.24-7.00) | 0.0146 | 4.11 (1.64-10.32) | 0.0026 |
| Age (<35 vs 35-39 years) | 1.13 (0.52-2.45) | 0.7535 | 1.31 (0.53-3.22) | 0.5636 | |
| Age (≥40 vs 35-39 years) | 0.13 (0.05-0.34) | <0.0001 | 0.08 (0.02-0.27) | <0.0001 | |
| Infertility type (secondary vs primary) | 3.09 (1.20-7.92) | 0.0191 | 5.90 (1.62-21.53) | 0.0072 | |
| Basal E2 (pg/mL) | 1.00 (1.00-1.01) | 0.0005 | 1.00 (1.00-1.01) | 0.0008 | |
表4 基于logistic回归探讨患者扳机前指标与各结局指标之间的关系
Tab.4 Pre-trigger variables and outcome associations via logistic regression
| Outcome | Factor | Before PSM | After PSM | ||
|---|---|---|---|---|---|
| OR (95%CI) | P | OR (95%CI) | P | ||
| Retrieved Oocyte number | Exogenous trigger (yes vs no) | 2.04 (1.35-3.08) | 0.0008 | 2.42 (1.53-3.83) | 0.0002 |
| Age (<35 vs 35-39 years) | 1.71 (1.13-2.59) | 0.0117 | - | - | |
| Age (≥40 vs 35-39 years) | 1.28 (0.91-1.79) | 0.1568 | - | - | |
| Infertility duration (years) | - | - | 1.08 (1.02-1.16) | 0.0139 | |
| BMI (kg/m²) | 0.96 (0.92-1.00) | 0.0376 | 0.93 (0.88-0.99) | 0.0176 | |
| Basal FSH (mIU/mL) | 0.97 (0.95-0.98) | <0.0001 | 0.97 (0.95-0.98) | 0.0002 | |
| Decision-day LH (mIU/mL) | 1.01 (1.00-1.02) | 0.0154 | 1.02 (1.01-1.03) | 0.0032 | |
| 2PN | Exogenous trigger (Yes vs No) | 2.32 (1.73-3.11) | <0.0001 | 2.65 (1.91-3.67) | <0.0001 |
| Infertility type (secondary vs primary) | 1.86 (1.33-2.59) | 0.0003 | 2.08 (1.38-3.14) | 0.0004 | |
| BMI (kg/m²) | 0.95 (0.91-0.99) | 0.0240 | - | - | |
| Basal FSH (mIU/mL) | 0.98 (0.96-0.99) | 0.0099 | - | - | |
| Available embryos | Exogenous trigger (Yes vs No) | 2.31 (1.72-3.10) | <0.0001 | 2.72 (1.97-3.78) | <0.0001 |
| Infertility type (secondary vs primary) | 1.56 (1.12-2.16) | 0.0077 | 2.01 (1.34-3.03) | 0.0008 | |
| Basal FSH (mIU/mL) | 0.98 (0.96-1.00) | 0.0118 | - | - | |
| High-quality embryos | Exogenous trigger (Yes vs No) | 3.38 (2.32-4.93) | <0.0001 | 3.78 (2.53-5.67) | <0.0001 |
| Age (<35 vs 35-39 years) | 0.81 (0.52-1.26) | 0.3412 | - | - | |
| Age (≥40 vs 35-39 years) | 0.62 (0.43-0.90) | 0.0108 | - | - | |
| Infertility type (secondary vs primary) | 1.73 (1.14-2.64) | 0.0108 | 2.08 (1.26-3.45) | 0.0044 | |
| Clinical pregnancy | Exogenous trigger (Yes vs No) | 2.95 (1.40-6.24) | 0.0045 | 4.13 (1.86-9.18) | 0.0005 |
| Age (<35 vs 35-39 years) | 0.79 (0.40-1.54) | 0.4882 | 1.14 (0.49-2.62) | 0.7618 | |
| Age (≥40 vs 35-39 years) | 0.25 (0.12-0.50) | 0.0001 | 0.16 (0.07-0.39) | <0.0001 | |
| Infertility type (secondary vs primary) | - | - | 3.97 (1.39-11.31) | 0.0098 | |
| Basal E2 (pg/mL) | 1.00 (1.00-1.01) | 0.0006 | 1.00 (1.00-1.01) | 0.0016 | |
| Live birth | Exogenous trigger (Yes vs No) | 2.94 (1.24-7.00) | 0.0146 | 4.11 (1.64-10.32) | 0.0026 |
| Age (<35 vs 35-39 years) | 1.13 (0.52-2.45) | 0.7535 | 1.31 (0.53-3.22) | 0.5636 | |
| Age (≥40 vs 35-39 years) | 0.13 (0.05-0.34) | <0.0001 | 0.08 (0.02-0.27) | <0.0001 | |
| Infertility type (secondary vs primary) | 3.09 (1.20-7.92) | 0.0191 | 5.90 (1.62-21.53) | 0.0072 | |
| Basal E2 (pg/mL) | 1.00 (1.00-1.01) | 0.0005 | 1.00 (1.00-1.01) | 0.0008 | |
| Subgroup | Clinical outcome | P | OR (95% CI) |
|---|---|---|---|
| Logistic regression | |||
| Age<35 years | Available embryos | 0.0264 | 1.95 (1.08-3.53) |
| High-quality embryos | 0.0009 | 3.99 (1.76-9.04) | |
| Age 35-39 years | Available embryos | 0.0014 | 2.70 (1.47-4.98) |
| High-quality embryos | 0.0045 | 2.68 (1.36-5.30) | |
| Age≥40 years | 2PN | <0.0001 | 2.55 (1.70-3.81) |
| Available embryos | <0.0001 | 2.45 (1.63-3.68) | |
| High-quality embryos | <0.0001 | 3.37 (1.96-5.79) | |
| PSM analysis | |||
| Age <35 years | Available embryos | 0.0171 | 2.29 (1.16-4.51) |
| High-quality embryos | 0.0011 | 4.38 (1.81-10.60) | |
| Age 35-39 years | Retrieved oocyte number | 0.0274 | 2.17 (1.09-4.32) |
| Available embryos | 0.0013 | 3.24 (1.58-6.64) | |
| High-quality embryos | 0.0046 | 2.97 (1.40-6.32) | |
| Clinical pregnancy | 0.0151 | 5.01 (1.37-18.37) | |
| Live birth | 0.0199 | 6.25 (1.34-29.23) | |
| Age≥40 years | 2PN | <0.0001 | 3.18 (2.02-5.00) |
| Available embryos | <0.0001 | 2.84 (1.82-4.43) | |
| High-quality embryos | <0.0001 | 4.25 (2.38-7.60) | |
表5 亚组分析:外源性扳机对临床结局的年龄分层效应
Tab.5 Subgroup analysis: Age-stratified effects of exogenous triggering on clinical outcomes
| Subgroup | Clinical outcome | P | OR (95% CI) |
|---|---|---|---|
| Logistic regression | |||
| Age<35 years | Available embryos | 0.0264 | 1.95 (1.08-3.53) |
| High-quality embryos | 0.0009 | 3.99 (1.76-9.04) | |
| Age 35-39 years | Available embryos | 0.0014 | 2.70 (1.47-4.98) |
| High-quality embryos | 0.0045 | 2.68 (1.36-5.30) | |
| Age≥40 years | 2PN | <0.0001 | 2.55 (1.70-3.81) |
| Available embryos | <0.0001 | 2.45 (1.63-3.68) | |
| High-quality embryos | <0.0001 | 3.37 (1.96-5.79) | |
| PSM analysis | |||
| Age <35 years | Available embryos | 0.0171 | 2.29 (1.16-4.51) |
| High-quality embryos | 0.0011 | 4.38 (1.81-10.60) | |
| Age 35-39 years | Retrieved oocyte number | 0.0274 | 2.17 (1.09-4.32) |
| Available embryos | 0.0013 | 3.24 (1.58-6.64) | |
| High-quality embryos | 0.0046 | 2.97 (1.40-6.32) | |
| Clinical pregnancy | 0.0151 | 5.01 (1.37-18.37) | |
| Live birth | 0.0199 | 6.25 (1.34-29.23) | |
| Age≥40 years | 2PN | <0.0001 | 3.18 (2.02-5.00) |
| Available embryos | <0.0001 | 2.84 (1.82-4.43) | |
| High-quality embryos | <0.0001 | 4.25 (2.38-7.60) | |
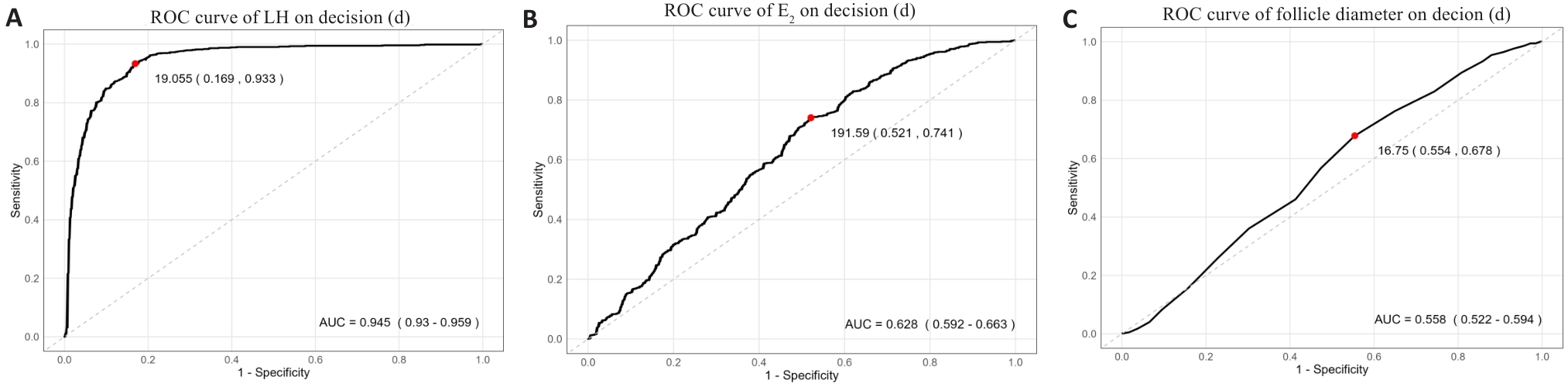
图1 ROC曲线
Fig.1 Receiver operating characteristic (ROC) curves of decision-day biomarkers for optimal trigger strategy selection. A: LH levels (AUC=0.945, 95% CI: 0.93-0.959). B: Estradiol (E₂) levels (AUC=0.628, 95% CI: 0.592-0.663). C: Follicle diameter (AUC=0.558, 95% CI: 0.522-0.594). The optimal cutoff values are indicated by red points: 19.055 mIU/mL for LH (sensitivity 93.3%, specificity 93.1%); 191.59 pg/mL for E₂ (sensitivity 74.1%, specificity 47.9%); 16.75 mm for follicle diameter (sensitivity 67.8%, specificity 44.6%). Dashed diagonal lines represent reference (no discrimination; AUC=0.5).
| [1] | Steptoe PC, Edwards RG. Birth after the reimplantation of a human embryo[J]. Lancet, 1978, 312(8085): 366. doi:10.1016/s0140-6736(78)92957-4 |
| [2] | Baker VL, Dyer S, Chambers GM, et al. International committee for monitoring assisted reproductive technologies (ICMART): world report for cycles conducted in 2017-2018[J]. Hum Reprod, 2025, 40(6): 1110-26. doi:10.1093/humrep/deaf049 |
| [3] | Allersma T, Farquhar C, Cantineau AE. Natural cycle in vitro fertilisation (IVF) for subfertile couples[J]. Cochrane Database Syst Rev, 2013(8): CD010550. doi:10.1002/14651858.cd010550.pub2 |
| [4] | von Wolff M. The role of Natural Cycle IVF in assisted reproduction[J]. Best Pract Res Clin Endocrinol Metab, 2019, 33(1): 35-45. doi:10.1016/j.beem.2018.10.005 |
| [5] | Bodri D, Kawachiya S, Kondo M, et al. Oocyte retrieval timing based on spontaneous luteinizing hormone surge during natural cycle in vitro fertilization treatment[J]. Fertil Steril, 2014, 101(4): 1001-7. doi:10.1016/j.fertnstert.2014.01.016 |
| [6] | Tian T, Li Y, Lv J, et al. The potential influence of follicle diameter on natural cycle in vitro fertilization among women with diminished ovarian reserve: a retrospective cohort study[J]. J Ovarian Res, 2023, 16(1): 195. doi:10.1186/s13048-023-01281-4 |
| [7] | Reichman DE, Zakarin L, Chao K, et al. Diminished ovarian reserve is the predominant risk factor for gonadotropin-releasing hormone antagonist failure resulting in breakthrough luteinizing hormone surges in in vitro fertilization cycles[J]. Fertil Steril, 2014, 102(1): 99-102. doi:10.1016/j.fertnstert.2014.04.010 |
| [8] | Lenton EA. Natural cycle IVF with and without terminal HCG: learning from failed cycles[J]. Reprod BioMedicine Online, 2007, 15(2): 149-55. doi:10.1016/S1472-6483(10)60702-X |
| [9] | Gordon JD, DiMattina M, Reh A, et al. Utilization and success rates of unstimulated in vitro fertilization in the United States: an analysis of the Society for Assisted Reproductive Technology database[J]. Fertil Steril, 2013, 100(2): 392-5. doi:10.1016/j.fertnstert.2013.03.037 |
| [10] | Di Guardo F, Blockeel C, De Vos M, et al. Poor ovarian response and the possible role of natural and modified natural cycles[J]. Ther Adv Reprod Health, 2022, 16: 26334941211062026. doi:10.1177/26334941211062026 |
| [11] | Alpha Scientists in Reproductive Medicine and ESHRE Special Interest Group of Embryology. The Istanbul consensus workshop on embryo assessment: proceedings of an expert meeting[J]. Hum Reprod, 2011, 26(6): 1270-83. doi:10.1016/j.rbmo.2011.02.001 |
| [12] | Kochhar PK, Ghosh P. Diminished ovarian reserve predisposes to premature luteinizing hormone surges in gonadotropin-releasing hormone antagonist cycles in In vitro fertilization[J]. J Hum Reprod Sci, 2020, 13(3): 191-5. doi:10.4103/jhrs.jhrs_133_19 |
| [13] | Zhu Q, Li Y, Ma J, et al. Potential factors result in diminished ovarian reserve: a comprehensive review[J]. J Ovarian Res, 2023, 16(1): 208. doi:10.1186/s13048-023-01296-x |
| [14] | Hanson BM, Tao X, Zhan Y, et al. Young women with poor ovarian response exhibit epigenetic age acceleration based on evaluation of white blood cells using a DNA methylation-derived age prediction model[J]. Hum Reprod, 2020, 35(11): 2579-88. doi:10.1093/humrep/deaa206 |
| [15] | Lebovitz O, Haas J, Mor N, et al. Predicting IVF outcome in poor ovarian responders[J]. BMC Womens Health, 2022, 22(1): 395. doi:10.1186/s12905-022-01964-y |
| [16] | Tiwari M, Chaube SK. Human chorionic gonadotropin mediated generation of reactive oxygen species is sufficient to induce meiotic exit but not apoptosis in rat oocytes[J]. Biores Open Access, 2017, 6(1): 110-22. doi:10.1089/biores.2017.0018 |
| [17] | Wang S, He G, Chen M, et al. The role of antioxidant enzymes in the ovaries[J]. Oxid Med Cell Longev, 2017, 2017: 4371714. doi:10.1155/2017/4371714 |
| [18] | Yano S, Ishiuchi T, Abe S, et al. Histone H3K36me2 and H3K36me3 form a chromatin platform essential for DNMT3A-dependent DNA methylation in mouse oocytes[J]. Nat Commun, 2022, 13(1): 4440. doi:10.1038/s41467-022-32141-2 |
| [19] | Uysal F, Sukur G, Bozdemir N, et al. Unveiling the impact of DNA methylation machinery: Dnmt1 and Dnmt3a in orchestrating oocyte development and cellular homeostasis[J]. Genesis, 2024, 62(1): e23579. doi:10.1002/dvg.23579 |
| [20] | Ai J, Jin L, Zheng Y, et al. The morphology of inner cell mass is the strongest predictor of live birth after a frozen-thawed single embryo transfer[J]. Front Endocrinol: Lausanne, 2021, 12: 621221. doi:10.3389/fendo.2021.621221 |
| [21] | von Wolff M, Kollmann Z, Flück CE, et al. Gonadotrophin stimulation for in vitro fertilization significantly alters the hormone milieu in follicular fluid: a comparative study between natural cycle IVF and conventional IVF[J]. Hum Reprod, 2014, 29(5): 1049-57. doi:10.1093/humrep/deu044 |
| [22] | Polyzos NP, Drakopoulos P, Tournaye H. Modified natural cycle IVF for poor ovarian responders: rethink before concluding[J]. Hum Reprod, 2016, 31(1): 221-2. doi:10.1093/humrep/dev272 |
| [23] | Ho JR, Paulson RJ. Modified natural cycle in in vitro fertilization[J]. Fertil Steril, 2017, 108(4): 572-6. doi:10.1016/j.fertnstert.2017.08.021 |
| [24] | Rackow BW, Kliman HJ, Taylor HS. GnRH antagonists may affect endometrial receptivity[J]. Fertil Steril, 2008, 89(5): 1234-9. doi:10.1016/j.fertnstert.2007.04.060 |
| [25] | Orvieto R, Meltzer S, Rabinson J, et al. GnRH agonist versus GnRH antagonist in ovarian stimulation: the role of endometrial receptivity[J]. Fertil Steril, 2008, 90(4): 1294-6. doi:10.1016/j.fertnstert.2007.10.022 |
| [26] | Xu B, Geerts D, Hu S, et al. The depot GnRH agonist protocol improves the live birth rate per fresh embryo transfer cycle, but not the cumulative live birth rate in normal responders: a randomized controlled trial and molecular mechanism study[J]. Hum Reprod, 2020, 35(6): 1306-18. doi:10.1093/humrep/deaa086 |
| [1] | 张庆颜, 张 俊, 周星宇, 黎 莹, 陈映雪, 陈 薪, 陈士岭. 高龄不孕症患者冻融胚胎移植胚胎数目和质量与早期妊娠丢失率的关系[J]. 南方医科大学学报, 2021, 41(7): 1050-1055. |
| [2] | 吴晓敏, 陈映雪, 周星宇, 张 俊, 黎 莹, 李 欣, 张笑菲, 陈士岭. 卵泡发育中晚期添加HMG可改善妊娠结局:基于682例高龄卵巢储备减退患者[J]. 南方医科大学学报, 2021, 41(3): 412-417. |
| [3] | 谢多,邱卓琳,罗琛,褚庆军,全松. ICSI 中不同来源精子对卵母细胞受精、胚胎质量及发育潜能的影响[J]. 南方医科大学学报, 2014, 34(06): 857-. |
| [4] | 陈士岭,罗燕群,夏容,陈薪,施晓鋆,郑海燕,王乐乐,吴雅琴. 年轻妇女基础FSH 高水平与卵子和胚胎的数量、质量及临床结局的关系[J]. 南方医科大学学报, 2011, 31(05): 777-. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||